Standardizing the reporting of cholangiocarcinoma: the society of abdominal radiology disease focused panel on cholangiocarinoma lexicon
- PMID: 39775025
- PMCID: PMC12181104
- DOI: 10.1007/s00261-024-04769-9
Standardizing the reporting of cholangiocarcinoma: the society of abdominal radiology disease focused panel on cholangiocarinoma lexicon
Abstract
In March 2023, the Society of Abdominal Radiology (SAR) Disease Focused Panel (DFP) on Cholangiocarcinoma (CCA) was formed. One of its initial tasks was for creation of a lexicon specific for CCA to complement the terms related to the Liver Imaging Reporting and Data System (LI-RADS) category M. A committee was formed and vetted 15 unique terms for CCA. The multidisciplinary members of the DFP passed each term by over 90% approval. The purpose of this paper is to describe the process for developing the lexicon, introduce the lexicon terms, and provide a pictorial atlas of the 15 vetted terms relating to the imaging findings of CCA.
Keywords: Cholangiocarcinoma; Lexicon; Liver cancer.
© 2024. The Author(s).
Conflict of interest statement
Declarations. Competing interests: The authors declare no competing interests.
Figures
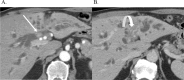

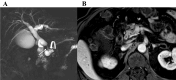
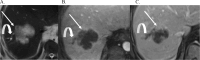




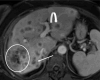
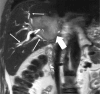
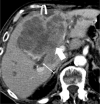


References
-
- Marks RM, Fung A, Cruite I, Blevins K, Lalani T, Horvat N, et al. The adoption of LI-RADS: a survey of non-academic radiologists. Abdom Radiol (NY). 2023;48(8):2514–24. Epub 20230526. doi: 10.1007/s00261-023-03951-9. PubMed PMID: 37233747. - PubMed
-
- Marks RM, Masch WR, Chernyak V. LI-RADS: Past, Present, and Future, From the AJR Special Series on Radiology Reporting and Data Systems. AJR Am J Roentgenol. 2021 Feb;216(2):295–304. 10.2214/AJR.20.24272. Epub 2020 Dec 23. PMID: 33052720. - PubMed
-
- Pesapane F, Tantrige P, De Marco P, Carriero S, Zugni F, Nicosia L, Bozzini AC, Rotili A, Latronico A, Abbate F, Origgi D, Santicchia S, Petralia G, Carrafiello G, Cassano E. Advancements in Standardizing Radiological Reports: A Comprehensive Review. Medicina (Kaunas). 2023 Sep 17;59(9):1679. 10.3390/medicina59091679. PMID: 37763797; PMCID: PMC10535385. - PMC - PubMed
-
- American College of Radiology Committee on LI-RADS®. The LI-RADS v2018 Manual 2018. Available from: https://www.acr.org/-/media/ACR/Files/Clinical-Resources/LIRADS/LI-RADS-.... Accessed on April 12, 2024.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

