Femoral nerve palsy following Girdlestone resection arthroplasty: An observational cadaveric study
- PMID: 39744734
- PMCID: PMC11686531
- DOI: 10.5312/wjo.v15.i12.1175
Femoral nerve palsy following Girdlestone resection arthroplasty: An observational cadaveric study
Abstract
Background: When patients with a failed hip arthroplasty are unsuitable for reimplantation, Girdlestone resection arthroplasty (GRA) is a viable treatment option. We report on a patient who was treated with a GRA due to a periprosthetic infection. We discovered partial paralysis of the quadriceps muscle in this patient. We investigated the femoral nerve anatomy, particularly the nerve entry points, to better understand this phenomenon.
Aim: To reveal the femoral nerve anatomy with respect to severe proximal migration after GRA.
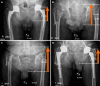
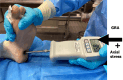
Methods: Eight cadaveric hemipelves were investigated. The branches of the femoral nerve were dissected and traced distally. The GRA was performed by the direct anterior approach. Axial stress to the lower extremity was applied, and the relative movement of the femur was recorded. The femoral nerve and its entry points were assessed.
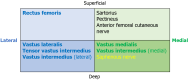
Results: GRA led to a 3.8 cm shift of the femur in vertical direction, a 1.8 cm shift in the dorsal direction, and a 2.3 cm shift in the lateral direction. A 36.5° external shift was observed. This caused stress to the lateral division of the femoral nerve. We observed migration of the femoral nerve entry point at the following locations: (1) Vastus medialis (5.3 mm); (2) The medial part of the vastus intermedius (5.4 mm); (3) The lateral part of the vastus intermedius (16.3 mm); (4) Rectus femoris (23.1 mm); (5) Tensor vastus intermedius (30.8 mm); and (6) Vastus lateralis (28.8 mm).
Conclusion: Migration of the femur after GRA altered the anatomy of the femoral nerve. Stress occurred at the lateral nerve division leading to poor functional results.
Keywords: Anatomy of the femoral nerve; Failed hip replacement; Femoral nerve palsy; Girdlestone resection arthroplasty; Periprosthetic infection; Resection arthroplasty of the hip.
©The Author(s) 2024. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: Dominik Spuehler, Lukas Kuster, and Karl Grob have no conflicts of interest to disclose. Professor Oliver Ullrich is Vice President of the German Society for Aerospace Medicine (DGLRM), President of the Swiss SkyLab Foundation (Zurich, Switzerland), and he is a member of the following Editorial Boards: Scientific Reports (Nature), Acta Astronautica (Elsevier), International Journal of Molecular Science (MDPI), Flugmedizin, Reisemedizin, Tropenmedizin (Thieme).
Figures

References
-
- Malcolm TL, Gad BV, Elsharkawy KA, Higuera CA. Complication, Survival, and Reoperation Rates Following Girdlestone Resection Arthroplasty. J Arthroplasty. 2015;30:1183–1186. - PubMed
-
- Basu I, Howes M, Jowett C, Levack B. Girdlestones excision arthroplasty: current update. Int J Surg. 2011;9:310–313. - PubMed
LinkOut - more resources
Full Text Sources

