NLRP3 Inflammasome Activation and Altered Mitophagy Are Key Pathways in Inclusion Body Myositis
- PMID: 39723571
- PMCID: PMC11669947
- DOI: 10.1002/jcsm.13672
NLRP3 Inflammasome Activation and Altered Mitophagy Are Key Pathways in Inclusion Body Myositis
Abstract
Background: Inclusion body myositis (IBM) is the most prevalent muscle disease in adults for which no current treatment exists. The pathogenesis of IBM remains poorly defined. In this study, we aimed to explore the interplay between inflammation and mitochondrial dysfunction in IBM.
Methods: The study population consisted of 38 IBM patients and 22 age- and sex-matched controls without a myopathy. Mean age was 62.9 years (SD = 9) in IBM group and 59.7 (10) in controls. Bulk RNA sequencing, Meso Scale Discovery electrochemiluminescence (ECL), western blotting, histochemistry and immunohistochemistry were performed on frozen muscle samples from the study participants.
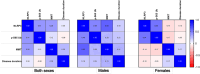
Results: We demonstrated activation of the NLRP3 inflammasome in IBM muscle samples, with the NLRP3 inflammasome being the most upregulated pathway on RNA sequencing, along with increased expression of NLRP3 and ASC proteins in IBM group. NLRP3 RNA levels most strongly correlated with TLR7 (correlation coefficient ρ = 0.91) and complement activation-related genes, and inversely correlated with several mitochondria-related genes among others. On muscle histopathology, there was increased NRLP3 immunoreactivity in both inflammatory cells and muscle fibres. Mitophagy is critical for removing damaged mitochondria and preventing the formation of a vicious cycle of mitochondrial dysfunction-NLRP3 inflammasome activation. Herein, we showed altered mitophagy, as witnessed by the elevated levels of p-S65-Ubiquitin, a mitophagy marker, in muscle lysates from IBM patients compared to controls (median of 114.3 vs. 81.25 ECL units, p = 0.005). The p-S65-Ubiquitin levels were most significantly elevated in IBM males compared to male controls (136 vs. 83.5 ECL units; p = 0.013), whereas IBM females had milder nonsignificant elevation compared to female controls (97.25 vs. 69 ECL units, p = 0.31). On muscle histopathology, p-S65-Ubiquitin aggregates accumulated in muscle fibres that were mostly Type 2 and devoid of cytochrome-c-oxidase reactivity. NLRP3 RNA levels correlated with p-S65-Ubiquitin levels in both sexes (males: ρ = 0.48, females: ρ = 0.54) but with loss of muscle strength, as reflected by the manual motor test score, only in males (males: ρ = 0.62, females: ρ = -0.14). Lastly, we identified sex-specific molecular pathways in IBM. Females had upregulation of pathways related to response to stress, which could conceivably offset some of the pathomechanisms of IBM, while males had upregulation of pathways related to cell adhesion and migration.
Conclusions: There is activation of the NLRP3 inflammasome in IBM, along with altered mitophagy, particularly in males, which is of potential therapeutic significance. These findings suggest sex-specific mechanisms in IBM that warrant further investigation.
Keywords: autophagy; inclusion body myositis; inflammasome; mitochondrial dysfunction; mitophagy.
© 2024 The Author(s). Journal of Cachexia, Sarcopenia and Muscle published by Wiley Periodicals LLC.
Conflict of interest statement
Mayo Clinic, F. C. F. and W. S. have filed a patent related to PRKN mitophagy activators. All other authors report no conflicts of interest.
Figures




Update of
-
NLRP3 inflammasome activation and altered mitophagy are key pathways in inclusion body myositis.medRxiv [Preprint]. 2024 Jun 16:2024.06.15.24308845. doi: 10.1101/2024.06.15.24308845. medRxiv. 2024. Update in: J Cachexia Sarcopenia Muscle. 2025 Feb;16(1):e13672. doi: 10.1002/jcsm.13672. PMID: 38947067 Free PMC article. Updated. Preprint.
References
-
- Greenberg S. A., Pinkus J. L., Kong S. W., Baecher‐Allan C., Amato A. A., and Dorfman D. M., “Highly Differentiated Cytotoxic T Cells in Inclusion Body Myositis,” Brain 142 (2019): 2590–2604. - PubMed
-
- Callan A., Capkun G., Vasanthaprasad V., Freitas R., and Needham M., “A Systematic Review and Meta‐Analysis of Prevalence Studies of Sporadic Inclusion Body Myositis,” Journal of Neuromuscular Diseases 4 (2017): 127–137. - PubMed
-
- Dahlbom K., Lindberg C., and Oldfors A., “Inclusion Body Myositis: Morphological Clues to Correct Diagnosis,” Neuromuscular Disorders 12 (2002): 853–857. - PubMed
MeSH terms
Substances
Grants and funding
- AARF-22-973152/APDA and Alzheimer's Association
- Michael J. Fox Foundation for Parkinson's Research
- 22A07/Florida Department of Health
- Mayo Clinic Foundation
- Mayo Clinic Center for Clinical and Translational Sciences
- U54 NS110435/NS/NINDS NIH HHS/United States
- Ted Nash Long Life Foundation
- RF1AG55549/NH/NIH HHS/United States
- K08-AR78254/National Institute of Arthritis, Musculoskeletal and Skins Diseases
- American Neuromuscular Foundation
- K08 AR078254/AR/NIAMS NIH HHS/United States
- Mayo Clinic Center for Biomedical Discovery
- Mayo Clinic Robert and Arlene Kogod Center on Aging
- RF1 NS085070/NS/NINDS NIH HHS/United States
- RF1 AG055549/AG/NIA NIH HHS/United States
- R01 NS110085/NS/NINDS NIH HHS/United States
- P30 AG062677/AG/NIA NIH HHS/United States
LinkOut - more resources
Full Text Sources
Miscellaneous

