Correlation Between BMI and Kidney Tumor Lateralization: Insights into Survival and Risk Factors
- PMID: 39766039
- PMCID: PMC11674721
- DOI: 10.3390/cancers16244139
Correlation Between BMI and Kidney Tumor Lateralization: Insights into Survival and Risk Factors
Abstract
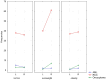
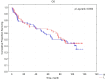
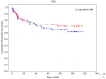
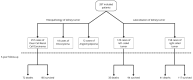
Background: Kidney cancer accounts for approximately 2% of all diagnosed cancers and fatalities worldwide, and a notable increase in its incidence has been observed in recent years. Previous studies have identified various risk factors for renal cell carcinoma (RCC), including age, gender, smoking, hypertension, overweight, and obesity. However, limited information is available regarding the correlation between RCC risk factors and tumor lateralization. Objectives: To investigate the relationship between body mass index (BMI) and the lateralization of kidney tumors in patients undergoing surgery for renal cell carcinoma. Moreover, we aim to evaluate the impact of lateralization of malignant kidney tumors on overall survival (OS) and cancer-specific survival (CSS). Materials and Methods: This single-center study included 287 patients who underwent surgical treatment for kidney tumors between January 2016 and December 2019. The patients were allocated into the following groups based on their BMI: normal (18.5-24.99 kg/m2), overweight (25-29.99 kg/m2), or obese (≥30 kg/m2). The study collected demographic and histopathological data, as well as patient history, including risk factors such as smoking and hypertension. Results: Right-sided kidney tumors occurred more frequently (55.05%, n = 158) than left-sided ones (44.95%, n = 129). A statistically significant relationship (p = 0.04731) was observed between BMI and the frequency of right-sided kidney tumors in the overweight group (70 vs. 43 cases). There was no correlation between BMI and the occurrence of kidney tumors in the normal BMI and obesity groups. Furthermore, the analysis revealed no association between the lateralization of kidney tumors, smoking, and hypertension. The 5-year survival rate was 62%, with a mean follow-up duration of 104 months (approximately 8.5 years). No statistically significant difference was observed between the right- and left-sided cancer groups, with survival rates of 58% and 66%, respectively (p = 0.652). Conclusions: This study highlighted that right-sided kidney tumors occurred significantly more frequently in overweight individuals in our cohort of patients. No association was observed between lateralization of kidney cancer and overall survival (OS) or cancer-specific survival (CSS).
Keywords: hypertension; kidney cancer; lateralization; obesity; overweight.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

References
-
- Huang J., Leung D.K.-W., Chan E.O.-T., Lok V., Leung S., Wong I., Lao X.-Q., Zheng Z.-J., Chiu P.K.-F., Ng C.-F., et al. A Global Trend Analysis of Kidney Cancer Incidence and Mortality and Their Associations with Smoking, Alcohol Consumption, and Metabolic Syndrome. Eur. Urol. Focus. 2022;8:200–209. doi: 10.1016/j.euf.2020.12.020. - DOI - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources

