Intra-arterial lidocaine administration of lidocaine in middle meningeal artery for short-term treatment of subarachnoid hemorrhage-related headaches
- PMID: 39819076
- PMCID: PMC11748390
- DOI: 10.1177/15910199241307049
Intra-arterial lidocaine administration of lidocaine in middle meningeal artery for short-term treatment of subarachnoid hemorrhage-related headaches
Abstract
Background and purpose: We report short- and intermediate-term effects on headaches with intra-arterial injection of lidocaine in the middle meningeal artery in patients with severe headaches associated with subarachnoid hemorrhage.
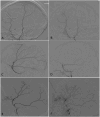
Methods: We treated seven patients with intra-arterial lidocaine in doses up to 50 mg in each middle meningeal artery via a microcatheter bilaterally (except in one patient). We recorded the maximum intensity of headache (graded by 11-point numeric rating scale) prior to procedure and every day for the next 10 days or discharge, whichever came first. We identified changes in the middle meningeal artery pre- and post-intra-arterial lidocaine administration and quantified from Grade 0 (no change) to Grade 5 (severe narrowing or near occlusion of anterior and posterior dural branches or proximal middle meningeal artery that precludes adequate imaging of distal branches).
Results: We observed improvement in severity of headaches of headache in all seven subarachnoid hemorrhage patients. The resolution of headache was immediate and complete in four patients, unilateral immediate resolution in one patient, and delayed complete resolution in patient. Two patients met the definition of severe headache (defined as 2 or more days with maximum pain scores of 8 or greater or need for 3 or more different analgesics for 2 or more days) post-lidocaine treatment. One of these patients had are lapse in headache with the severity matching pretreatment severity and required a second treatment. On analysis of angiographic data, there was consistent narrowing of middle meningeal arteries after administration of intra-arterial lidocaine and was graded as 5 in 2 arteries, 4 in 10 arteries, and 3 in 2 arteries.
Conclusions: We found that intra-arterial injection of lidocaine can result in consistent amelioration of headache in patients with subarachnoid hemorrhage. The therapeutic benefit may be related to vasoconstriction (reversal of vasodilation) in the middle meningeal arteries after administration of lidocaine.
Keywords: Intra-arterial administration; intractable headache; lidocaine; middle meningeal artery; subarachnoid hemorrhage.
Conflict of interest statement
Declaration of conflicting interestsDr. Qureshi is confounder of Qureshi Medical LLC, QureVasc LLC, and DyQure LLC. Dr. Qureshi also holds a patent on intra-arterial sustained release device in the middle meningeal artery.
Figures
Similar articles
-
Blazing the trail! Commentary on "Intra-arterial lidocaine administration in middle meningeal artery for short-term treatment of subarachoid hemorrhage-related headaches" by Qureshi et al.Interv Neuroradiol. 2025 Feb 25:15910199251324039. doi: 10.1177/15910199251324039. Online ahead of print. Interv Neuroradiol. 2025. PMID: 40007259 Free PMC article.
-
Intra-arterial injection of lidocaine into middle meningeal artery to treat intractable headaches and severe migraine.J Neuroimaging. 2021 Nov;31(6):1126-1134. doi: 10.1111/jon.12918. Epub 2021 Aug 13. J Neuroimaging. 2021. PMID: 34388298
-
Effect of intra-arterial injection of lidocaine and methyl-prednisolone into middle meningeal artery on intractable headaches.J Vasc Interv Neurol. 2014 Dec;7(5):69-72. J Vasc Interv Neurol. 2014. PMID: 25566345 Free PMC article.
-
Intra-arterial lidocaine therapy via the middle meningeal artery for migraine headache: Theory, current practice and future directions.Interv Neuroradiol. 2023 Aug 13:15910199231195470. doi: 10.1177/15910199231195470. Online ahead of print. Interv Neuroradiol. 2023. PMID: 37574789 Review.
-
Headache persisting after aneurysmal subarachnoid hemorrhage: A narrative review of pathophysiology and therapeutic strategies.Headache. 2022 Oct;62(9):1120-1132. doi: 10.1111/head.14394. Epub 2022 Sep 16. Headache. 2022. PMID: 36112096 Review.
Cited by
-
Blazing the trail! Commentary on "Intra-arterial lidocaine administration in middle meningeal artery for short-term treatment of subarachoid hemorrhage-related headaches" by Qureshi et al.Interv Neuroradiol. 2025 Feb 25:15910199251324039. doi: 10.1177/15910199251324039. Online ahead of print. Interv Neuroradiol. 2025. PMID: 40007259 Free PMC article.
References
-
- Gorelick PB, Hier DB, Caplan LR, et al. Headache in acute cerebrovascular disease. Neurology 1986; 36: 1445–1450. - PubMed
-
- Dorhout Mees SM, Bertens D, van der Worp HB, et al. Magnesium and headache after aneurysmal subarachnoid haemorrhage. J Neurol Neurosurg Psychiatry 2010; 81: 490–493. 20091013. - PubMed
-
- Swope R, Glover K, Gokun Y, et al. Evaluation of headache severity after aneurysmal subarachnoid hemorrhage. Interdisciplinary Neurosurgery 2014; 1: 119–122.
-
- Glisic EK, Gardiner L, Josti L, et al. Inadequacy of headache management after subarachnoid hemorrhage. Am J Crit Care 2016; 25: 136–143. - PubMed
-
- Viswanathan V, Lucke-Wold B, Jones C, et al. Change in opioid and analgesic use for headaches after aneurysmal subarachnoid hemorrhage over time. Neurochirurgie 2021; 67: 427–432. 20210323. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

