Evaluation of Dynamic Respiratory Muscle Strength, Physical Fitness, and Physical Activity in Children with Asthma and Healthy Peers
- PMID: 39766006
- PMCID: PMC11675843
- DOI: 10.3390/healthcare12242579
Evaluation of Dynamic Respiratory Muscle Strength, Physical Fitness, and Physical Activity in Children with Asthma and Healthy Peers
Abstract
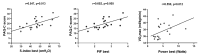
Background: Systemic inflammation, attacks, deterioration of thoracic region mechanics, medications used, and decreased physical activity level (PAL) and fitness negatively may affect respiratory muscle strength. The primary aim of this study was to evaluate dynamic inspiratory muscle strength (S-index), PAL, and physical fitness in children with asthma compared to healthy peers. The secondary aim of this study was to investigate the relationships between S-index and peak inspiratory flow (PIF) values and functional parameters in childhood asthma. Methods: This cross-sectional prospective study consisted of participants of 6-11 years of age, specifically, 20 children with asthma and 20 healthy peers. The device (POWERbreathe K5) evaluated PIF and S-index variables. PAL was determined with the Physical Activity Questionnaire-Child (PAQ-C) and fitness was evaluated with the FITNESSGRAM test battery. Results: The PIF Average (Avg): 1.8 ± 0.6, Best: 2.6 ± 0.6 (asthmatic children) vs. Avg: 2.4 ± 0.7, Best: 3.1 ± 0.9 (healthy children); p = 0.017, p = 0.027, respectively) and S-index (Avg: 34.1 ± 10.3, Best: 45.6 ± 9.9 (asthmatic children) vs. Avg: 43.2 ± 12.1, Best: 56.6 ± 14.7 (healthy children); p = 0.015, p = 0.008 respectively) values of children with asthma were significantly lower compared to healthy peers. The PAL and physical fitness of asthmatic and healthy peers were similar (p > 0.05). There were significant relationships between S-indexavg and S-indexbest with the PAQ-C score (r = 0.498, p < 0.025 r = 0.547, p < 0.013, respectively) and PIFavg and PIFbest with the PAQ-C score (r = 0.490, p < 0.028 r = 0.602, p < 0.005) in children with asthma. Conclusions: Dynamic respiratory muscle strength is negatively affected in children with asthma whereas their physical activity and fitness levels are comparable to their peers. However, it was found that children with a higher S-index and PIF rate had higher PALs. These findings suggest that pulmonary rehabilitation interventions to improve respiratory muscle function should be considered an important strategy to maintain and increase physical activity levels in children with asthma.
Keywords: S-index; asthma; child; fitness; physical activity.
Conflict of interest statement
The authors declare no potential conflicts of interest.
Figures
References
-
- Levy M.L., Bacharier L.B., Bateman E., Boulet L.P., Brightling C., Buhl R., Brusselle G., Cruz A.A., Drazen J.M., Duijts L., et al. Key recommendations for primary care from the 2022 Global Initiative for Asthma (GINA) update. NPJ Prim. Care Respir. Med. 2023;33:7. doi: 10.1038/s41533-023-00330-1. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Research Materials