Clinical Predispositions, Features, and Outcomes of Infections with Carbapenem-resistant Enterobacterales among Critical Care Patients
- PMID: 39802247
- PMCID: PMC11719537
- DOI: 10.5005/jp-journals-10071-24876
Clinical Predispositions, Features, and Outcomes of Infections with Carbapenem-resistant Enterobacterales among Critical Care Patients
Abstract
Background: Carbapenem-resistant Enterobacterales (CRE) infections pose a significant global public health threat. We aimed to assess the risk variables, clinical characteristics, and outcomes of CRE-caused infections in criticalcare patients.
Patients and methods: This prospective study enrolled 181 adult patients infected with Enterobacterales in the intensive care unit (ICU). Patients underwent clinical assessment and monitoring throughout their ICU stay. Carbapenem resistance was identified through antibiotic susceptibility testing and multiplex molecular detection of carbapenemase-encoding genes.
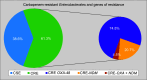
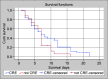
Results: The mean age of patients was 67.99 ± 12.89 years, with 71.3% being males. Of 181 patients, 111 (61.3%) were found to have CRE infections, including 39 Klebsiella pneumoniae and 31 Escherichia coli isolates. The CRE isolates showed the predominance of the OXA-48 (74.8%), followed by the NewDelhi Metallobetalactamase (NDM) carbapenemase genes (20.7%). The risk factors associated with CRE infection included high sequential organ failure assessment (SOFA) score, prolonged length of stay (LOS) in ICU, prior use of broad-spectrum antimicrobials, hemodialysis, plasma exchange, and prolonged mechanical ventilation. Carbapenem-resistant Enterobacterales infections significantly required longer LOS, more need for mechanical ventilation, and exhibited lower rates of bacterial elimination than carbapenem-susceptible Enterobacterales (CSE) infections. The type of resistance gene did not significantly influence the mortality rate among CRE patients. The successful treatment of OXA-48-positive CRE showed a strong correlation with tigecycline and colistin antibiotics.
Conclusion: Carbapenem-resistant Enterobacterales infection in ICU patients was associated with adverse outcomes. Identification of high-risk patients is essential for early diagnosis and appropriate management. Therefore, it is crucial to improve infection control methods and implement antimicrobial stewardship to avoid spreading infections.
How to cite this article: Shoala ARK, Nassar Y, El-Kholy AA, Soliman NS, Abdel-Fattah A, El-Ghawaby H. Clinical Predispositions, Features, and Outcomes of Infections with Carbapenem-resistant Enterobacterales among Critical Care Patients. Indian J Crit Care Med 2025;29(1):36-44.
Keywords: Carbapenem-resistant Enterobacterales; Carbapenemase; NDM gene; OXA-48 gene; Outcome; Risk factors.
Copyright © 2025; The Author(s).
Conflict of interest statement
Source of support: The study was supported by a Pfizer General Research Grant; Pfizer-2019 for a study under the title (Genomic Characterization of Carbapenem-resistant Enterobacteriaceae in Egypt) Conflict of interest: NoneConflict of interest: None
Figures
Similar articles
-
Association Between Types of Carbapenemase and Clinical Outcomes of Infection Due to Carbapenem Resistance Enterobacterales.Infect Drug Resist. 2022 Jun 13;15:3025-3037. doi: 10.2147/IDR.S363588. eCollection 2022. Infect Drug Resist. 2022. PMID: 35720254 Free PMC article.
-
Continuous Evolution: Perspective on the Epidemiology of Carbapenemase Resistance Among Enterobacterales and Other Gram-Negative Bacteria.Infect Dis Ther. 2021 Mar;10(1):75-92. doi: 10.1007/s40121-020-00395-2. Epub 2021 Jan 25. Infect Dis Ther. 2021. PMID: 33492641 Free PMC article. Review.
-
Phenotypic and molecular characterization of multidrug-resistant Enterobacterales isolated from clinical samples in Palestine: a focus on extended-spectrum β-lactamase- and carbapenemase-producing isolates.BMC Infect Dis. 2024 Aug 12;24(1):812. doi: 10.1186/s12879-024-09726-x. BMC Infect Dis. 2024. PMID: 39134953 Free PMC article.
-
Prevalence and risk factors of carbapenem-resistant Enterobacterales positivity by active screening in intensive care units in the Henan Province of China: A multi-center cross-sectional study.Front Microbiol. 2022 Sep 14;13:894341. doi: 10.3389/fmicb.2022.894341. eCollection 2022. Front Microbiol. 2022. PMID: 36187994 Free PMC article.
-
Microbiology of Meropenem-Vaborbactam: A Novel Carbapenem Beta-Lactamase Inhibitor Combination for Carbapenem-Resistant Enterobacterales Infections.Infect Dis Ther. 2020 Dec;9(4):757-767. doi: 10.1007/s40121-020-00350-1. Epub 2020 Oct 5. Infect Dis Ther. 2020. PMID: 33017041 Free PMC article. Review.
References
-
- Sikora A, Zahra F. Treasure Island (FL): StatPearls Publishing; 2024. Nosocomial Infections.32644738
-
- Abou-assy RS, Aly MM, Amashah RH, Jastaniah SD, Al Deen HM. Epidemiology of carbapenem resistance Enterobacterales in Saudi Arabia: A systematic review. J Contemp Med Sci. 2022;8(1):18–26. doi: 10.22317/jcms.v8i1.1168. - DOI
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous