A 15-Year Observational Cohort of Acute Empyema at a Single-Center in Japan
- PMID: 39766595
- PMCID: PMC11672654
- DOI: 10.3390/antibiotics13121205
A 15-Year Observational Cohort of Acute Empyema at a Single-Center in Japan
Abstract
Introduction: Despite the advancements in diagnostic methods and antibiotic treatment, empyema is a critical respiratory infection, showing a high mortality rate of 10-25%. Patients and Methods: To evaluate the bacterial etiology and prognostic factors of acute empyema, we conducted this long-term retrospective cohort study at our institute between 2008 and 2022. Results: A total of 80 patients were enrolled in this cohort. The median age was 72 years (range 19 to 93 years), and 61 (76%) were male. The most common underlying disease was malignancy, seen in 28 (35%). The mean Charlson comorbidity index (CCI) was 2.7 (±2.4). The 30-day and in-hospital mortality were 9 (11%) and 15 (19%), respectively. Univariate analysis revealed that healthcare-associated infection, inappropriate treatment, high CCI score, performance status (PS) of 2-4, and isolation of potentially drug-resistant (PDR) pathogens were poor prognostic factors. Finally, multivariate analysis showed that high CCI score (p = 0.009) and isolation of PDR pathogens (p = 0.011) were independent poor prognostic factors for in-hospital death in acute empyema. Conclusions: We found that higher CCI scores and isolation of PDR pathogens were independent poor prognostic factors for in-hospital mortality among empyema patients.
Keywords: dysbiosis; effusion; empyema; pleural infection; potential drug-resistant pathogen.
Conflict of interest statement
Authors have no conflicts of interests.
Figures
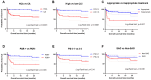
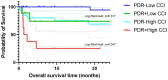
References
-
- Asai N., Suematsu H., Hagihara M., Nishiyama N., Kato H., Sakanashi D., Koizumi Y., Yamagishi Y., Mikamo H. The etiology and bacteriology of healthcare-associated empyema are quite different from those of community-acquired empyema. J. Infect. Chemother. 2017;23:661–667. doi: 10.1016/j.jiac.2017.04.011. - DOI - PubMed
LinkOut - more resources
Full Text Sources

