Predictive value and optimal cut-off level of high-sensitivity troponin T in patients with acute pulmonary embolism
- PMID: 39778527
- PMCID: PMC11725470
- DOI: 10.3904/kjim.2024.131
Predictive value and optimal cut-off level of high-sensitivity troponin T in patients with acute pulmonary embolism
Abstract
Background/aims: Elevated troponin levels predict in-hospital mortality and influence decisions regarding thrombolytic therapy in patients with acute pulmonary embolism (PE). However, the usefulness of high-sensitivity troponin T (hsTnT) regarding PE remains uncertain. We aimed to establish the optimal cut-off level and compare its performance for precise risk stratification.
Methods: 374 patients diagnosed with acute PE were reviewed. PE-related adverse outcomes, a composite of PE-related deaths, cardiopulmonary resuscitation incidents, systolic blood pressure < 90 mmHg, and all-cause mortality within 30 days were evaluated. The optimal hsTnT cut-off for all-cause mortality, and the net reclassification index (NRI) was used to assess the incremental value in risk stratification.
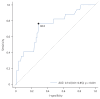
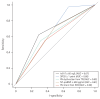
Results: Among 343 normotensive patients, 17 (5.0%) experienced all-cause mortality, while 40 (10.7%) had PE-related adverse outcomes. An optimal hsTnT cut-off value of 60 ng/L for all-cause mortality (AUC 0.74, 95% CI 0.61-0.85, p < 0.001) was identified, which was significantly associated with PE-related adverse outcomes (OR 4.07, 95% CI 2.06-8.06, p < 0.001). Patients with hsTnT ≥ 60 ng/L were older, hypotensive, had higher creatinine levels, and right ventricular dysfunction signs. Combining hsTnT ≥ 60 ng/L with simplified pulmonary embolism severity index ≥1 provided additional prognostic information. Reclassification analysis showed a significant shift in risk categories, with an NRI of 1.016 ± 0.201 (p < 0.001).
Conclusion: We refined troponin's predictive value in patients with acute PE, proposing a new cut-off value of hsTnT ≥ 60 ng/L. Validation through large-scale studies is essential to offer clinically useful guidance for managing patient population.
Keywords: Biomarker; Pulmonary embolism; Risk assessment; Troponin T.
Conflict of interest statement
The authors disclose no conflicts.
Figures

Similar articles
-
Predictive value of the high-sensitivity troponin T assay and the simplified Pulmonary Embolism Severity Index in hemodynamically stable patients with acute pulmonary embolism: a prospective validation study.Circulation. 2011 Dec 13;124(24):2716-24. doi: 10.1161/CIRCULATIONAHA.111.051177. Epub 2011 Nov 14. Circulation. 2011. PMID: 22082681
-
Age-adjusted high-sensitivity troponin T cut-off value for risk stratification of pulmonary embolism.Eur Respir J. 2015 May;45(5):1323-31. doi: 10.1183/09031936.00174514. Epub 2015 Jan 22. Eur Respir J. 2015. PMID: 25614162
-
Optimal Cutoff Values and Utility of High-Sensitivity Troponin T and NT-proBNP for the Risk Stratification of Patients with Acute Pulmonary Embolism.Clin Chem. 2025 May 2;71(5):559-566. doi: 10.1093/clinchem/hvae212. Clin Chem. 2025. PMID: 39704155
-
Elevated serum cardiac troponin and mortality in acute pulmonary embolism: Systematic review and meta-analysis.Respir Med. 2019 Oct;157:26-35. doi: 10.1016/j.rmed.2019.08.011. Epub 2019 Aug 23. Respir Med. 2019. PMID: 31476570
-
Prognostic value of right ventricular dysfunction or elevated cardiac biomarkers in patients with low-risk pulmonary embolism: a systematic review and meta-analysis.Eur Heart J. 2019 Mar 14;40(11):902-910. doi: 10.1093/eurheartj/ehy873. Eur Heart J. 2019. PMID: 30590531 Free PMC article.
References
-
- Konstantinides SV, Meyer G, Becattini C, et al. 2019 ESC Guidelines for the diagnosis and management of acute pulmonary embolism developed in collaboration with the European Respiratory Society (ERS) Eur Heart J. 2020;41:543–603. - PubMed
-
- Westermann D, Neumann JT, Sörensen NA, Blankenberg S. High-sensitivity assays for troponin in patients with cardiac disease. Nat Rev Cardiol. 2017;14:472–483. - PubMed
-
- Giannitsis E, Katus HA. Cardiac troponin level elevations not related to acute coronary syndromes. Nat Rev Cardiol. 2013;10:623–634. - PubMed
-
- Giannitsis E, Kurz K, Hallermayer K, Jarausch J, Jaffe AS, Katus HA. Analytical validation of a high-sensitivity cardiac troponin T assay. Clin Chem. 2010;56:254–261. - PubMed
-
- Mitchell C, Rahko PS, Blauwet LA, et al. Guidelines for performing a comprehensive transthoracic echocardiographic examination in adults: recommendations from the American Society of Echocardiography. J Am Soc Echocardiogr. 2019;32:1–64. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous
