Finite Element Analysis of Functionally Loaded Subperiosteal Implants Evaluated on a Realistic Model Reproducing Severe Atrophic Jaws
- PMID: 39846694
- PMCID: PMC11755603
- DOI: 10.3390/mps8010008
Finite Element Analysis of Functionally Loaded Subperiosteal Implants Evaluated on a Realistic Model Reproducing Severe Atrophic Jaws
Abstract
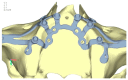
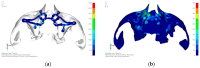
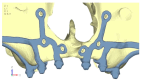
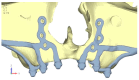
Implant-supported prosthetic rehabilitation for patients with severely atrophic jaws is challenging due to complex anatomical considerations and the limitations of conventional augmentation techniques. This study explores the potential of subperiosteal (juxta-osseous) implants as an alternative solution, using finite element analysis (FEA) to evaluate mechanical performance. Realistic jaw models, developed from radiographic data, are utilized to simulate various implant configurations and load scenarios. Results indicate that different screw placements, implant designs, and structural modifications can significantly influence stress distribution and biomechanical behavior. Upper and lower jaw models were assessed under multiple load conditions to determine optimal configurations. Findings suggest that strategic adjustments, such as adding posterior screws or altering implant connections, can enhance load distribution and reduce stress concentration, particularly in critical areas. Tensile loads in critical bone areas near cortical fixing screws exceeded 50 MPa under anterior loading, while configurations with larger load distributions reduced stress on both implant and bone. The study provides evidence-based insights into optimizing subperiosteal implant design to improve stability, longevity, and patient outcomes.
Keywords: finite element analysis (FEA); juxta-osseous implants; severe jaw atrophy.
Conflict of interest statement
The authors declare no conflicts of interests.
Figures
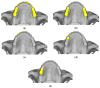
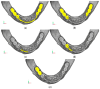

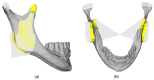



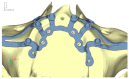












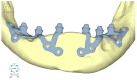

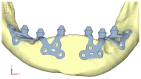

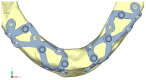
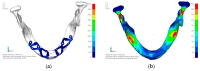

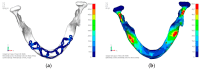
References
-
- Alotaibi F.F., Rocchietta I., Buti J., D’Aiuto F. Comparative evidence of different surgical techniques for the management of vertical alveolar ridge defects in terms of complications and efficacy: A systematic review and network meta-analysis. J. Clin. Periodontol. 2023;50:1487–1519. doi: 10.1111/jcpe.13850. - DOI - PubMed
-
- Felice P., Barausse C., Barone A., Zucchelli G., Piattelli M., Pistilli R., Ippolito D.R., Simion M. Interpositional augmentation technique in the treatment of posterior mandibular atrophies: A retrospective study comparing 129 autogenous and heterologous bone blocks with 2 to 7 years follow-up. Int. J. Periodontics Restor. Dent. 2017;37:469–480. doi: 10.11607/prd.2999. - DOI - PubMed
-
- Esposito M., Cannizzaro G., Barausse C., Cosci F., Soardi E., Felice P. Cosci versus Summers technique for crestal sinus lift: 3-year results from a randomized controlled trial. Eur. J. Oral Implantol. 2014;7:129–137. - PubMed
LinkOut - more resources
Full Text Sources

