This is a preprint.
Estimating the burden of RSV- and influenza-associated hospitalizations, ICU admissions, and deaths across age and socioeconomic groups in New York State, 2005-2019
- PMID: 39830274
- PMCID: PMC11741487
- DOI: 10.1101/2025.01.10.24319265
Estimating the burden of RSV- and influenza-associated hospitalizations, ICU admissions, and deaths across age and socioeconomic groups in New York State, 2005-2019
Abstract
Background: Multiple prophylactic products are now available to protect against respiratory syncytial virus (RSV) in different age groups. Assessing the pre-intervention burden of RSV infections across various severity levels and risk groups is crucial, as it provides a baseline for evaluating the impact of these products.
Methods: We obtained monthly time series data on hospitalizations, intensive care unit (ICU) admissions, and deaths by age group, ZIP code, and cause for New York state from 2005 to 2019. Socioeconomic status (SES) of the ZIP codes was classified using supervised principal component analysis (PCA). We estimated the incidence of hospitalizations, ICU admissions, and deaths attributable to RSV and to influenza using hierarchical Bayesian regression models. Additionally, we assessed severity, defined by ICU admission and mortality risks, as well as recording fraction (i.e., percent of estimated virus-associated hospitalizations recorded as being due to the specific virus), stratified by age, SES, and over time.
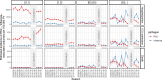
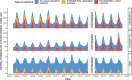
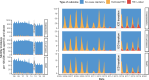
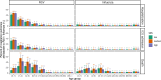
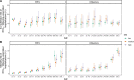
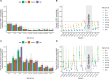
Results: The estimated annual incidence of RSV-associated hospitalizations and ICU admissions were highest in infants under 1 in the low SES group (2,240 [95% credible interval (CrI): 2,200-2,290] hospitalizations and 330 [95% CrI: 320-350] ICU admissions per 100,000 person-years). The incidence of RSV-associated deaths was highest among adults ≥85 years old (61 [95% CrI: 49-74] per 100,000 person-years). In contrast to RSV, the burden of influenza was greatest in age groups ≥65 years. The risk of ICU admission varied by patients' age and SES, and the mortality risk increased dramatically with age for both pathogens (RSV: 11.9% [95% CrI: 9.6-14.3%], influenza: 14.4% [95% CrI: 13.1-15.6%] among ≥85 year age group). Incidence varied by epidemic year and season, and we observed an increasing recording fraction of RSV among all age groups over the study period.
Conclusions: RSV and influenza contribute significantly to the burden of hospitalizations, ICU admissions, and deaths, particularly among infants and older adults. Although the recording fraction of RSV increased over the study period, it remains lower, particularly for adults. Our findings reveal a disparity in hospitalization burden by SES, particularly among younger age groups.
Conflict of interest statement
Conflicts of interest DMW has been the principal investigator on grants from Pfizer and Merck to Yale University for work unrelated to this manuscript and has received consulting fees from Pfizer, Merck, and GSK for work unrelated to this manuscript. JLW has received consulting fees from Pfizer for work unrelated to this project.
Figures

Similar articles
-
Estimated incidence of respiratory hospitalizations attributable to RSV infections across age and socioeconomic groups.Pneumonia (Nathan). 2022 Oct 25;14(1):6. doi: 10.1186/s41479-022-00098-x. Pneumonia (Nathan). 2022. PMID: 36280891 Free PMC article.
-
Age-Specific Estimates of Respiratory Syncytial Virus-Associated Hospitalizations in 6 European Countries: A Time Series Analysis.J Infect Dis. 2022 Aug 12;226(Suppl 1):S29-S37. doi: 10.1093/infdis/jiac150. J Infect Dis. 2022. PMID: 35748871
-
Economic burden and secondary complications of influenza-related hospitalization among adults in the US: a retrospective cohort study.J Med Econ. 2024 Jan-Dec;27(1):324-336. doi: 10.1080/13696998.2024.2314429. Epub 2024 Feb 22. J Med Econ. 2024. PMID: 38343288
-
Global disease burden of and risk factors for acute lower respiratory infections caused by respiratory syncytial virus in preterm infants and young children in 2019: a systematic review and meta-analysis of aggregated and individual participant data.Lancet. 2024 Mar 30;403(10433):1241-1253. doi: 10.1016/S0140-6736(24)00138-7. Epub 2024 Feb 14. Lancet. 2024. PMID: 38367641
-
Global, regional, and national incidence and mortality burden of non-COVID-19 lower respiratory infections and aetiologies, 1990-2021: a systematic analysis from the Global Burden of Disease Study 2021.Lancet Infect Dis. 2024 Sep;24(9):974-1002. doi: 10.1016/S1473-3099(24)00176-2. Epub 2024 Apr 15. Lancet Infect Dis. 2024. PMID: 38636536 Free PMC article.
References
-
- Li Y, Wang X, Blau DM, Caballero MT, Feikin DR, Gill CJ, et al. Global, regional, and national disease burden estimates of acute lower respiratory infections due to respiratory syncytial virus in children younger than 5 years in 2019: a systematic analysis. Lancet. 2022;399: 2047–2064. - PMC - PubMed
-
- Thompson WW, Shay DK, Weintraub E, Brammer L, Cox N, Anderson LJ, et al. Mortality associated with influenza and respiratory syncytial virus in the United States. JAMA. 2003;289: 179–186. - PubMed
-
- Fact sheets, Influenza (seasonal). 3 Oct 2023. [cited 12 Nov 2024]. Available: https://www.who.int/news-room/fact-sheets/detail/influenza-(seasonal)
-
- Simoes EA. Environmental and demographic risk factors for respiratory syncytial virus lower respiratory tract disease. J Pediatr. 2003;143: S118–26. - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
