On-Call Simulation: A One-Day Comprehensive Simulation of Clinical Practice for Final-Year Medical Students
- PMID: 39735066
- PMCID: PMC11672163
- DOI: 10.7759/cureus.74555
On-Call Simulation: A One-Day Comprehensive Simulation of Clinical Practice for Final-Year Medical Students
Abstract
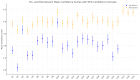
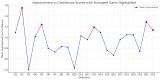
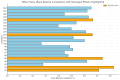
Introduction Transitioning from a medical student to a foundation doctor presents numerous challenges, particularly in managing on-call duties that require quick decision-making, clinical skills, and prioritisation under pressure. The Simulation On-Call (SOC) program was developed as a one-day, immersive simulation event to equip final-year medical students with the skills and confidence needed for these responsibilities. Methods The SOC program is an annual event held for final-year medical students at the Royal Blackburn Hospital, Blackburn, UK. It is conducted over five days, with 80 final-year medical students rotating through nine stations that replicated common on-call scenarios. Each station required students to address critical medical situations, such as managing an acutely unwell patient, electrolyte abnormalities, and referring and communicating with colleagues, while managing realistic interruptions through a "bleep" system. Pre- and post-event questionnaires, featuring 25 Likert-scale items, were disseminated to assess student feedback and self-reported confidence across competencies, including communication, clinical decision-making, and task prioritisation. A retrospective review and analysis of the feedback was performed to assess the impact of the SOC program by assessing the pre- and post-session questionnaires. Results Of the 80 participants, 70 completed the pre-event questionnaire, and 72 completed the post-event questionnaire. Statistical analysis revealed a significant increase in students' self-reported confidence across all 25 Likert-scale items, with marked improvements in task prioritisation (rₛ = 0.74, p < 0.001), managing acutely unwell patients (rₛ = 0.60, p < 0.001), and escalation skills (rₛ = 0.49, p < 0.001). Effect sizes ranged from moderate to large, underscoring the practical impact of the Simulation On-Call program in enhancing preparedness and confidence for on-call responsibilities. Conclusion The SOC program provided a valuable, realistic, and supportive environment for final-year medical students to practice on-call responsibilities. The significant improvement in student confidence highlights the effectiveness of this program as a preparatory tool for foundation doctors. Future iterations will incorporate feedback to continually refine the simulation experience, ensuring its alignment with clinical demands.
Keywords: emergency simulation; medical edu; medical student teaching; simulation based training; simulation course; simulation design; simulation in medical education; skills and simulation training; student education; teaching by simulation.
Copyright © 2024, Desouky et al.
Conflict of interest statement
Human subjects: Consent for treatment and open access publication was obtained or waived by all participants in this study. Animal subjects: All authors have confirmed that this study did not involve animal subjects or tissue. Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work. Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work. Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Figures
References
-
- Training and simulation for patient safety. Aggarwal R, Mytton OT, Derbrew M, et al. Qual Saf Health Care. 2010;19 Suppl 2:0–43. - PubMed
-
- Features and uses of high-fidelity medical simulations that lead to effective learning: a BEME systematic review. Issenberg SB, McGaghie WC, Petrusa ER, Lee Gordon D, Scalese RJ. Med Teach. 2005;27:10–28. - PubMed
-
- The utility of simulation in medical education: what is the evidence? Okuda Y, Bryson EO, DeMaria S Jr, Jacobson L, Quinones J, Shen B, Levine AI. Mt Sinai J Med. 2009;76:330–343. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous
