Primary and revision myringoplasty in children: Long-term outcome and analysis of the factors influencing the results
- PMID: 39720117
- PMCID: PMC11665936
- DOI: 10.1016/j.joto.2024.04.001
Primary and revision myringoplasty in children: Long-term outcome and analysis of the factors influencing the results
Abstract
Objective: Assess the long-term outcome of pediatric myringoplasty.
Methods: Tympanoplasty type I, myringoplasty, was performed on 85 children (91 consecutive operations, 74 primary and 17 revisions) under 16 years of age. The perforations were sequela either to acute or chronic inflammatory middle ear disease. Medial grafting technique was employed with temporalis fascia. Adenoidectomy was performed earlier on all but five children. The preoperative observation period exceeded one year for all patients. The mean follow-up was 5.4 (SD 3.6) years.
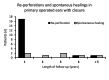
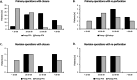
Results: The long-term graft take rate was 84% for primary myringoplasty, and 53% for revision operations. The re-perforations were associated with postoperative discharge, subtotal or total perforation and revision surgery. In the cohort, sixty ears (66%) were completely healthy (intact tympanic membrane in normal position without adhesions and with good mobility) after follow-up. Spontaneous healing took place in 37% after re-perforation. The preoperative ventilation tube treatment did not affect the outcome and there were no differences between age groups. Preoperative sonotubometry or Valsalva test results did not correlate with outcome. Four ears needed a ventilation tube during the follow-up due to poor ventilation. The mean pure tone thresholds improved significantly after operation.
Conclusions: Myringoplasty in children is a reliable procedure without age restrictions. One year of preoperative observation excludes most unstable ears, and high tendency of spontaneous healing after re-perforation suggests the need for a lengthy follow-up before revision surgery.
Keywords: Middle ear; Myringoplasty; Pediatric; Surgery.
© [copyright 2024] PLA General Hospital Department of Otolaryngology Head and Neck Surgery. Production and hosting by Elsevier (Singapore) Pte Ltd.
Figures
Similar articles
-
Pediatric myringoplasty: A study of effectiveness and influencing factors.Int J Pediatr Otorhinolaryngol. 2022 Feb;153:110990. doi: 10.1016/j.ijporl.2021.110990. Epub 2021 Nov 24. Int J Pediatr Otorhinolaryngol. 2022. PMID: 34973522
-
Pediatric partial gelfoam myringoplasty with ventilation tube placement.Int J Pediatr Otorhinolaryngol. 2019 Nov;126:109632. doi: 10.1016/j.ijporl.2019.109632. Epub 2019 Aug 9. Int J Pediatr Otorhinolaryngol. 2019. PMID: 31419743
-
Long-Term Follow-Up After Fat Graft Myringoplasty: Do Size and Location Matter?Ear Nose Throat J. 2021 Jun;100(3_suppl):229S-234S. doi: 10.1177/0145561320973555. Epub 2020 Dec 14. Ear Nose Throat J. 2021. PMID: 33314958
-
Butterfly myringoplasty for total, subtotal, and annular perforations.Laryngoscope. 2016 Nov;126(11):2565-2568. doi: 10.1002/lary.25904. Epub 2016 Jul 14. Laryngoscope. 2016. PMID: 27411314
-
Circumferential subannular tympanoplasty: surgical and hearing outcome in 224 ears with subtotal perforation.Acta Otolaryngol. 2022 Mar-Apr;142(3-4):254-258. doi: 10.1080/00016489.2022.2042596. Epub 2022 Mar 2. Acta Otolaryngol. 2022. PMID: 35235490 Review.
References
-
- Abood A., Torzynski B., Ovesen T. Pediatric type 1 tympanoplasty – does age matter? Int. J. Pediatr. Otorhinolaryngol. 2020 - PubMed
-
- Alho O.-P., Oja H., Koivu M., Sorri M. Chronic otitis media with effusion in infancy. Arch. Otolaryngol. Head Neck Surg. 1995;121:432–436. - PubMed
-
- Berger G., Shapira A., Marshak G. Myringoplasty in children. J. Otolaryngol. 1983;12:228–230. - PubMed
-
- Black J.H., Hickey S.A., Wormald P.J. An analysis of the results of myringoplasty in children. Int. J. Pediatr. Otorhinolaryngol. 1995;31:95–100. - PubMed
-
- Blanshard J., Robson A., Smith I., Maw A.R. A long term view of myringoplasty in children. J. Laryngol. Otol. 1990;104:758–762. - PubMed
LinkOut - more resources
Full Text Sources