An Acta Orthopaedica educational article: Treatment of pediatric spondylolysis and spondylolisthesis
- PMID: 39804815
- PMCID: PMC11734530
- DOI: 10.2340/17453674.2024.42450
An Acta Orthopaedica educational article: Treatment of pediatric spondylolysis and spondylolisthesis
Abstract
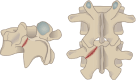
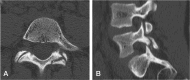
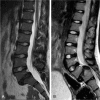
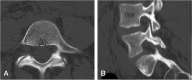
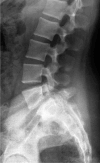
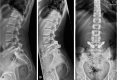
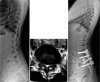
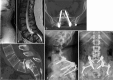
Spondylolysis is defined as a defect or elongation in the pars interarticularis of the lumbar spine, either unilateral or bilateral. Growing children with bilateral spondylolysis may develop spondylolisthesis, i.e., forward slipping of the affected vertebra. The etiology of spondylolysis is regarded as a stress fracture due to repetitive loading associated with a genetic predisposition. Lumbar magnetic resonance imaging (MRI) shows an increased signal intensity before an actual fracture line develops. In low grade spondylolisthesis, two-thirds of children with acute pediatric spondylolysis will undergo bony union with early activity restriction. Health-related quality of life is improved in patients achieving bony union as compared with patients having non-union, of which one-fourth will additionally develop spondylolisthesis. In patients with high-grade spondylolisthesis, defined as a more than 50% forward slippage of the affected vertebra, spinal fusion is recommended to prevent further progression.
Figures
References
-
- Fredrickson B E, Baker D, McHolick W J, Yuan H A, Lubicky J P. The natural history of spondylolysis and spondylolisthesis. J Bone Joint Surg Am 1984; 66(5): 699-707. - PubMed
-
- Jackson D W, Wiltse L L, Cirincoine R J. Spondylolysis in the female gymnast. Clin Orthop Relat Res 1976; 117:68-73. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous

