Tetracycline and chloramphenicol exposure induce decreased susceptibility to tigecycline and genetic alterations in AcrAB-TolC efflux pump regulators in Escherichia coli and Klebsiella pneumoniae
- PMID: 39841693
- PMCID: PMC11753663
- DOI: 10.1371/journal.pone.0315847
Tetracycline and chloramphenicol exposure induce decreased susceptibility to tigecycline and genetic alterations in AcrAB-TolC efflux pump regulators in Escherichia coli and Klebsiella pneumoniae
Abstract
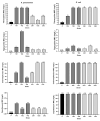
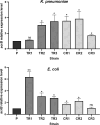
Tigecycline (Tgc), a third-generation tetracycline is found as the last line of defense against multi-drug resistant bacteria. Recent increased rate of resistance to tgc, a human-restricted agent among animal bacteria poses a significant global health challenge. Overuse of first generation tetracyclines (Tet) and phenicols in animals have been suggested to be associated with Tgc resistance development. In the current study we aimed to determine the effect of tetracycline (Tet) and chloramphenicol (Chl) overexposure on Tgc susceptibility. A Tet and Chl-susceptible isolate of K. pneumoniae and E. coli were exposed to successively increasing concentrations of tetracycline and chloramphenicol separately until a ≥4 times increase in Tet and Chl MICs was observed. Susceptibility changes to several antimicrobial agents were tested using disk diffusion and broth dilution methods. The genetic alterations of genes coding for major AcrAB regulators including acrR (repressor of acrAB), ramR (repressor of ramA), soxR (repressor of soxS) in K. pneumoniae and lon (proteolytic degradation of MarA), marR (repressor of marA), acrR and soxR in E. coli were investigated. The expression level of acrB was measured using reverse transcription-quantitative polymerase chain reaction (RT-qPCR) method. The excessive exposure (15 to 40 selection cycles) of studied bacteria to both antibiotics significantly decreased susceptibility of Tet-resistant (R) and Chl-R variants of E. coli (n = 6) and K. pneumoniae (n = 6) to several groups of antibiotics including tigecycline (4-16 and 8-64 times respectively) and quinolones. About 58% of variants (n = 7) carried genetic alterations in AcrAB regulators including ramR (frameshift mutations/locus deletion), MarR (L33R, A70T, G15S amino acid substitutions) and Lon (L630F change, frameshift mutation) which were associated with acrB upregulation. Our study demonstrated the capacity of chloramphenicol and tetracycline exposure for selection of mutants which revealed tigecycline resistance/decreased susceptibility mostly mediated by active efflux mechanism. Unaltered acrB expression level in some strains indicates possible contribution of other efflux pumps or non-efflux-based mechanisms in the development of multiple- antibiotic resistance phenotype.
Copyright: © 2025 Nasralddin et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Similar articles
-
First emergence of acrAB and oqxAB mediated tigecycline resistance in clinical isolates of Klebsiella pneumoniae pre-dating the use of tigecycline in a Chinese hospital.PLoS One. 2014 Dec 12;9(12):e115185. doi: 10.1371/journal.pone.0115185. eCollection 2014. PLoS One. 2014. PMID: 25503276 Free PMC article.
-
AcrAB-TolC efflux pump overexpression and tet(A) gene mutation increase tigecycline resistance in Klebsiella pneumoniae.World J Microbiol Biotechnol. 2024 Jun 6;40(8):233. doi: 10.1007/s11274-024-04039-2. World J Microbiol Biotechnol. 2024. PMID: 38842631
-
Tigecycline susceptibility in Klebsiella pneumoniae and Escherichia coli causing neonatal septicaemia (2007-10) and role of an efflux pump in tigecycline non-susceptibility.J Antimicrob Chemother. 2013 May;68(5):1036-42. doi: 10.1093/jac/dks535. Epub 2013 Jan 18. J Antimicrob Chemother. 2013. PMID: 23335112
-
Regulation of the AcrAB-TolC efflux pump in Enterobacteriaceae.Res Microbiol. 2018 Sep-Oct;169(7-8):425-431. doi: 10.1016/j.resmic.2017.10.005. Epub 2017 Nov 8. Res Microbiol. 2018. PMID: 29128373 Review.
-
Tigecycline.2025 Apr 15. LiverTox: Clinical and Research Information on Drug-Induced Liver Injury [Internet]. Bethesda (MD): National Institute of Diabetes and Digestive and Kidney Diseases; 2012–. 2025 Apr 15. LiverTox: Clinical and Research Information on Drug-Induced Liver Injury [Internet]. Bethesda (MD): National Institute of Diabetes and Digestive and Kidney Diseases; 2012–. PMID: 31643224 Free Books & Documents. Review.
Cited by
-
Selected Polyphenols of Polish Poplar Propolis as a Key Component Shaping Its Antibacterial Properties-In Vitro and In Silico Approaches.Molecules. 2025 May 3;30(9):2036. doi: 10.3390/molecules30092036. Molecules. 2025. PMID: 40363841 Free PMC article.
-
Emergence of transferable tigecycline and eravacycline resistance gene tet(X4) in Escherichia coli isolates from Iran.Sci Rep. 2025 May 13;15(1):16581. doi: 10.1038/s41598-025-98206-6. Sci Rep. 2025. PMID: 40360684 Free PMC article.
References
-
- Renteria M, Biedenbach D, Bouchillon S, Hoban D, Raghubir N, Sajben P. In vitro activity of tigecycline and comparators against carbapenem-resistant Enterobacteriaceae in Africa–Middle East countries: TEST 2007–2012. Journal of Global Antimicrobial Resistance. 2014;2(3):179–82. doi: 10.1016/j.jgar.2014.03.002 - DOI - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases

