Burden of comorbidities in heart failure patients in Türkiye
- PMID: 39735480
- PMCID: PMC11673618
- DOI: 10.55730/1300-0144.5934
Burden of comorbidities in heart failure patients in Türkiye
Abstract
Background/aim: Heart failure (HF) is associated with a wide range of comorbidities that negatively impact clinical outcomes and cause high economic burden. We aimed to evaluate the frequency and burden of comorbidities in HF patients in Türkiye and their relationships with patients' demographic characteristics.
Materials and methods: Based on ICD-10 codes in the national electronic database of the Turkish Ministry of Health covering the entire population of Türkiye (n = 85,279,553) from 1 January 2016 to 31 December 2022, data on the prevalence of comorbidities in HF patients were obtained. The frequency and burden of comorbidities were analyzed separately by age groups, sex, and socioeconomic status (SES).
Results: Between 2016 and 2022, there were 2,722,151 patients (51.7% female) of all ages who were diagnosed with HF. In Türkiye, the most common comorbidities of HF patients were hypertension (HT) (97.6%), atherosclerotic cardiovascular disease (ASCVD) (84.9%), dyslipidemia (59.5%), anxiety disorder (48.1%), diabetes mellitus (DM) (45.2%), chronic obstructive pulmonary disease (COPD) (43.6%), anemia (40.6%), and atrial fibrillation (AF) (37.1%). Female patients had higher rates of anemia, DM, HT, and anxiety disorders, while male patients had higher rates of ASCVD, COPD, and dyslipidemia. The most common comorbidity in patients under 20 years of age was congenital heart disease (52.3%). More than 90% of HF patients had ≥2 comorbidities. HF patients with ≥5 comorbidities increased from 18.1% in the group aged 20-49 years to 38.3% in the group aged 50-79 years. Comorbidities were similar across SES groups.
Conclusion: The most common comorbidities in cases of HF in Türkiye are HT, ASCVD, dyslipidemia, DM, COPD, anemia, and AF, respectively, and more than 90% of patients have ≥2 comorbidities. While ASCVD and dyslipidemia were more common in male patients, anemia, DM, and anxiety disorders were more common in female patients. The number of comorbid conditions increased with advanced age.
Keywords: Comorbidity; comorbidity burden; electronic health records; heart failure.
© TÜBİTAK.
Conflict of interest statement
Conflict of interest: The authors declare that there is no conflict of interest regarding the publication of this manuscript.
Figures
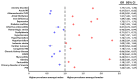

References
-
- McDonagh TA, Metra M, Adamo M, Gardner RS, Baumbach A, et al. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: developed by the Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC) With the special contribution of the Heart Failure Association (HFA) of the ESC. European Heart Journal. 2021;42(36):3599–3726. doi: 10.1093/eurheartj/ehab368. - DOI - PubMed
-
- Heidenreich PA, Bozkurt B, Aguilar D, Allen LA, Byun JJ, et al. 2022 AHA/ACC/HFSA guideline for the management of heart failure: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Journal of the American College of Cardiology. 2022;79(17):e263–e421. doi: 10.1016/j.jacc.2021.12.012. - DOI - PubMed
-
- Goff DC, Jr, Lloyd-Jones DM, Bennett G, Coady S, D’Agostino RB, et al. American College of Cardiology/American Heart Association Task Force on Practice Guidelines. 2013 ACC/AHA guideline on the assessment of cardiovascular risk: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation 2014; 24: S49–73. Erratum in: Circulation. 2014;24:S74–75. doi: 10.1161/01.cir.0000437741.48606.98. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

