Fluoroscopy-guided aspiration of the acutely dislocated total hip arthroplasty: a feasible, high-yield, and safe procedure
- PMID: 39792214
- PMCID: PMC11723859
- DOI: 10.1186/s13244-024-01880-9
Fluoroscopy-guided aspiration of the acutely dislocated total hip arthroplasty: a feasible, high-yield, and safe procedure
Erratum in
-
Correction: Fluoroscopy-guided aspiration of the acutely dislocated total hip arthroplasty: a feasible, high-yield, and safe procedure.Insights Imaging. 2025 Apr 14;16(1):85. doi: 10.1186/s13244-025-01963-1. Insights Imaging. 2025. PMID: 40227545 Free PMC article. No abstract available.
Abstract
Objective: To determine the feasibility, yield, and safety of fluoroscopic-guided aspiration of the acutely dislocated total hip arthroplasty (AD-THA).
Materials and methods: IRB-approved, retrospective review of fluoroscopic-guided aspirations of AD-THA (January 2005-December 2023) was performed. Data from electronic charts and fluoroscopy images/reports were obtained. Positive yield was defined as spontaneous aspirate or saline rinse adequate for microbiology analysis. Sub-analysis by needle target (acetabular cup or femur) was performed for spontaneous aspiration rate, aspirate volume and fluoroscopy time. Differences between groups were analyzed with unpaired, t-test (2-tail) and between proportions with Fisher's exact test, with significance p < 0.05.
Results: Aspiration of 20 AD-THA in 19 patients (12 female, mean age (SD) of 73 years (16)) targeted the acetabular cup in 45% (9/20) or femur in 55% (11/20) of cases. Positive yield was obtained in 95% (19/20), with spontaneous aspirate in 75% (15/20) and saline rinse in 20% (4/20) of cases; in 5% (1/20), no diagnostic sample was obtained. Spontaneous aspirate mean volume (SD, range) for all cases was 8.3 mL (6.9, 0.2-25), and higher when targeting the acetabular cup 11.2 mL (6.9, 5-25) versus the femur 4.0 mL (4.4, 0.2-12) (p = 0.026). The rate of spontaneous aspiration was higher for the acetabular cup 100% (9/9) versus the femur 55% (6/11) (p = 0.038). The mean fluoroscopy time (SD, range) for all cases was 43 s (25, 19-102), and shorter for targeting the acetabular cup 32 s (16, 19-75) versus the femur 56 s (28, 28-102) (p = 0.034). No immediate complications occurred in all aspirations.
Conclusion: Fluoroscopy-guided aspiration of AD-THA is a feasible, high-yield, and safe procedure. Targeting the acetabular cup results in a higher rate of spontaneous aspirate, larger aspiration volume, and lower fluoroscopy time.
Critical relevance statement: Although technically more challenging, radiologists should feel confident aspirating the acutely dislocated total hip arthroplasty (AD-THA) under fluoroscopic guidance.
Key points: Total hip arthroplasty (THA) infection can be evaluated with synovial fluid aspiration. Fluoroscopic-guided aspiration of the dislocated THA is feasible, high-yield, and safe. Targeting of the acetabular cup is recommended over the femoral prosthetic component. Acetabular cup targeting gives larger, spontaneous aspirates with lower fluoroscopy time.
Keywords: Dislocation; Fluoroscopy; Image-guided hip aspiration; Intervention; Total hip arthroplasty.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: Approval by the Ottawa Hospital Research Institute Research Ethics Board was obtained (OHSN-REB Protocol #: 20220692-01H). Written informed consent was waived by the Ottawa Hospital Research Institute Research Ethics Board. Consent for publication: Not applicable. Competing interests: The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Figures
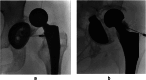
References
-
- Ahmed SS, Begum F, Kayani B, Haddad FS (2019) Risk factors, diagnosis and management of prosthetic joint infection after total hip arthroplasty. Expert Rev Med Devices 16:1063–1070 - PubMed
LinkOut - more resources
Full Text Sources

