Endograft-specific hemodynamics after endovascular aneurysm repair: a CFD analysis
- PMID: 39733131
- PMCID: PMC11682169
- DOI: 10.1038/s41598-024-83148-2
Endograft-specific hemodynamics after endovascular aneurysm repair: a CFD analysis
Abstract
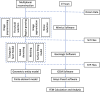
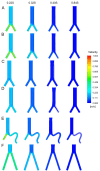
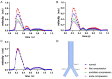
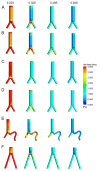
Intraluminal prosthetic graft thrombus (IPT) has been described in case of endovascular aortic pathology repair. This study aimed to assess hemodynamic indicators associated with various anatomical morphologies following endovascular aortic repair (EVAR), aiming to offer further references for the choice of clinical therapy. Six model models (normal, iliac compression, aortic compression, aortoiliac compression, iliac distortion, and long-leg stent) were established based on common anatomical morphologies following EVAR. Hemodynamic indicators, such as flow velocity, time-average wall shear stress (TAWSS), oscillatory shear stress index (OSI), and relative residence time (RRT), were captured using computational fluid dynamics (CFD), and the differences between the six models were examined. The peak blood flow velocity at the compressed side iliac artery and the uncompressed side iliac artery corresponding to the aortoiliac artery compression model and the aortic compression model decreased by 30.63% to 48.62%, compared with that in the normal model. Compared with that in the normal model, the peak blood flow velocity at the aorta and the distorted side iliac artery in the iliac distortion model decreased by 7.89% and 41.13%, respectively. The length of the iliac artery stent has little effect on the blood flow velocity. The TAWSS at Iliac grafts showed varying degrees of decline in the other three compression models, particularly in the aortic compression model compared to the normal model. The TAWSS increases at the corner of the artery showing distortion but exhibited a significant decrease toward the distal end of the corner. The areas with higher OSI, and longer RRT were concentrated in the aortoiliac compression model and the iliac distortion model. We found that endograft compression and distortion may be risk factors for IPT. Moreover, the influence of longer stents on the hemodynamics inside stent-grafts is negligible. However, future real-world studies should be conducted to test and verify this speculation.
Keywords: Abdominal aortic aneurysm; Computational fluid dynamics; Endovascular aneurysm repair; Hemodynamic indicator; Intraluminal prosthetic graft thrombus.
© 2024. The Author(s).
Conflict of interest statement
Declarations. Competing interests: The authors declare no competing interests.
Figures






References
-
- Jackson, R. S., Chang, D. C. & Freischlag, J. A. Comparison of long-term survival after open vs endovascular repair of intact abdominal aortic aneurysm among Medicare beneficiaries. JAMA307(15), 1621–1628 (2012). - PubMed
-
- Bianchini Massoni, C. et al. Prevalence, risk factors and clinical impact of intraprosthetic thrombus deposits after EVAR. J. Cardiovasc. Surg. (Torino)61(6), 729–737 (2020). - PubMed
-
- Maleux, G. et al. Mural thrombotic deposits in abdominal aortic endografts are common and do not require additional treatment at short-term and midterm follow-up. J. Vasc. Interv. Radiol.19(11), 1558–1562 (2008). - PubMed
Publication types
MeSH terms
Grants and funding
- JYLJ202204/Clinical Research Program of 9th People's Hospital
- 21S31904300/Shanghai Science and Technology Innovation Action Plan
- 20224Y0170/Shanghai Municipal Health Bureau Project
- No.JYYC004/Original Exploration Project of Shanghai Ninth People's Hospital
- 82300540/National Natural Science Foundation of China
LinkOut - more resources
Full Text Sources
Miscellaneous

