Evaluating One-Week Post-Casting Alignment Checks and Surgical Intervention Rates in Pediatric Type IIA Supracondylar Humeral Fractures
- PMID: 39811178
- PMCID: PMC11726482
Evaluating One-Week Post-Casting Alignment Checks and Surgical Intervention Rates in Pediatric Type IIA Supracondylar Humeral Fractures
Abstract
Background: This study aims to determine the rate of surgical intervention in children with type IIA supracondylar humerus fractures (SCHF) following routine post-casting radiographic assessment. We hypothesized that no cases would convert to operative management following one-week post-casting alignment assessments.
Methods: This single-center retrospective study focused on pediatric patients diagnosed with type IIA SCHF from 2019 to 2022. Patients were treated with initial long arm cast immobilization, followed by a one-week post-casting radiographic alignment check in cast. Fractures were graded in consensus using the Wilkins-Modified Gartland classification system by three fellowship-trained pediatric orthopaedic surgeons. Demographics, casting details, follow-up dates, and treatment histories were examined. Alignment was considered acceptable or requiring surgery based on the treating surgeons' discretion. The study excluded patients with concomitant ipsilateral upper extremity fractures, flexion-type fractures, lost to follow-up before cast removal, or with type I, IIB or III SCHFs.
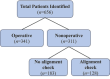
Results: Of the 128 patients reviewed in our study, 85 were classified as type IIA SCHF by consensus. The cohort had an average age of 4.2 years (range: 1.1-10.2 years) and was 52% male. The patient population was ethnically diverse, with Hispanic patients constituting the majority (56%), followed by White patients (26%), Black patients (9%), and Asian patients (8%).Patients presented for definitive treatment an average of 2.8 days post-injury and spent an average of 28.8 days in casts. Alignment checks occurred an average of 10.3 days post-injury (SD ±2.5 days). Alignment shifts were noted in 7.1% of cases (n=6). Of these six cases, two were assessed by surgeons as having acceptable alignment, not requiring further intervention. The remaining four cases underwent closed reduction and percutaneous pinning. The rate of conversion to surgical treatment for type IIA supracondylar humerus fractures in our study was 4.7%.
Conclusion: This investigation found that 4.7% of nonoperative type IIA SCHFs converted to operative treatment at the one-week post-casting alignment check. Future studies are warranted to determine specific risk factors for alignment loss in type IIA SCHFs. Level of Evidence: IV.
Keywords: fracture stability; pediatric supracondylar fracture; pediatrics; post-casting care; routine radiographs; supracondylar fracture; type 2A SCHF; type IIA SCHF.
Copyright © The Iowa Orthopaedic Journal 2024.
Conflict of interest statement
Disclosures: The authors report no potential conflicts of interest related to this study.
Figures
Similar articles
-
Medium-term clinical results in the treatment of supracondylar humeral fractures in children: does the surgical approach impact outcomes?J Orthop Traumatol. 2024 Sep 11;25(1):43. doi: 10.1186/s10195-024-00781-3. J Orthop Traumatol. 2024. PMID: 39261419 Free PMC article.
-
Pediatric Type II Supracondylar Humerus Fractures: Factors Associated With Successful Closed Reduction and Immobilization.J Pediatr Orthop. 2020 Sep;40(8):e690-e696. doi: 10.1097/BPO.0000000000001586. J Pediatr Orthop. 2020. PMID: 32776771
-
Single-surgeon perspective: is there ever a need to open extension-type supracondylar fractures?Ir J Med Sci. 2023 Dec;192(6):2845-2849. doi: 10.1007/s11845-023-03294-w. Epub 2023 Feb 28. Ir J Med Sci. 2023. PMID: 36849653
-
Low incidence of ulnar nerve injury with crossed pin placement for pediatric supracondylar humerus fractures using a mini-open technique.J Orthop Trauma. 2005 Mar;19(3):158-63. doi: 10.1097/00005131-200503000-00002. J Orthop Trauma. 2005. PMID: 15758668 Review.
-
Does posterior approach always lead to poor functional and cosmetic outcomes in displaced pediatric supracondylar humeral fractures?Ulus Travma Acil Cerrahi Derg. 2023 Apr;29(4):523-529. doi: 10.14744/tjtes.2022.29403. Ulus Travma Acil Cerrahi Derg. 2023. PMID: 36995201 Free PMC article. Review.
References
-
- Hope N, Varacallo M. StatPearls. StatPearls Publishing; 2023. Supracondylar Humerus Fractures. Accessed January 20 2024 http://www.ncbi.nlm.nih.gov/books/NBK560933/. In:
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous