Results of an Online Survey on Intensive Care Management of Patients with Aneurysmal Subarachnoid Hemorrhage in German-Speaking Countries
- PMID: 39768538
- PMCID: PMC11676747
- DOI: 10.3390/jcm13247614
Results of an Online Survey on Intensive Care Management of Patients with Aneurysmal Subarachnoid Hemorrhage in German-Speaking Countries
Abstract
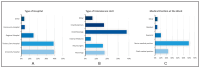
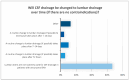
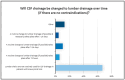
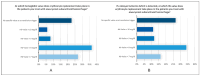
Background: The clinical course of patients with aneurysmal SAH (aSAH) is often dynamic and highly unpredictable. Since its management varies between hospitals despite guidelines, this survey aimed to assess the current state of intensive care treatment for aSAH in the German-speaking region and provide insights that could aid standardization of care for aSAH patients in the intensive care setting. Methods: From February 2023 to April 2023, medical professionals of the German Interdisciplinary Association for Intensive Care and Emergency Medicine (DIVI), the Initiative of German Neuro-Intensive Trial Engagement (IGNITE) network and manually recorded clinics with intensive care units were invited to participate in a standardized anonymous online questionnaire including 44 questions. The questionnaire was validated in multiple steps by experts of different specialties including those from the DIVI. A descriptive data analysis was carried out. Results: A total of 135 out of 220 participants answered the survey completely. The results showed that most patients were treated in anesthesia-led intensive care units at university and maximum care hospitals. Aneurysms were usually treated within 24 h after bleeding. If vasospasm was detected, induced hypertension was usually implemented as the first treatment option. In refractory vasospasm, interventional spasmolysis with calcium antagonists was usually carried out (81%), despite unclear evidence. There were significant discrepancies in blood pressure target values, particularly after aneurysm repair or after delayed cerebral ischemia (DCI), as well as in hemoglobin limit values for erythrocyte substitution. Despite the limited level of evidence, most institutions used temperature management (68%), including hypothermia (56%), for severe cases. Conclusions: While we anticipated variations between individual intensive care facilities, our survey identified numerous similarities in the treatment of aSAH patients. Methods such as interventional spasmolysis and temperature management were used frequently despite limited evidence. Our results can serve as a fundamental framework for formulating recommendations for intensive care treatment and planning of multicenter studies.
Keywords: intensive care medicine; multimodal monitoring; subarachnoid hemorrhage; vasospasm.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

Similar articles
-
Economic and Humanistic Burden of Cerebral Vasospasm and Its Related Complications after Aneurysmal Subarachnoid Hemorrhage: A Systematic Literature Review.Neurol Ther. 2022 Jun;11(2):597-620. doi: 10.1007/s40120-022-00348-6. Epub 2022 Apr 20. Neurol Ther. 2022. PMID: 35441974 Free PMC article. Review.
-
A Survey on Monitoring and Management of Cerebral Vasospasm and Delayed Cerebral Ischemia After Subarachnoid Hemorrhage: The Mantra Study.J Neurosurg Anesthesiol. 2024 Jul 1;36(3):258-265. doi: 10.1097/ANA.0000000000000923. Epub 2023 May 26. J Neurosurg Anesthesiol. 2024. PMID: 37254166
-
Associations between endothelin polymorphisms and aneurysmal subarachnoid hemorrhage, clinical vasospasm, delayed cerebral ischemia, and functional outcome.J Neurosurg. 2018 May;128(5):1311-1317. doi: 10.3171/2016.12.JNS162594. Epub 2017 May 26. J Neurosurg. 2018. PMID: 28548598
-
Detection of delayed cerebral ischemia using objective pupillometry in patients with aneurysmal subarachnoid hemorrhage.J Neurosurg. 2020 Jan 1;132(1):27-32. doi: 10.3171/2018.9.JNS181928. Epub 2019 Jan 11. J Neurosurg. 2020. PMID: 30641848
-
Clinical Burden of Angiographic Vasospasm and Its Complications After Aneurysmal Subarachnoid Hemorrhage: A Systematic Review.Neurol Ther. 2023 Apr;12(2):371-390. doi: 10.1007/s40120-022-00436-7. Epub 2023 Jan 7. Neurol Ther. 2023. PMID: 36609962 Free PMC article. Review.
Cited by
-
Acute care of aneurysmal subarachnoid hemorrhage: practical consensus statement from a multidisciplinary group of German-speaking neurointensivists and neuroradiologists on behalf of the DIVI neurology section.Neurol Res Pract. 2025 Jul 30;7(1):54. doi: 10.1186/s42466-025-00407-x. Neurol Res Pract. 2025. PMID: 40739674 Free PMC article.
References
-
- Hoh B.L., Ko N.U., Amin-Hanjani S., Chou S.H.-Y., Cruz-Flores S., Dangayach N.S., Derdeyn C.P., Du R., Hänggi D., Hetts S.W., et al. 2023 Guideline for the Management of Patients With Aneurysmal Subarachnoid Hemorrhage: A Guideline From the American Heart Association/American Stroke Association. Stroke. 2023;54:E314–E370. doi: 10.1161/STR.0000000000000436. - DOI - PubMed
-
- Goursaud S., de Lizarrondo S.M., Grolleau F., Chagnot A., Agin V., Maubert E., Gauberti M., Vivien D., Ali C., Gakuba C. Delayed Cerebral Ischemia After Subarachnoid Hemorrhage: Is There a Relevant Experimental Model? A Systematic Review of Preclinical Literature. Front. Cardiovasc. Med. 2021;8:752769. doi: 10.3389/fcvm.2021.752769. - DOI - PMC - PubMed
-
- Psychogios K., Tsivgoulis G. Subarachnoid hemorrhage and vasospasm: Clinical implications and management strategies. Pract. Neurol. 2019;19:39–42.
LinkOut - more resources
Full Text Sources
Miscellaneous

