Adolescent thoracic scoliosis due to giant ganglioneuroma: a two-case report and literature review
- PMID: 39780926
- PMCID: PMC11704773
- DOI: 10.18999/nagjms.86.4.711
Adolescent thoracic scoliosis due to giant ganglioneuroma: a two-case report and literature review
Abstract
Ganglioneuromas are rare benign tumors that arise from the sympathetic nervous system. The presentation of tumors is variable and associated with adolescent thoracic scoliosis. Herein, we present two case reports and a review of literature. The two cases involved 10 and 13-year-old patients who were asymptomatic for muscle pain or weakness, and ganglioneuromas were incidentally detected through imaging screening. Both patients underwent a two-stage surgery. The first stage involved detachment of the tumor from the spinal cord and simultaneously performing deformity correction surgery from the posterior aspect. The second stage was resection of the ganglioneuroma through the anterior approach without neurological problems. A two-stage surgery was necessary to excise the tumor and correct the deformity, thereby avoiding neurological problems and concurrently establish a pathological diagnosis. Commencing with the posterior approach proved to be safe and was more effective.
Keywords: adolescent thoracic scoliosis; corrective fusion; ganglioneuroma; tumor resection; two-stage surgery.
Conflict of interest statement
The authors have no conflicts of interest to disclose.
Figures
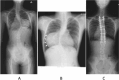
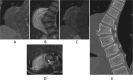
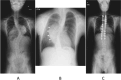

References
-
- Qiu Y, Wang S, Wang B, Zhu F. Adolescent thoracolumbar scoliosis secondary to ganglioneuroma: A two case report. Spine (Phila Pa 1976). 2007;32(10):E326–E329. doi: 10.1097/01.brs.0000261628.77342.ba. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
