Association Between Nocturnal Hypoxemia Parameters and Coronary Microvascular Dysfunction: A Cross-Sectional Study
- PMID: 39749250
- PMCID: PMC11694025
- DOI: 10.2147/NSS.S494018
Association Between Nocturnal Hypoxemia Parameters and Coronary Microvascular Dysfunction: A Cross-Sectional Study
Abstract
Objective: There is a connection between obstructive sleep apnea (OSA) and coronary microvascular dysfunction (CMD), but the underlying mechanisms remain unclear. This study aims to evaluate the correlation between OSA-related nocturnal hypoxemia parameters and CMD.
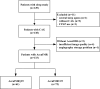
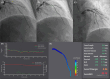
Methods: This is an observational, single-center study that included patients who underwent polysomnography and coronary angiography during hospitalization. The presence of CMD was determined by angio-based index of microcirculatory resistance (AccuIMR). Categorical variables were compared using chi-square test or Fisher exact test. The t-test and Mann-Whitney U-test were used to compare normally and non-normally distributed continuous variables, respectively. Univariate and multivariable logistic regression analyses were performed to evaluate the relationship between nocturnal hypoxemia parameters and CMD.
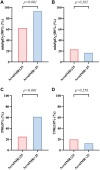
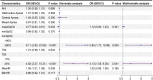
Results: A total of 133 patients were included in this study, of whom 72 (54.14%) had evidence of CMD. Patients with CMD exhibited a higher prevalence of OSA and experienced more severe nocturnal hypoxia. After adjusting for potential confounding factors, minimum oxygen saturation (minSpO2) ≤90% (OR 5.89; 95% CI 1.73-19.99; P=0.004) and the percentage of time spent with oxygen saturation below 90% (T90) ≥5% (OR 3.13; 95% CI 1.05-9.38; P=0.041) were independently associated with CMD. However, no significant association was observed between apnea-hypopnea index (AHI) and CMD.
Conclusion: Parameters of nocturnal hypoxemia are associated with CMD. Hypoxemia parameters may more sensitively reflect the correlation between OSA and CMD than AHI.
Keywords: cardiology; coronary microvascular dysfunction; dentistry; nocturnal hypoxemia; obstructive sleep apnea.
© 2024 Feng et al.
Conflict of interest statement
The authors report no conflicts of interest in this work.
Figures
References
-
- Pepine CJ, Anderson RD, Sharaf BL, et al. Coronary microvascular reactivity to adenosine predicts adverse outcome in women evaluated for suspected ischemia results from the National Heart, Lung and Blood Institute WISE (Women’s Ischemia Syndrome Evaluation) study. J Am Coll Cardiol. 2010;55(25):2825–2832. doi: 10.1016/j.jacc.2010.01.054 - DOI - PMC - PubMed
-
- Ng MK, Yeung AC, Fearon WF. Invasive assessment of the coronary microcirculation: superior reproducibility and less hemodynamic dependence of index of microcirculatory resistance compared with coronary flow reserve. Circulation. 2006;113(17):2054–2061. doi: 10.1161/CIRCULATIONAHA.105.603522 - DOI - PubMed
LinkOut - more resources
Full Text Sources

