A Case of Fibrolamellar Hepatocellular Carcinoma in Which Tumor Control Was Achieved by Re-Administering Atezolizumab and Bevacizumab
- PMID: 39702734
- PMCID: PMC11659117
- DOI: 10.1002/cnr2.70090
A Case of Fibrolamellar Hepatocellular Carcinoma in Which Tumor Control Was Achieved by Re-Administering Atezolizumab and Bevacizumab
Abstract
Background: Fibrolamellar hepatocellular carcinoma (FL-HCC) clinically occurs in young people aged 20-30 years, who often have a normal liver background. We propose a treatment for such cases in which a combination therapy of atezolizumab and bevacizumab is followed by sandwiching radiation therapy to release tumor antigens and then re-administering the combination therapy of atezolizumab and bevacizumab (ABC conversion therapy).
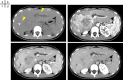
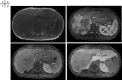
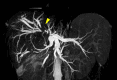
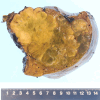
Case: The patient is a 15-year-old girl. On April 18, 2022, she noticed skin yellowing and visited her local doctor. Computed tomography (CT) revealed a large mass in the right lobe of the liver and bile duct obstruction due to the tumor. She also had a nodule on her chest that appeared to be a metastatic tumor and was referred to Kinki University Hospital in April 2023. She was suspected to have FL-HCC based on contrast-enhanced ultrasound and CT scan results. There were findings suggestive of lung metastasis; however, she underwent a right hepatic lobectomy on May 17, 2023, considering the risk of liver failure and intra-abdominal bleeding due to the large liver tumor. A CT scan conducted on July 25, 2022, showing increased lung metastases, and she started atezolizumab/bevacizumab combination treatment on October 20, 2022. On March 15, 2023, multiple lung metastases and new intrahepatic lesions appeared, which was diagnosed as progressive disease (PD), and lenvatinib was discontinued. On November 17, 2023, radiation therapy (25 Gy/5 Fr) was administered to the lung and intrahepatic lesions to release tumor antigens, and on November 27, 2023, atezolizumab and bevacizumab combination treatment was resumed to control the tumor.
Conclusion: Combination therapy with atezolizumab, bevacizumab, and radiation therapy may be an option for the treatment of FL-HCC.
Keywords: atezolizumab; bevacizumab; combination therapy; fibrolamellar hepatocellular carcinoma; radiation therapy.
© 2024 The Author(s). Cancer Reports published by Wiley Periodicals LLC.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures



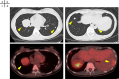


References
-
- Edmondson H. A., “Differential Diagnosis of Tumors and Tumor‐Like Lesions of Liver in Infancy and Childhood,” AMA Journal of Diseases of Children 91 (1956): 168–186. - PubMed
-
- Chaudhari V. A., Khobragade K., Bhandare M., and Shrikhande S. V., “Management of Fibrolamellar Hepatocellular Carcinoma,” Chinese Clinical Oncology 7 (2018): 51. - PubMed
-
- Kudo M., Aoki T., Ueshima K., et al., “Achievement of Complete Response and Drug‐Free Status by Atezolizumab Plus Bevacizumab Combined With or Without Curative Conversion in Patients With Transarterial Chemoembolization‐Unsuitable, Intermediate‐Stage Hepatocellular Carcinoma: A Multicenter Proof‐Of‐Concept Study,” Liver Cancer 12 (2023): 321–338. - PMC - PubMed
Publication types
MeSH terms
Substances
Supplementary concepts
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

