Role of Medical Nutrition Therapy as Treatment of Sarcopenia in Older People with Type 2 Diabetes
- PMID: 39796606
- PMCID: PMC11723121
- DOI: 10.3390/nu17010172
Role of Medical Nutrition Therapy as Treatment of Sarcopenia in Older People with Type 2 Diabetes
Abstract
Background: Globally, the progressive increase in the aging population has led to social and health problems associated with age-related chronic diseases, such as type 2 diabetes mellitus (T2DM) and sarcopenia. Recent studies have highlighted that sarcopenia and diabetes have a bidirectional relationship. Nutritional therapy is a key element in the treatment of both sarcopenia and diabetes. To date, there are no nutritional guidelines for the management of sarcopenia in T2DM. The aim of this study was to evaluate the efficacy of a muscle-targeted nutritional intervention in older people with sarcopenia and type 2 diabetes based on the Italian nutrition guidelines.
Methods: A total of 211 subjects (117 M and 94 F) affected by T2DM with a mean age of 74 ± 6.0 years were screened for sarcopenia, using EWGSOP2 diagnosis criteria, and enrolled to receive personalized dietary plans with two main targets: a daily energy intake of 25-30 kcal/kg body weight and a daily protein intake of at least 1.1-1.2 g/kg body weight.
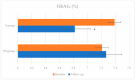
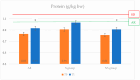
Results: In total, 34 subjects (24 M and 10 F) were sarcopenic with a prevalence of 16%, which was higher in men. After six months of treatment, handgrip strength increased by 0.83 kg (19.57 ± 5.70 kg vs. 20.40 ± 6.10 kg, p = 0.649), protein intake improved (0.91 ± 0.28 g/kg body weight vs. 1.03 ± 0.40 g/kg body weight, p = 0.115), and the glycated hemoglobin decreased (7.39 ± 0.49% to 6.82 ± 0.98%, p = 0.010). Seven younger subjects had an improvement of sarcopenia with a decrease in HbA1c (7.50 ± 0.59% vs. 6.91 ± 0.79, p = 0.19). The difference over time in the consumption of saturated fatty acids (OR 0.6, 95% CI 0.33-1.09, p = 0.096) and simple sugars (OR 0.91, 95% CI 0.80-1.01, p = 0.090) appeared to be associated with an improvement of sarcopenia status. A total of 177 subjects did not meet the criteria for a diagnosis of sarcopenia, and 148 subjects were assessed. The handgrip strength (26.22 ± 9.36 vs. 26.18 ± 9.24 kg, p0.974) and the glycated hemoglobin (7.21 ± 1.07 vs. 7.27 ± 0.98%, p = 0.735) remained stable over time, while protein intake at six months increased (0.81 ± 0.29 vs. 0.91 ± 0.29 g/kg body weight, p = 0.024). Four people were diagnosed with sarcopenia at follow-up, with a lower handgrip strength test result. These subjects were older and had worse glycemic control (HbA1c + 0.5%).
Conclusions: Lifestyle modification is important to prevent or reverse the development of the disease. Nutritional therapy in this population is therefore aimed at meeting all nutritional needs and promoting better glycemic control, in terms of glycated hemoglobin, in order to reduce the development of sarcopenia. Although promising, the intervention requires validation in larger studies with control groups.
Keywords: body composition; diet; nutritional status; sarcopenia; type 2 diabetes.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
References
-
- Sun H., Saeedi P., Karuranga S., Pinkepank M., Ogurtsova K., Duncan B.B., Stein C., Basit A., Chan J.C.N., Mbanya J.C., et al. IDF Diabetes Atlas: Global, regional and country-level diabetes prevalence estimates for 2021 and projections for 2045. Diabetes Res. Clin. Pract. 2022;183:109119. doi: 10.1016/j.diabres.2021.109119. Erratum in Diabetes Res. Clin. Pract. 2023, 204, 110945. - DOI - PMC - PubMed
-
- Rosenberg I.H. Summary Comments. Am. J. Clin. Nutr. 1989;50:1231–1233. doi: 10.1093/ajcn/50.5.1231. - DOI
-
- Cruz-Jentoft A.J., Bahat G., Bauer J., Boirie Y., Bruyère O., Cederholm T., Cooper C., Landi F., Rolland Y., Sayer A.A., et al. Sarcopenia: Revised European consensus on definition and diagnosis. Age Ageing. 2019;48:16–31. doi: 10.1093/ageing/afy169. Erratum in Age Ageing 2019, 48, 601. - DOI - PMC - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical