Living alone predicts non-home discharge post elective hip arthroplasty: A matched-pair cohort study
- PMID: 39746111
- PMCID: PMC11694960
- DOI: 10.1371/journal.pone.0316024
Living alone predicts non-home discharge post elective hip arthroplasty: A matched-pair cohort study
Abstract
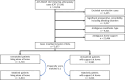
The impact of home support and interaction with family members on recovery and perioperative outcomes remains unclear. We determined whether living alone was predictive of discharge disposition following total hip arthroplasty (THA). Data were from American College of Surgeons National Surgical Quality Improvement Program participating hospitals in 2021. The primary endpoint was discharging disposition. A total of 1716 patients living alone and 3961 with others at home were identified. The 1:1 propensity-matched cohort included 3248 total patients (1624 in each group). On univariate analysis, living alone was associated with non-home discharge (22.0% [358/1624] vs. 10.5% [170/1623]; odds ratio [OR], 2.42 [95% CI, 1.98 to 2.94]; P < .001), need for services in those returning home (63.1% [799/1266] vs. 57.7% [839/1453]; OR, 1.25 [95% CI, 1.07 to 1.46]; P = .004), and increased length of hospital stay (2.05 vs. 1.72 days; mean difference, 0.34 [95% CI, 0.18 to 0.49]; P < .001). On multivariable analysis, living alone remained an independent predictor of non-home discharge (adjusted odds ratio, 2.84 [95% CI, 2.30 to 3.54]; c = 0.734). Thus, compared to propensity-matched THA patients with others at home, those living alone experience a much greater rate of non-home discharge and need for support.
Copyright: © 2025 Agnor et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Figures

References
-
- Fingar KR, Stocks C, Weiss AJ, Steiner CA. Most Frequent Operating Room Procedures Performed in U.S. Hospitals, 2003–2012. Healthcare Cost and Utilization Project (HCUP) Statistical Briefs. Rockville (MD): Agency for Healthcare Research and Quality (US); 2006. Available: http://www.ncbi.nlm.nih.gov/books/NBK274246/ - PubMed
-
- Kitsis P, Zisimou T, Gkiatas I, Kostas-Agnantis I, Gelalis I, Korompilias A, et al. Postoperative Delirium and Postoperative Cognitive Dysfunction in Patients with Elective Hip or Knee Arthroplasty: A Narrative Review of the Literature. Life (Basel). 2022;12: 314. doi: 10.3390/life12020314 - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

