Causal Associations Between Sleep Traits and Delirium: A Bidirectional Two-Sample Mendelian Randomization Study
- PMID: 39726858
- PMCID: PMC11669593
- DOI: 10.2147/NSS.S491216
Causal Associations Between Sleep Traits and Delirium: A Bidirectional Two-Sample Mendelian Randomization Study
Abstract
Purpose: Numerous studies have identified a correlation between sleep and delirium; however, the causal relationship remains ambiguous. This bidirectional two-sample Mendelian randomization (MR) study was conducted to examine the possible causal relationships between sleep traits and delirium.
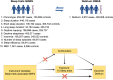
Patients and methods: Utilizing genome-wide association studies (GWAS), we identified ten sleep traits: chronotype, sleep duration, short sleep duration, long sleep duration, daytime napping, daytime sleepiness, insomnia, number of sleep episodes (NSE), sleep efficiency, and rapid eye movement sleep behavior disorder (RBD). In this MR study, genetic variants independently associated with exposures were selected as instrumental variables (IVs). To establish causal inferences, three regression models were employed-inverse variance weighted (IVW), MR Egger, and weighted median (WM) -and conducted sensitivity analyses to assess the robustness of our findings.
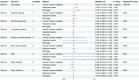
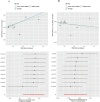
Results: Our results suggest no significant causal association between the ten sleep traits and the risk of delirium. The reverse MR analysis revealed that delirium is associated with an increased propensity for morning chronotype [ORIVW, 1.025; 95% CI, 1.012-1.036; p = 1.50E-05; adjusted p values (padjusted)= 1.35E-04] and a decreased risk of long sleep duration [ORIVW, 0.996; 95% CI, 0.993-0.999; p = 0.013; padjusted= 0.059]. However, no robust evidence currently exists to substantiate a causal relationship between delirium and other sleep traits.
Conclusion: Our bidirectional, two-sample MR analysis study did not provide definitive evidence that sleep traits may augment the susceptibility to delirium. However, the reverse MR results indicate that delirium may predispose patients to an earlier sleep-wake cycle. Additional large-scale investigations are necessary to examine the bidirectional causality between delirium and sleep traits.
Keywords: Mendelian randomization analysis; delirium; genome-wide association studies; sleep traits.
© 2024 Liu et al.
Conflict of interest statement
The authors claim that the research had no commercial or financial conflicts of interest.
Figures

Similar articles
-
Causal Relationship Between Sleep Traits and Risk of Systemic Lupus Erythematosus: A Two-Sample Mendelian Randomization Study.Front Immunol. 2022 Jun 17;13:918749. doi: 10.3389/fimmu.2022.918749. eCollection 2022. Front Immunol. 2022. PMID: 35784289 Free PMC article.
-
Mendelian randomization of individual sleep traits associated with major depressive disorder.J Affect Disord. 2024 Nov 15;365:105-111. doi: 10.1016/j.jad.2024.08.068. Epub 2024 Aug 15. J Affect Disord. 2024. PMID: 39153551 Review.
-
Association between sleep traits and risk of colorectal cancer: a bidirectional Mendelian randomization study.J Gastrointest Oncol. 2024 Aug 31;15(4):1556-1567. doi: 10.21037/jgo-24-11. Epub 2024 Jul 22. J Gastrointest Oncol. 2024. PMID: 39279980 Free PMC article.
-
Causal relationship between sleep characteristics and thyroid function: A bidirectional Mendelian randomization study.Medicine (Baltimore). 2024 Nov 15;103(46):e40516. doi: 10.1097/MD.0000000000040516. Medicine (Baltimore). 2024. PMID: 39560538 Free PMC article.
-
Associations between sleep traits and colorectal cancer: a mendelian randomization analysis.Front Oncol. 2025 Feb 6;15:1416243. doi: 10.3389/fonc.2025.1416243. eCollection 2025. Front Oncol. 2025. PMID: 39980544 Free PMC article.
Cited by
-
Causal relationship between distinct sleep characteristics and delirium: A multivariable Mendelian randomization study.Medicine (Baltimore). 2025 May 30;104(22):e42600. doi: 10.1097/MD.0000000000042600. Medicine (Baltimore). 2025. PMID: 40441237 Free PMC article.
-
The intersection of delirium and long-term cognition in older adults: the critical role of delirium prevention.J Neurol. 2025 May 6;272(6):381. doi: 10.1007/s00415-025-13104-1. J Neurol. 2025. PMID: 40329080 Review.
References
LinkOut - more resources
Full Text Sources

