Histological evaluation of the regenerative potential of injectable hyaluronic acid hydrogel or collagen with blood clot as scaffolds during revascularization of immature necrotic dog's teeth
- PMID: 39737041
- PMCID: PMC11682749
- DOI: 10.5455/OVJ.2024.v14.i11.29
Histological evaluation of the regenerative potential of injectable hyaluronic acid hydrogel or collagen with blood clot as scaffolds during revascularization of immature necrotic dog's teeth
Abstract
Background: Regenerative endodontics' primary objective is to establish a favorable environment in the root canal by removing infection, providing a sturdy scaffold, and sealing the apical end of the tooth tightly. These actions should promote pulp regeneration and root development.
Aim: This study evaluated histologically the regenerative potential of injectable hyaluronic acid (HA) hydrogel or collagen with blood clot as scaffolds during revascularization of immature necrotic dog's teeth.
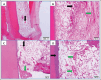
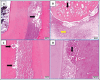
Methods: Sixteen permanent immature necrotic premolars with 32 roots were chosen from two 4-5-month-old mongrel dogs. Out of the 32 roots, 24 roots were sealed for 2 weeks after being cleaned with CaOH2. According to the treatment protocol, the 24 cleaned roots were randomly assigned to one of three treatment groups (each with 8 roots): blood clot + HA group, blood clot + collagen group, and blood clot group. The control group consisted of the eight infected roots that remained untreated. Three months after the surgery, the assessment of tissue ingrowth in the pulp cavity took into account the kind of cellular components, the intercellular matrix, angiogenesis, and the occurrence of any hard tissue formation. The pulp's capacity for regeneration was described descriptively, taking into account the type of regenerated tissue, the root's apical closure, and any potential periodontal and periapical histological alterations. Semi-quantitative analysis was used to assess the degree of pulp tissue regeneration. Tukey's post hoc test was used after a two-way ANOVA for statistical analysis of all the data.
Results: When comparing the treated groups to the control group, a significant increase in tissue ingrowth and a significant decrease in the periapical inflammatory reaction were noted (p < 0.05). It's interesting to note that blood clot + HA group's inflammatory cell count was significantly greater (p < 0.05) than that of the other treatment groups. Furthermore, blood clot + collagen group and blood clot group did not differ significantly in inflammatory cell count from one another. Tissue ingrowth did not differ significantly (p > 0.05) amongst treated groups.
Conclusion: The tissue regeneration of the immature necrotic teeth is improved by revascularization, whether or not it is combined with HA or collagen scaffolds. After revascularization, using HA as a scaffold is less efficient in reducing the inflammation than collagen.
Keywords: Dental pulps; Periapical pathosis; Regenerative endodontic; Revascularization; Scaffolds.
Conflict of interest statement
The authors declare no conflicts of interest to report.
Figures


References
-
- Abada, H.M., Hashem, A.A.R., Abu-Seida, A.M. and Nagy, M.M. 2022. The effect of changing apical foramen diameter on regenerative potential of mature teeth with necrotic pulp and apical periodontitis. Clin. Oral Investig. 26(2), 1843–1853. - PubMed
-
- Abbas, K.F., Tawfik, H., Hashem, A.A., Ahmed, H.M.A., Abu-Seida, A.M. and Refai, H.M. 2020. Histopathological evaluation of different regenerative protocols using Chitosan-based formulations for management of immature non-vital teeth with apical periodontitis: in vivo study. Aust. Endod. J. 46, 405–414. - PubMed
-
- Abdelsalam, N., Abu Seida, A.M., Fayyad, D. and Tawfik, H. 2020. Radiographic and histopathologic outcomes of immature dog teeth with apical periodontitis after revascularization using propolis. Saudi Endod. J. 10(3), 199–207.
-
- Abdelsalam, M.S., Elgendy, A.A., Abu-Seida, A.M., Abdelaziz, T.M. and El-Haddad, K.E. 2024. Radiography evaluation of the regenerative potential of injectable hyaluronic acid hydrogel or collagen with blood clot as scaffolds during revascularization of immature necrotic dog’s teeth. Ain Shams Dent. J. 2024 [In Press].
-
- Abu-Seida, A.M.A. 2012. Efficacy of diclofenac sodium, either alone or together with cefotaxime sodium, for control of postoperative pain, in dogs undergoing ovariohysterectomy. Asian J. Anim. Vet. Adv. 7, 180–186.
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
