A Rare Neuroendocrine Tumor at the Junction of the Cystic and Common Hepatic Ducts: The Value of a Multimodal Approach in Preoperative Diagnosis
- PMID: 39726501
- PMCID: PMC11670260
- DOI: 10.7759/cureus.74486
A Rare Neuroendocrine Tumor at the Junction of the Cystic and Common Hepatic Ducts: The Value of a Multimodal Approach in Preoperative Diagnosis
Abstract
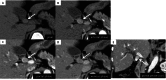
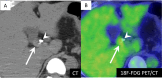
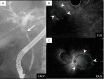
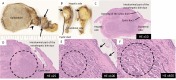
Neuroendocrine tumors (NETs) of the biliary tract are extremely rare due to a paucity of Kulchitsky cells. While their preoperative diagnosis remains challenging due to the lack of specific diagnostic markers and imaging findings, there have been no detailed reports describing the diagnostic utility of various imaging modalities for bile duct NETs at the junction of the cystic and common hepatic ducts. We report a case of a woman in her 40s who presented with jaundice and elevated hepatobiliary enzymes. Imaging studies identified a 17 mm × 15 mm × 13 mm nodule at the junction of the cystic and common hepatic ducts. Contrast-enhanced computed tomography (CT) demonstrated a well-enhanced nodule from the early phase, while magnetic resonance imaging showed slightly high intensity on T2-weighted images and strong diffusion restriction. Fluorine-18-fluorodeoxyglucose (18F-FDG) positron emission tomography/CT revealed mild 18F-FDG uptake with a maximum standardized uptake value of 3.5. Endoscopic retrograde cholangiopancreatography (ERCP) suggested extramural compression by a submucosal tumor, and endoscopic ultrasonography (EUS) and intraductal ultrasound (IDUS) revealed a well-circumscribed, homogeneous, hypoechoic submucosal nodule. This comprehensive multimodal approach allowed for the inclusion of NET in the preoperative differential diagnosis. The patient underwent cholecystectomy and extrahepatic bile duct resection, and histopathological examination confirmed a World Health Organization grade 1 NET at the junction of the cystic and common hepatic ducts. The patient remains recurrence-free after two years of follow-up. This is the first detailed report demonstrating the potential utility of a multimodal approach, including ERCP, EUS, and IDUS, in the preoperative diagnosis of biliary tract NET at this specific anatomical location, particularly in identifying the characteristic features of a submucosal tumor.
Keywords: common hepatic duct; computed tomography; cystic duct; endoscopic retrograde cholangiopancreatography; endoscopic ultrasonography; intraductal ultrasound; magnetic resonance imaging; neuroendocrine tumor.
Copyright © 2024, Saito et al.
Conflict of interest statement
Human subjects: Consent for treatment and open access publication was obtained or waived by all participants in this study. Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work. Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work. Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Figures


References
-
- Neuroendocrine and adrenal tumors, version 2.2021, NCCN clinical practice guidelines in oncology. Shah MH, Goldner WS, Benson AB, et al. J Natl Compr Canc Netw. 2021;19:839–868. - PubMed
-
- Klimstra DS, Lam AK, Paradis V, et al. Digestive System Tumours, WHO Classification of Tumours, 5th Edition, Volume 1. Vol. 1. Lyon, France: World Health Organaization; 2019. Tumours of the Gallbladder and Extrahepatic Bile Ducts; pp. 292–294.
-
- Carcinoid tumor of the common bile duct: evidence for its origin in metaplastic endocrine cells. Barrón-Rodríguez LP, Manivel JC, Méndez-Sánchez N, et al. Am J Gastroenterol. 1991;86:1073–1076. - PubMed
-
- Well-differentiated neuroendocrine (carcinoid) tumors of the extrahepatic biliary ducts. Noronha YS, Raza AS. Arch Pathol Lab Med. 2010;134:1075–1079. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
