Urinary proteomics identifies distinct immunological profiles of sepsis associated AKI sub-phenotypes
- PMID: 39695715
- PMCID: PMC11654061
- DOI: 10.1186/s13054-024-05202-9
Urinary proteomics identifies distinct immunological profiles of sepsis associated AKI sub-phenotypes
Abstract
Background: Patients with sepsis-induced AKI can be classified into two distinct sub-phenotypes (AKI-SP1, AKI-SP2) that differ in clinical outcomes and response to treatment. The biologic mechanisms underlying these sub-phenotypes remains unknown. Our objective was to understand the underlying biology that differentiates AKI sub-phenotypes and associations with kidney outcomes.
Methods: We prospectively enrolled 173 ICU patients with sepsis from a suspected respiratory infection (87 without AKI and 86 with AKI on enrollment). Among the AKI patients, 66 were classified as AKI-SP1 and 20 as AKI-SP2 using a three-plasma biomarker classifier. Aptamer-based proteomics assessed 5,212 proteins in urine collected on ICU admission. We compared urinary protein abundances between AKI sub-phenotypes, conducted pathway analyses, tested associations with risk of RRT and blood bacteremia, and predicted AKI-SP2 class membership using LASSO.
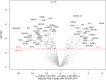
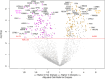
Measurement and main results: In total, 117 urine proteins were higher in AKI-SP2, 195 were higher in AKI-SP1 (FDR < 0.05). Urinary proteins involved in inflammation and chemoattractant of neutrophils and monocytes (CXCL1 and REG3A) and oxidative stress (SOD2) were abundant in AKI-SP2, while proteins involved in collagen deposition (GP6), podocyte derived (SPOCK2), proliferation of mesenchymal cells (IL11RA), anti-inflammatory (IL10RB and TREM2) were abundant in AKI-SP1. Pathways related to immune response, complement activation and chemokine signaling were upregulated in AKI-SP2 and pathways of cell adhesion were upregulated in AKI-SP1. Overlap was present between urinary proteins that differentiated AKI sub-phenotypes and proteins that differentiated risk of RRT during hospitalization. Variable correlation was found between top aptamers and ELISA based protein assays. A LASSO derived urinary proteomic model to classify AKI-SP2 had a mean AUC of 0.86 (95% CI: 0.69-0.99).
Conclusion: Our findings suggest AKI-SP1 is characterized by a reparative, regenerative phenotype and AKI-SP2 is characterized as an immune and inflammatory phenotype associated with blood bacteremia. We identified shared biology between AKI sub-phenotypes and eventual risk of RRT highlighting potential therapeutic targets. Urine proteomics may be used to non-invasively classify SP2 participants.
Keywords: Acute kidney injury; Intensive care unit; Sepsis; Urinary proteomics.
© 2024. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: The University of Washington institutional review board approved this study. Consent for publication: No individual personal data is included in the study. The IRB provided waiver of consent to participate in this study. Competing interests: There are no conflicts of interest among the authors of this manuscript.
Figures

Comment in
-
Urinary proteomics in sepsis-associated AKI.Crit Care. 2025 Feb 16;29(1):77. doi: 10.1186/s13054-025-05306-w. Crit Care. 2025. PMID: 39956897 Free PMC article. No abstract available.
References
-
- Uchino S, Kellum JA, Bellomo R, et al. Acute renal failure in critically ill patients: a multinational, multicenter study. JAMA. 2005;294:813–8. - PubMed
-
- Joannidis M, Metnitz PGH. Epidemiology and natural history of acute renal failure in the ICU. Crit Care Clin. 2005;21:239–49. - PubMed
-
- Hoste EAJ, Bagshaw SM, Bellomo R, Cely CM, Colman R, Cruz DN, et al. Epidemiology of acute kidney injury in critically ill patients: the multinational AKI-EPI study. Intensive Care Med. 2015;41:1411–23. - PubMed
-
- Clermont G, Acker CG, Angus DC, Sirio CA, Pinsky MR, Johnson JP. Renal failure in the ICU: comparison of the impact of acute renal failure and end-stage renal disease on ICU outcomes. Kidney Int. 2002;62:986–96. - PubMed
-
- Bellomo R, Kellum JA, Ronco C. Acute kidney injury. Lancet Lond Engl. 2012;380:756–66. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

