Urinary biomarkers for diagnosing acute kidney injury in sepsis in the emergency department
- PMID: 39811377
- PMCID: PMC11731463
- DOI: 10.1016/j.heliyon.2024.e41252
Urinary biomarkers for diagnosing acute kidney injury in sepsis in the emergency department
Abstract
Background: Development of acute kidney injury (AKI) in patients with sepsis is associated with increased mortality, highlighting the importance of early detection and management. However, baseline creatinine or urine output measurements are required for AKI diagnosis, which can be challenging in emergency departments (EDs). We aimed to evaluate the association between urinary biomarkers and the AKI diagnosis or 30-day survival status in patients with sepsis in the ED.
Methods: This prospective observational study enrolled patients from a single ED. We enrolled adult patients presenting to the ED with symptoms suggestive of infection and an initial quick sequential organ failure assessment score ≥2. Initial urine samples were collected, and urinary biomarkers (dickkopf-3, soluble triggering receptor expressed on myeloid cells-1, kidney injury molecule-1, neutrophil gelatinase-associated lipocalin (NGAL), and tissue inhibitor of metalloproteinases-2 (TIMP-2), and insulin-like growth factor binding protein-7 (IGFBP-7), and TIMP-2 × IGFBP-7) were analyzed using an enzyme-linked immunosorbent assay kit. Multivariable logistic regression models were used to evaluate biomarker performance.
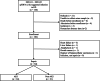
Results: Of 84 patients, 63 (75.0 %) were diagnosed with AKI and 16 (19.0 %) died within 30 days. None of the urinary biomarkers demonstrated significant differences between the survivors and non-survivors. NGAL (p = 0.014) and TIMP-2 × IGFBP-7 (p = 0.027) levels were different between the AKI and non-AKI groups. The multivariable logistic regression model suggested a higher area under the receiver operating characteristic curve for models, including TIMP-2 × IGFBP-7 (from 0.853 to 0.889, p = 0.018).
Conclusion: None of the urinary biomarkers in the initial urine sample demonstrated an independent association with AKI diagnosis or 30-day survival status in patients with sepsis presenting to the ED. Further studies with larger population are necessary to confirm its clinical utility and explore its role.
Keywords: Acute kidney injury; Biomarkers; Emergency service; Hospital; Insulin-like growth factor binding proteins; Sepsis; Tissue inhibitor of Metalloproteinase-2.
© 2024 The Authors.
Conflict of interest statement
The authors declare the following financial interests/personal relationships which may be considered as potential competing interests: Inwon Park reports financial support was provided by 10.13039/501100003725National Research Foundation (NRF) of Korea. Inwon Park reports financial support was provided by Korea Health Industry Development Institute (KHIDI). Inwon Park reports financial support was provided by Seoul 10.13039/100018366National University 10.13039/100008212College of Medicine. Inwon Park reports financial support was provided by Seoul 10.13039/100018366National University Bundang Hospital. If there are other authors, they declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Similar articles
-
Association of Renal Stress/Damage and Filtration Biomarkers with Subsequent AKI during Hospitalization among Patients Presenting to the Emergency Department.Clin J Am Soc Nephrol. 2016 Jun 6;11(6):938-946. doi: 10.2215/CJN.10551015. Epub 2016 Mar 29. Clin J Am Soc Nephrol. 2016. PMID: 27026519 Free PMC article.
-
Diagnostic and prognostic value of neutrophil gelatinase-associated lipocalin, matrix metalloproteinase-9, and tissue inhibitor of matrix metalloproteinases-1 for sepsis in the Emergency Department: an observational study.Crit Care. 2014 Nov 19;18(6):634. doi: 10.1186/s13054-014-0634-6. Crit Care. 2014. PMID: 25407832 Free PMC article.
-
Urinary NGAL, IGFBP-7, and TIMP-2: novel biomarkers to predict contrast medium-induced acute kidney injury in children.Ren Fail. 2022 Dec;44(1):1201-1206. doi: 10.1080/0886022X.2022.2075277. Ren Fail. 2022. PMID: 36120960 Free PMC article. Clinical Trial.
-
Comparative accuracy of biomarkers for the prediction of hospital-acquired acute kidney injury: a systematic review and meta-analysis.Crit Care. 2022 Nov 12;26(1):349. doi: 10.1186/s13054-022-04223-6. Crit Care. 2022. PMID: 36371256 Free PMC article.
-
Biomarkers for the diagnosis of sepsis-associated acute kidney injury: systematic review and meta-analysis.Ann Palliat Med. 2021 Apr;10(4):4159-4173. doi: 10.21037/apm-20-1855. Epub 2021 Mar 22. Ann Palliat Med. 2021. PMID: 33832292
Cited by
-
The Predictive Value of Tumor Necrosis Factor Receptor-Associated Factor-Interacting Protein With Forkhead-Associated Domain (TIFA) and Interleukin-1 Beta in Sepsis-Associated Acute Kidney Injury: Bioinformatics Analysis and Experimental Validation.Cureus. 2025 May 18;17(5):e84333. doi: 10.7759/cureus.84333. eCollection 2025 May. Cureus. 2025. PMID: 40385253 Free PMC article.
-
Biological attributes of zinc-dependent endopeptidases in endothelial dysfunction associated with sepsis: a narrative review.Inflamm Res. 2025 Jun 30;74(1):95. doi: 10.1007/s00011-025-02056-x. Inflamm Res. 2025. PMID: 40583077 Review.
References
-
- Zarbock A., Nadim M.K., Pickkers P., Gomez H., Bell S., Joannidis M., et al. Sepsis-associated acute kidney injury: consensus report of the 28th Acute Disease Quality Initiative workgroup. Nat. Rev. Nephrol. 2023;19(6):401–417. - PubMed
-
- Evans L., Rhodes A., Alhazzani W., Antonelli M., Coopersmith C.M., French C., et al. Surviving sepsis campaign: international guidelines for management of sepsis and septic shock 2021. Crit. Care Med. 2021;49(11):e1063–e1143. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous