Mortality Patterns in Pediatric Pulmonary Vein Stenosis: Insights Into Right Ventricular Systolic Pressure Associations
- PMID: 39818963
- PMCID: PMC12054485
- DOI: 10.1161/JAHA.124.037908
Mortality Patterns in Pediatric Pulmonary Vein Stenosis: Insights Into Right Ventricular Systolic Pressure Associations
Erratum in
-
Correction to: Mortality Patterns in Pediatric Pulmonary Vein Stenosis: Insights Into Right Ventricular Systolic Pressure Associations.J Am Heart Assoc. 2025 Mar 18;14(6):e035037. doi: 10.1161/JAHA.124.035037. Epub 2025 Mar 13. J Am Heart Assoc. 2025. PMID: 40079358 Free PMC article.
Abstract
Background: Pulmonary vein stenosis in children is associated with a poor prognosis. However, the cause and risk factors for mortality remain uncertain.
Methods: This retrospective, single-center study identified children with primary and secondary pulmonary vein stenosis through a cardiac catheterization database. Kaplan-Meier analysis, log-rank tests, and Cox regression analysis were performed to assess outcome and identify significant predictors of mortality.
Results: Among 56 children with pulmonary vein stenosis (33 male children, 59%), 20 (36%) died at a median age of 10 months (interquartile range, 4-24 months). All patients underwent cardiac catheterization, with 45 (80%) undergoing at least 1 interventional procedure. Causes of death included multiorgan failure (35%), progressive respiratory failure (20%), and sudden cardiac death (15%). Prematurity, chronic lung disease, a genetic syndrome, or the number of affected pulmonary veins did not significantly correlate with mortality. However, right ventricular (RV) systolic pressure greater than half systemic pressure was associated with mortality (hazard ratio [HR], 5.5 [95% CI, 2.2-14.1]; P<0.001). The final predictive model for mortality included RV systolic pressure greater than half systemic pressure (HR, 4.0 [95% CI, 1.6-10.4]; P=0.004), moderately or severely diminished RV systolic function (HR, 3.6 [95% CI, 1.1-11.5]; P=0.032), and the presence of congenital heart disease (HR, 2.4 [95% CI, 0.9-6.7]; P=0.084).
Conclusions: This report is the first to indicate that RV systolic pressure and RV dysfunction are significant independent predictors of mortality in children with pulmonary vein stenosis. A greater understanding of mortality in this population is necessary, particularly in those with RV systolic pressure less than half systemic.
Keywords: cardiac catheterization; pulmonary vein stenosis; right ventricular systolic pressure.
Conflict of interest statement
None.
Figures

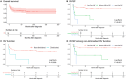
Similar articles
-
Correction to: Mortality Patterns in Pediatric Pulmonary Vein Stenosis: Insights Into Right Ventricular Systolic Pressure Associations.J Am Heart Assoc. 2025 Mar 18;14(6):e035037. doi: 10.1161/JAHA.124.035037. Epub 2025 Mar 13. J Am Heart Assoc. 2025. PMID: 40079358 Free PMC article.
-
Pulmonary Vein Stenosis: Outcomes in Children With Congenital Heart Disease and Prematurity.Semin Thorac Cardiovasc Surg. 2019 Summer;31(2):266-273. doi: 10.1053/j.semtcvs.2018.09.027. Epub 2018 Sep 29. Semin Thorac Cardiovasc Surg. 2019. PMID: 30278272 Free PMC article.
-
Adverse ventricular-ventricular interactions in right ventricular pressure load: Insights from pediatric pulmonary hypertension versus pulmonary stenosis.Physiol Rep. 2016 Jun;4(11):e12833. doi: 10.14814/phy2.12833. Physiol Rep. 2016. PMID: 27302992 Free PMC article.
-
Correlation of Transthoracic Echocardiographic Estimates of Right Ventricular Pressure with Right Ventricular Pressure Measurements on Cardiac Catheterization in Children with Pulmonary Hypertension.J Cardiothorac Vasc Anesth. 2024 Dec;38(12):3101-3108. doi: 10.1053/j.jvca.2024.09.016. Epub 2024 Sep 19. J Cardiothorac Vasc Anesth. 2024. PMID: 39393986
-
Intraluminal Pulmonary Vein Stenosis in Children: A "New" Lesion.Anesth Analg. 2019 Jul;129(1):27-40. doi: 10.1213/ANE.0000000000003924. Anesth Analg. 2019. PMID: 30451723 Review.
Cited by
-
Incidence and Risk Factors of Pulmonary Vein Stenosis After Orthotopic Heart Transplantation in Pediatric Patients.Pediatr Cardiol. 2025 Mar 8. doi: 10.1007/s00246-025-03828-2. Online ahead of print. Pediatr Cardiol. 2025. PMID: 40056188
-
Ten-Year Experience with Pediatric Pulmonary Vein Interventions: Adverse Events and Institutional Strategies for Safety.Pediatr Cardiol. 2025 Jul 20. doi: 10.1007/s00246-025-03955-w. Online ahead of print. Pediatr Cardiol. 2025. PMID: 40684406
References
-
- Mahgoub L, Kaddoura T, Kameny AR, Lopez Ortego P, Vanderlaan RD, Kakadekar A, Dicke F, Rebeyka I, Calderone CA, Redington A, et al. Pulmonary vein stenosis of ex‐premature infants with pulmonary hypertension and bronchopulmonary dysplasia, epidemiology, and survival from a multicenter cohort. Pediatr Pulmonol. 2017;52:1063–1070. doi: 10.1002/ppul.23679 - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources

