Interobserver Variability in Manual Versus Semi-Automatic CT Assessments of Small Lung Nodule Diameter and Volume
- PMID: 39728910
- PMCID: PMC11680079
- DOI: 10.3390/tomography10120148
Interobserver Variability in Manual Versus Semi-Automatic CT Assessments of Small Lung Nodule Diameter and Volume
Abstract
Background: This study aimed to assess the interobserver variability of semi-automatic diameter and volumetric measurements versus manual diameter measurements for small lung nodules identified on computed tomography scans.
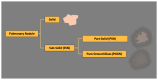
Methods: The radiological patient database was searched for CT thorax examinations with at least one noncalcified solid nodule (∼3-10 mm). Three radiologists with four to six years of experience evaluated each nodule in accordance with the Fleischner Society guidelines using standard diameter measurements, semi-automatic lesion diameter measurements, and volumetric assessments. Spearman's correlation coefficient measured intermeasurement agreement. We used descriptive Bland-Altman plots to visualize agreement in the measured data. Potential discrepancies were analyzed.
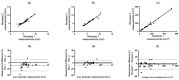
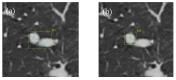
Results: We studied a total of twenty-six nodules. Spearman's test showed that there was a much stronger relationship (p < 0.05) between reviewers for the semi-automatic diameter and volume measurements (avg. r = 0.97 ± 0.017 and 0.99 ± 0.005, respectively) than for the manual method (avg. r = 0.91 ± 0.017). In the Bland-Altman test, the semi-automatic diameter measure outperformed the manual method for all comparisons, while the volumetric method had better results in two out of three comparisons. The incidence of reviewers modifying the software's automatic outline varied between 62% and 92%.
Conclusions: Semi-automatic techniques significantly reduced interobserver variability for small solid nodules, which has important implications for diagnostic assessments and screening. Both the semi-automatic diameter and semi-automatic volume measurements showed improvements over the manual measurement approach. Training could further diminish observer variability, given the considerable diversity in the number of adjustments among reviewers.
Keywords: computed tomography (CT); interobserver variability; lung nodule size; semi-automatic measurement.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures





Similar articles
-
Influence of lung nodule margin on volume- and diameter-based reader variability in CT lung cancer screening.Br J Radiol. 2018 Oct;91(1090):20170405. doi: 10.1259/bjr.20170405. Epub 2017 Nov 8. Br J Radiol. 2018. PMID: 28972803 Free PMC article.
-
Improved Interobserver Agreement on Lung-RADS Classification of Solid Nodules Using Semiautomated CT Volumetry.Radiology. 2020 Dec;297(3):675-684. doi: 10.1148/radiol.2020200302. Epub 2020 Sep 15. Radiology. 2020. PMID: 32930652 Free PMC article.
-
Comparison of the effects of model-based iterative reconstruction and filtered back projection algorithms on software measurements in pulmonary subsolid nodules.Eur Radiol. 2017 Aug;27(8):3266-3274. doi: 10.1007/s00330-016-4716-5. Epub 2017 Jan 5. Eur Radiol. 2017. PMID: 28058482
-
Improved interobserver agreement on nodule type and Lung-RADS classification of subsolid nodules using computer-aided solid component measurement.Eur J Radiol. 2022 Jul;152:110339. doi: 10.1016/j.ejrad.2022.110339. Epub 2022 May 5. Eur J Radiol. 2022. PMID: 35537358
-
Noncalcified lung nodules: volumetric assessment with thoracic CT.Radiology. 2009 Apr;251(1):26-37. doi: 10.1148/radiol.2511071897. Radiology. 2009. PMID: 19332844 Free PMC article. Review.
References
-
- Callister M.E., Baldwin D.R., Akram A.R., Barnard S., Cane P., Draffan J., Franks K., Gleeson F., Graham R., Malhotra P., et al. British Thoracic Society guidelines for the investigation and management of pulmonary nodules. Thorax. 2015;70((Suppl. S2)):ii1–ii54. doi: 10.1136/thoraxjnl-2015-207168. - DOI - PubMed
-
- MacMahon H., Naidich D.P., Goo J.M., Lee K.S., Leung A.N., Mayo J.R., Mehta A.C., Ohno Y., Powell C.A., Prokop M., et al. Guidelines for Management of Incidental Pulmonary Nodules Detected on CT Images: From the Fleischner Society 2017. Radiology. 2017;284:228–243. doi: 10.1148/radiol.2017161659. - DOI - PubMed
-
- Gould M.K., Donington J., Lynch W.R., Mazzone P.J., Midthun D.E., Naidich D.P., Wiener R.S. Evaluation of Individuals with Pulmonary Nodules: When Is It Lung Cancer? Diagnosis and Management of Lung Cancer, 3rd ed; American College of Chest Physicians evidence-based clinical practice guidelines. Chest. 2013;143((Suppl. S5)):e93S–e120S. doi: 10.1378/chest.12-2351. - DOI - PMC - PubMed
-
- Naidich D.P., Bankier A.A., MacMahon H., Schaefer-Prokop C.M., Pistolesi M., Goo J.M., Macchiarini P., Crapo J.D., Herold C.J., Austin J.H., et al. Recommendations for the management of subsolid pulmonary nodules detected at CT: A statement from the Fleischner Society. Radiology. 2013;266:304–317. doi: 10.1148/radiol.12120628. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

