Simplifying coronary artery disease risk stratification: development and validation of a questionnaire-based alternative comparable to clinical risk tools
- PMID: 39724785
- PMCID: PMC11732493
- DOI: 10.1016/j.ebiom.2024.105518
Simplifying coronary artery disease risk stratification: development and validation of a questionnaire-based alternative comparable to clinical risk tools
Abstract
Background: Coronary artery disease (CAD) comprises one of the leading causes of morbidity and mortality both in the European population and globally. All established clinical risk stratification scores and models require blood lipids and physical measurements. The latest reports of the European Commission suggest that attracting health professionals to collect these data can be challenging, both from a logistic and cost perspective, which limits the usefulness of established models and makes them unsuitable for population-wide screening in resource-limited settings, i.e., rural areas. Therefore, the aim of this study was to develop and externally validate a questionnaire-based risk stratification model on a population scale at minimal cost, i.e., the Questionnaire-Based Evaluation for Estimating Coronary Artery Disease (QUES-CAD) to stratify the 10-year incidence of coronary artery disease.
Methods: Cox proportional hazards (CoxPH) and Cox gradient boosting (CoxGBT) models were trained with 10-fold cross-validation using combinations of ten questionnaire variables on the White population of the UK Biobank (n = 448,818) and internally validated the models in all ethnic minorities (n = 27,433). The Lifelines cohort was employed as an independent external validation population (n = 97,770). Additionally, we compared QUES-CAD's performance, containing only questionnaire variables, to clinically established risk prediction tools, i.e., Framingham Coronary Heart Disease Risk Score, American College of Cardiology/American Heart Association pooled cohort equation, World Health Organization cardiovascular disease risk charts, and Systematic Coronary Risk Estimation 2 (SCORE2). We conducted partial log-likelihood ratio (PLR) tests and C-index comparisons between QUES-CAD and established clinical prediction models.
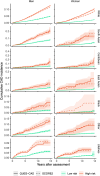
Findings: In the external validation set, QUES-CAD exhibited C-index values of CoxPH: 0.692 (95% Confidence Interval [CI]: 0.673-0.71) and CoxGBT: 0.699 (95% CI: 0.681-0.717) for the male population and CoxPH: 0.771 (95% CI: 0.748-0.794) and CoxGBT: 0.759 (95% CI: 0.736-0.783) for the female population. The addition of measurement-based variables and variables that require a prior medical examination (i.e., insulin use, number of treatments/medications taken, prevalent cardiovascular disease [other than CAD, and stroke diagnosed by a doctor]) and the further addition of biomarkers/other measurements (i.e., high-density lipoprotein [HDL] cholesterol, total cholesterol, and glycated haemoglobin) did not significantly improve QUES-CAD's performance in most instances. C-index comparisons and PLR tests showed that QUES-CAD performs and fits the data at least as well as the clinical prediction models.
Interpretation: QUES-CAD performs comparably to established clinical prediction models and enables a population-wide identification of high-risk individuals for CAD. The model developed and validated herein relies solely on ten questionnaire variables, overcoming the limitations of existing models that depend on physical measurements or biomarkers.
Funding: University Medical Center Groningen.
Keywords: Coronary artery disease; Data-driven prediction; Discriminative abilities; Machine learning; Population screening; Risk stratification.
Copyright © 2024 The Author(s). Published by Elsevier B.V. All rights reserved.
Conflict of interest statement
Declaration of interests PF, SvD, and JCF are employed by Ancora Health B.V. and own shares of Ancora Health B.V. BHRW sits on the medical advisory board of Ancora Health B.V., without being compensated for this position. All other authors have no conflict of interest to declare.
Figures


Similar articles
-
Deep-learning-based cardiovascular risk stratification using coronary artery calcium scores predicted from retinal photographs.Lancet Digit Health. 2021 May;3(5):e306-e316. doi: 10.1016/S2589-7500(21)00043-1. Lancet Digit Health. 2021. PMID: 33890578
-
Modification of coronary artery disease clinical risk factors by coronary artery disease polygenic risk score.Med. 2024 May 10;5(5):459-468.e3. doi: 10.1016/j.medj.2024.02.015. Epub 2024 Apr 19. Med. 2024. PMID: 38642556 Free PMC article.
-
Integrated Polygenic Tool Substantially Enhances Coronary Artery Disease Prediction.Circ Genom Precis Med. 2021 Apr;14(2):e003304. doi: 10.1161/CIRCGEN.120.003304. Epub 2021 Mar 2. Circ Genom Precis Med. 2021. PMID: 33651632 Free PMC article.
-
Nonobstructive Coronary Artery Disease by Coronary CT Angiography Improves Risk Stratification and Allocation of Statin Therapy.JACC Cardiovasc Imaging. 2017 Sep;10(9):1031-1038. doi: 10.1016/j.jcmg.2016.10.022. Epub 2017 Mar 15. JACC Cardiovasc Imaging. 2017. PMID: 28330658 Free PMC article. Review.
-
Prognostic models for newly-diagnosed chronic lymphocytic leukaemia in adults: a systematic review and meta-analysis.Cochrane Database Syst Rev. 2020 Jul 31;7(7):CD012022. doi: 10.1002/14651858.CD012022.pub2. Cochrane Database Syst Rev. 2020. PMID: 32735048 Free PMC article.
References
-
- Tsao C.W., Aday A.W., Almarzooq Z.I., et al. Heart disease and stroke statistics-2022 update: a report from the American Heart Association. Circulation. 2022;145(8):e153–e639. - PubMed
-
- Javed Z., Haisum Maqsood M., Yahya T., et al. Race, racism, and cardiovascular health: applying a social determinants of health framework to racial/ethnic disparities in cardiovascular disease. Circ Cardiovasc Qual Outcomes. 2022;15(1) - PubMed
-
- Kokkorakis M., Boutari C., Katsiki N., Mantzoros C.S. From non-alcoholic fatty liver disease (NAFLD) to steatotic liver disease (SLD): an ongoing journey towards refining the terminology for this prevalent metabolic condition and unmet clinical need. Metabolism. 2023;147 - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

