Effect of panretinal photocoagulation versus intravitreal bevacizumab injection on optic disc microcirculation in patients with diabetic retinopathy
- PMID: 39695775
- PMCID: PMC11656866
- DOI: 10.1186/s40942-024-00621-w
Effect of panretinal photocoagulation versus intravitreal bevacizumab injection on optic disc microcirculation in patients with diabetic retinopathy
Abstract
Background: This retrospective study aimed to compare optic disc vasculature changes in 1 and 3 months after treatment with either panretinal photocoagulation (PRP) or Intravitreal bevacizumab (IVB) in patients with diabetic retinopathy.
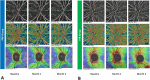
Methods: A total of 50 eyes of 29 diabetic patients without severe complications were included in this comparative case series. Of these, twenty-eight eyes (15 patients) were assigned to the PRP group, while twenty-two eyes (14 patients) were treated with the biosimilar (IVB) (Stivant® CinnaGen Co., Iran). Optical tomography angiography (OCTA) was performed to measure optic disc vascular density (VD) as well as retinal nerve fiber layer (RNFL) thickness.
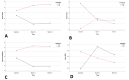
Results: The mean age of the enrolled patients was 62.1 ± 8.3 years (40 to 78 years). During follow-up, whole disc VD, inside disc VD and peripapillary VD decreased significantly in the PRP group at month 1 (p = 0.032, p = 0.32, and p = 0.016, respectively) and month 3 (p = 0.004, p = 0.001 and p = 0.011, respectively). There was an insignificant and slight increase for these parameters in the IVB group. (p > 0.05 for all) A comparison of two treatment arms based on mean whole disc VD, inside disc VD, and peripapillary VD changes revealed a significant difference at month 1 (p = 0.009, p = 0.019, and p = 0.002, respectively) and month 3 (p = 0.002, p = 0.015, and p = 0.009, respectively). Peripapillary RNFL thickness increased in the PRP group at month 1 (p = 0.002) and then decreased at month 3 (p = 0.001). During three months of follow-up, the peripapillary RNFL thickness decreased significantly in the IVB group (p = 0.001). Peripapillary RNFL thickness changes were significantly different between treatment groups at month 1 and month 3. (p = 0.001 for both) The RNFL changes during the study did not significantly correlate with peripapillary VD changes in each group (p = 0.231 and p = 372, for PRP and IVB group, respectively).
Conclusion: This study demonstrated that IVB and PRP treatments produced distinct short-term microvascular changes in the optic nerve of diabetic retinopathy patients. PRP treatment significantly reduced vascular density in the optic disc and peripapillary region over 3 months, with an initial increase in RNFL thickness followed by a decrease by month 3. In contrast, IVB treatment led to a slight increase in optic disc vascular density while significantly reducing RNFL thickness. No significant correlation was found between changes in RNFL thickness and peripapillary vascular density within either treatment group.
Keywords: Anti-vascular endothelial growth factor (anti-VEGF); Diabetic retinopathy; Optical coherence tomography angiography (OCTA); Panretinal photocoagulation (PRP); Retinal nerve fiber layer (RNFL) thickness; Vascular density.
© 2024. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: This study has been approved by the local institutional review board of Tehran University of Medical Sciences (IR.TUMS.FARABIH.REC.1400.038). The study was performed in accordance with the Helsinki Declaration of 1964, and its later amendments; All patients provided informed consent to participate in the study. Consent for publication: Written informed consents were obtained from each participant. Competing interests: The authors declare no competing interests.
Figures
References
-
- Gross JG, Glassman AR, Liu D, Sun JK, Antoszyk AN, Baker CW, Bressler NM, Elman MJ, Ferris FL, Gardner TW. Five-year outcomes of panretinal photocoagulation vs intravitreous ranibizumab for proliferative diabetic retinopathy: a randomized clinical trial. JAMA Ophthalmol. 2018;136(10):1138–48. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Research Materials

