Margin matters: analyzing the impact of circumferential margin involvement on survival and recurrence after incomplete total mesorectal excision for rectal cancer
- PMID: 39847185
- PMCID: PMC11757853
- DOI: 10.1007/s10151-024-03098-9
Margin matters: analyzing the impact of circumferential margin involvement on survival and recurrence after incomplete total mesorectal excision for rectal cancer
Abstract
Background: Incomplete mesorectal excision during rectal cancer surgery often leads to positive circumferential margins, with uncertain prognostic impacts. This study examines whether negative margins can mitigate the poorer prognosis typically associated with incomplete total mesorectal excision (TME) in rectal cancer surgery, thus potentially challenging the prevailing emphasis on complete mesorectal excision.
Patients and methods: A retrospective analysis was conducted on patients who underwent proctectomy for rectal adenocarcinoma with incomplete TME at a single center from 2010 to 2022. Patients were stratified by margin status as determined by pathologic analysis into three groups: involved, not involved with closest margin distance ≤ 2 mm, and not involved with closest margin distance > 2 mm. Outcomes included recurrence and survival. Effects of neoadjuvant therapy protocols on margin status were also assessed.
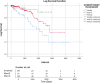
Results: From 2010 to 2022, 7941 patients underwent proctectomy for rectal cancer, with 236 (3%) having incomplete TME. The median age of these patients was 64 years, and 63% were male. Overall, margin involvement was observed in 54 (23%) patients. The median tumor size was 3.05 cm (interquartile range (IQR): 2-6) for the whole group. Involved margins (23.2%) had reduced overall survival (60.5 months versus 87.3 months, p < 0.001), increased local recurrence (20.4% versus 9.4%, p = 0.024), and lower disease-free survival (45.2 versus 58.9 months, p = 0.006) versus uninvolved margins. Margin involvement was prognostic for decreased survival even after adjusting for confounders (p < 0.05). Among uninvolved margins, distance (> 2 mm versus ≤ 2 mm) did not affect outcomes. Total neoadjuvant therapy (versus standard chemoradiation) was associated with lower involved margins (p = 0.007).
Conclusions: Positive margins retain negative prognostic impact with incomplete TME. Optimization of surgical resection remains vital. Total neoadjuvant therapy was associated with a lower rate of margin involvement.
Keywords: Incomplete TME; Margin status; Mesorectal excision; Neoadjuvant therapy; Rectal adenocarcinoma.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Conflicts of interest: The authors have no conflicts to disclose.
Figures


Similar articles
-
Association of Surgical Approaches and Outcomes in Total Mesorectal Excision and Margin Status for Rectal Cancer.J Surg Res. 2024 Aug;300:494-502. doi: 10.1016/j.jss.2024.05.032. Epub 2024 Jun 14. J Surg Res. 2024. PMID: 38875948
-
Predictors of Positive Circumferential Resection Margin in Rectal Cancer: A Current Audit of the National Cancer Database.Dis Colon Rectum. 2021 Sep 1;64(9):1096-1105. doi: 10.1097/DCR.0000000000002115. Dis Colon Rectum. 2021. PMID: 33951688
-
Association of Transanal Total Mesorectal Excision With Local Recurrence of Rectal Cancer.JAMA Netw Open. 2021 Feb 1;4(2):e2036330. doi: 10.1001/jamanetworkopen.2020.36330. JAMA Netw Open. 2021. PMID: 33533932 Free PMC article.
-
Statistical, Clinical, Methodological Evaluation of Local Recurrence Following Transanal Total Mesorectal Excision for Rectal Cancer: A Systematic Review.Dis Colon Rectum. 2021 Jul 1;64(7):899-914. doi: 10.1097/DCR.0000000000002110. Dis Colon Rectum. 2021. PMID: 33938532
-
Neoadjuvant radiotherapy for rectal cancer management.World J Gastroenterol. 2019 Sep 7;25(33):4850-4869. doi: 10.3748/wjg.v25.i33.4850. World J Gastroenterol. 2019. PMID: 31543678 Free PMC article. Review.
References
-
- Siegel RL, Wagle NS, Cercek A, Smith RA, Jemal A (2023) Colorectal cancer statistics, 2023. CA Cancer J Clin 73(3):233–254. 10.3322/caac.21772. (Epub 2023 Mar 1. PMID: 36856579) - PubMed
-
- American Cancer Society (2023) Colorectal cancer facts & figures 2023–2025. American Cancer Society, Atlanta
-
- Ferko A, Orhalmi J, Dusek T, Chobola M, Hovorkova E, Nikolov DH (2014) Higher risk of incomplete mesorectal excision and positive circumferential margin in low rectal cancer regardless of surgical technique. Wideochir Inne Tech Maloinwazyjne 9(4):569–577. 10.5114/wiitm.2014.45733. (Epub 2014 Oct 7. PMID: 25561995; PMCID: PMC4280422) - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources

