Evaluating the Adequacy of Central Line-Associated Bloodstream Infection As a Quality Measure: A Cross-Sectional Analysis at a Single Tertiary Care Center
- PMID: 39830835
- PMCID: PMC11741216
- DOI: 10.1097/CCE.0000000000001205
Evaluating the Adequacy of Central Line-Associated Bloodstream Infection As a Quality Measure: A Cross-Sectional Analysis at a Single Tertiary Care Center
Abstract
Importance: The current definition of central line-associated bloodstream infection (CLABSI) may overestimate the true incidence of CLABSI as it is often unclear whether the bloodstream infection (BSI) is secondary to the central line or due to another infectious source.
Objectives: We aimed to assess the prevalence and outcomes of central CLABSI at our institution, to identify opportunities for improvement, appropriately direct efforts for infection reduction, and identify gaps in the CLABSI definition and its application as a quality measure.
Design setting and participants: Retrospective cross-sectional study of patients identified to have a CLABSI in the period 2018-2022 cared for at the value-based purchasing (VBP) units of a 1200-bed tertiary care hospital located in Cleveland, OH. Each CLABSI episode was assessed for relationship with central venous catheter (CVC), suspected secondary source of BSI, mortality associated with the CLABSI hospital encounter, and availability of infectious disease physician or primary physician documentation of infectious source.
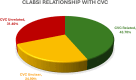
Main outcomes and measures: CLABSI episodes were classified as CVC related, CVC unrelated, and CVC relationship unclear. Mortality during the same encounter as the CLABSI event was assessed as an outcome measure. Descriptive statistics were performed.
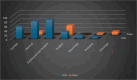
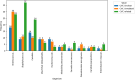
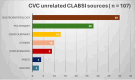
Results: A total of 340 CLABSI episodes occurred in adult patients in VBP units. Majority of the CLABSI, 77.5% (266), occurred in the ICU. Of the CLABSI analyzed, 31.5% (107) were classified as unrelated to the CVC; 25.0% (85) had an unclear source; 43% (148) were classified as CVC related. For CVC-related cases, Staphylococcus and Candida were the predominant organisms. For the CVC unrelated and unclear groups Enterococcus was most prevalent. The mortality rate was lowest among patients classified with a CVC-related BSI. The positive predictive value (PPV) of the Centers for Disease Control and Prevention CLABSI definition to predict a true CVC-related infection was found to be 58.0%.
Conclusions and relevance: The definition of CLABSI as a surrogate for catheter-related BSI is inadequate, with a PPV of 58.0% (43.1-67.6%). Efforts should be redirected toward revising the CLABSI definition and possibly reevaluating its criteria. Resources should be assigned to further investigate and systematically prevent BSIs from secondary sources while adhering to existing CLABSI prevention bundles.
Keywords: central venous catheterization; critical care; healthcare quality; healthcare-associated infection; nosocomial infection.
Copyright © 2025 The Authors. Published by Wolters Kluwer Health, Inc. on behalf of the Society of Critical Care Medicine.
Conflict of interest statement
The authors have disclosed that they do not have any potential conflicts of interest.
Figures
Similar articles
-
[Prevention and control status of central line-associated bloodstream infection in intensive care unit in Shandong province: a cross-sectional survey analysis].Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2024 Dec;36(12):1315-1320. doi: 10.3760/cma.j.cn121430-20240430-00397. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2024. PMID: 39780679 Chinese.
-
Comparison of Rates of Central Line-Associated Bloodstream Infections in Patients With 1 vs 2 Central Venous Catheters.JAMA Netw Open. 2020 Mar 2;3(3):e200396. doi: 10.1001/jamanetworkopen.2020.0396. JAMA Netw Open. 2020. PMID: 32129868 Free PMC article.
-
Emergency Department Central Line-associated Bloodstream Infections (CLABSI) Incidence in the Era of Prevention Practices.Acad Emerg Med. 2015 Sep;22(9):1048-55. doi: 10.1111/acem.12744. Acad Emerg Med. 2015. PMID: 26336036 Free PMC article.
-
The effect of the multimodal intervention including an automatic notification of catheter days on reducing central line-related bloodstream infection: a retrospective, observational, quasi-experimental study.BMC Infect Dis. 2022 Jul 8;22(1):604. doi: 10.1186/s12879-022-07588-9. BMC Infect Dis. 2022. PMID: 35804323 Free PMC article. Review.
-
Nurses' Knowledge and Behavior in Hospitals Regarding the Prevention of Central Line-Associated Bloodstream Infections: A Systematic Review.SAGE Open Nurs. 2025 May 30;11:23779608251347119. doi: 10.1177/23779608251347119. eCollection 2025 Jan-Dec. SAGE Open Nurs. 2025. PMID: 40453572 Free PMC article. Review.
References
-
- National Healthcare Safety Network: Bloodstream Infection Event (Central Line-Associated Bloodstream Infection and Non-Central Line Associated Bloodstream Infection). 2024. Available at: https://www.cdc.gov/nhsn/psc/bsi/index.html. Accessed June 1, 2024
-
- The Joint Commission: Preventing Central Line–Associated Bloodstream Infections: A Global Challenge, a Global Perspective. 2012. Available at: https://psnet.ahrq.gov/issue/preventing-central-line-associated-bloodstr.... Accessed June 12, 2024
-
- Agency for Healthcare Research and Quality: Toolkit for Reducing Central Line-Associated Blood Stream Infections. 2023. Available at: https://www.ahrq.gov/hai/clabsi-tools/index.html. Accessed June 12, 2024
-
- Sopirala MM, Estelle CD, Houston L: Central line-associated bloodstream infection misclassifications-rethinking the Centers for Disease Control and Prevention’s central line-associated bloodstream infection definition and its implications. Crit Care Med 2024; 52:357–361 - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Research Materials

