Design and rationale of the eLym™ System for Decompensation of Excess Lymphatic Fluid via the Thoracic Duct in Acute Heart Failure (DELTA-HF)
- PMID: 39716986
- PMCID: PMC12055369
- DOI: 10.1002/ehf2.15192
Design and rationale of the eLym™ System for Decompensation of Excess Lymphatic Fluid via the Thoracic Duct in Acute Heart Failure (DELTA-HF)
Abstract
Aims: The interstitial space is the major compartment in which the excess fluid is located, forming peripheral congestion in acute decompensated heart failure (ADHF). The lymphatic system is responsible for the constant drainage of the compartment. In ADHF, the inefficiency of this system causes extravascular fluid accumulation, underscoring the crucial role of lymphatic system failure in ADHF's pathophysiology. The eLym™ System is a transcutaneous device designed to facilitate lymph drainage by creating a low-pressure zone in the thoracic duct area, theoretically allowing more efficient decompression of the lymphatic system.
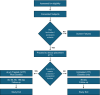
Methods and results: The safety and feasibility of the eLym™ System for the Decongestion of Excess Lymphatic Fluid via the Thoracic Duct in Acute Decompensated Heart Failure: DELTA-HF Study is a prospective, multicentre, single-arm study designed to evaluate the safety and feasibility of the WhiteSwell eLym™ System in the treatment of fluid overload in ADHF. A maximum of 50 subjects may be enrolled and undergo the treatment. Inclusion criteria include the presence of congestion, a home diuretic dose ≥80 mg furosemide (or equivalent) and elevated natriuretic peptides. The key exclusion criteria include anatomical abnormalities and the inability to undergo systemic anticoagulation. The study endpoints include the safety (short- and long-term) and feasibility of the procedure. Several congestion indexes will be prospectively assessed. Descriptive statistics will summarize the study results. The study was registered in clinicaltrial.gov (NCT05747196).
Conclusions: The results of the DELTA-HF study will provide information about the safety and feasibility of the eLym™ System and will provide first-in-human clinical signals of its use in ADHF patients.
Keywords: acute heart failure; decongestion; lymphatic system.
© 2024 The Author(s). ESC Heart Failure published by John Wiley & Sons Ltd on behalf of European Society of Cardiology.
Conflict of interest statement
J. B. has received honoraria from Bayer, Boehringer Ingelheim and AstraZeneca for lectures and Alleviant Medical and WhiteSwell for participating in clinical trial advisory boards. J. B. is a member of the Editorial Board of ESC Heart Failure and Heart Failure Reviews.
Figures


Similar articles
-
Direct Interstitial Decongestion in an Animal Model of Acute-on-Chronic Ischemic Heart Failure.JACC Basic Transl Sci. 2021 Nov 22;6(11):872-881. doi: 10.1016/j.jacbts.2021.09.008. eCollection 2021 Nov. JACC Basic Transl Sci. 2021. PMID: 34869951 Free PMC article.
-
Lymphatic Drainage in Patients with Heart Failure: A Feasibility Study.J Cardiovasc Transl Res. 2025 Apr;18(2):291-294. doi: 10.1007/s12265-025-10592-4. Epub 2025 Feb 3. J Cardiovasc Transl Res. 2025. PMID: 39900887
-
A Phenomapping Tool and Clinical Score to Identify Low Diuretic Efficiency in Acute Decompensated Heart Failure.JACC Heart Fail. 2024 Mar;12(3):508-520. doi: 10.1016/j.jchf.2023.09.029. Epub 2023 Dec 13. JACC Heart Fail. 2024. PMID: 38099890
-
The interstitial compartment as a therapeutic target in heart failure.Front Cardiovasc Med. 2022 Aug 17;9:933384. doi: 10.3389/fcvm.2022.933384. eCollection 2022. Front Cardiovasc Med. 2022. PMID: 36061549 Free PMC article. Review.
-
Role of Lymphatics in Heart Failure.J Soc Cardiovasc Angiogr Interv. 2023 Dec 4;2(6Part B):101204. doi: 10.1016/j.jscai.2023.101204. eCollection 2023 Nov-Dec. J Soc Cardiovasc Angiogr Interv. 2023. PMID: 39131069 Free PMC article. Review.
Cited by
-
Gut microbiota's role in heart failure.Heart Fail Rev. 2025 Jul 9. doi: 10.1007/s10741-025-10543-w. Online ahead of print. Heart Fail Rev. 2025. PMID: 40629225 Review.
-
Lower extremity lymphatic flow is associated with diuretic response in acute heart failure.Eur J Heart Fail. 2025 Jun;27(6):1136-1144. doi: 10.1002/ejhf.3655. Epub 2025 Apr 7. Eur J Heart Fail. 2025. PMID: 40194929 Free PMC article.
References
-
- Ambrosy AP, Cerbin LP, Armstrong PW, Butler J, Coles A, DeVore AD, et al. Body weight change during and after hospitalization for acute heart failure: patient characteristics, markers of congestion, and outcomes: findings from the ASCEND‐HF trial. JACC Heart Fail 2017;5:1‐13. doi:10.1016/j.jchf.2016.09.012 - DOI - PMC - PubMed
Publication types
MeSH terms
Associated data
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

