Child mortality in England after national lockdowns for COVID-19: An analysis of childhood deaths, 2019-2023
- PMID: 39847573
- PMCID: PMC11756792
- DOI: 10.1371/journal.pmed.1004417
Child mortality in England after national lockdowns for COVID-19: An analysis of childhood deaths, 2019-2023
Abstract
Background: During the COVID-19 pandemic children and young people (CYP) mortality in England reduced to the lowest on record, but it is unclear if the mechanisms which facilitated a reduction in mortality had a longer lasting impact, and what impact the pandemic, and its social restrictions, have had on deaths with longer latencies (e.g., malignancies). The aim of this analysis was to quantify the relative rate, and causes, of childhood deaths in England, before, during, and after national lockdowns for COVID-19 and its social changes.
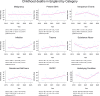
Methods and findings: Deaths of all children (occurring before their 18th birthday) occurring from April 2019 until March 2023 in England were identified. Data were collated by the National Child Mortality Database. Study population size and the underlying population profile was derived from 2021 Office of National Statistics census data Mortality for each analysis year was calculated per 1,000,000 person years. Poisson regression was used to test for an overall trend across the time period and tested if trends differed between April 2019 to March 2021 (Period 1)) and April 2021 to March 2023 (Period 2: after lockdown restrictions). This was then repeated for each category of death and demographic group. Twelve thousand eight hundred twenty-eight deaths were included in the analysis. Around 59.4% of deaths occurred under 1 year of age, 57.0% were male, and 63.9% were of white ethnicity. Mortality rate (per 1,000,000 CYP per year) dropped from 274.2 (95% CI 264.8-283.8) in 2019-2020, to 242.2 (95% CI 233.4-251.2) in 2020-2021, increasing to 296.1 (95% CI 286.3-306.1) in 2022-2023. Overall, death rate reduced across Period 1 (Incidence rate ratio (IRR) 0.96 (95% CI 0.92-0.99)) and then increased across Period 2 (IRR 1.12 (95% CI 1.08-1.16)), and this pattern was also seen for death by Infection and Underlying Disease. In contrast, rate of death after Intrapartum events increased across the first period, followed by a decrease in rate in the second (Period 1 IRR 1.15 (95% CI 1.00-1.34)) versus Period 2 (IRR 0.78 (95% CI 0.68-0.91), pdifference = 0.004). Rates of death from preterm birth, trauma and sudden unexpected deaths in infancy and childhood (SUDIC), increased across the entire 4-year-study period (preterm birth, IRR 1.03 (95% CI 1.00-1.07); trauma IRR 1.12 (95% CI 1.06-1.20); SUDIC IRR 1.09 (95% CI 1.04-1.13)), and there was no change in the rate of death from Malignancy (IRR 1.01 (95% CI 0.95-1.06)). Repeating the analysis, split by child characteristics, suggested that mortality initially dropped and subsequently rose for children between 1 and 4 years old (Period 1 RR 0.85 (95% CI 0.76-0.94) versus Period 2 IRR 1.31 (95% CI 1.19-1.43), pdifference < 0.001. For Asian, black and Other ethnic groups, we observed increased rates of deaths in the period 2021-2023, and a significant change in trajectory of death rates between Periods 1 and 2 (Asian (Period 1 IRR 0.93 (95% CI 0.86-1.01) versus Period 2 IRR 1.28 (95% CI 1.18-1.38), pdifference < 0.001); black (Period 1 IRR 0.97 (95% CI 0.85-1.10) versus Period 2 IRR 1.27 (95% CI 1.14-1.42), pdifference = 0.012); Other (Period 1 IRR 0.84 (95% CI 0.68-1.04) versus Period 2 IRR 1.45 (95% CI 1.20-1.75), pdifference = 0.003). Similar results were observed in CYP in the most deprived areas (Period 1 IRR 0.95 (95% CI 0.89-1.01) versus Period 2 IRR 1.18 (95% CI 1.12-1.25), pdifference < 0.001). There was no change in the trajectory of death rates for children from white (p = 0.601) or mixed (p = 0.823) ethnic backgrounds, or those in the least deprived areas (p = 0.832), between Periods 1 and 2; with evidence of a rise across the whole study period for children from white backgrounds (IRR 1.05 (95% CI 1.03-1.07), p < 0.001) and those in the least deprived areas (IRR 1.06 (95% CI 1.01-1.10), p < 0.001). Limitations include that the population at risk was estimated at a mid-point of the study, and changes may have biased our estimates. In particular, absolute rates should be interpreted with caution. In addition, child death in England is rare, which may further limit interpretation; particularly in the stratified analyses.
Conclusions: In this study, overall child mortality in England after the national lockdowns was higher than before them. We observed different temporal profiles across the different causes of death, with reassuring trends in deaths from Intrapartum deaths after lockdowns were lifted. However, for all other causes of death, rates are either static, or increasing. In addition, the relative rate of dying for children from non-white backgrounds, compared to white children, is now higher than before or during the lockdowns.
Copyright: © 2025 Odd et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures


References
-
- 14.9 Million excess deaths associated with the COVID-19 pandemic in 2020 and 2021. World Health Organisation; 2022 [cited 17/10/2024]. Available from https://www.who.int/news/item/05-05-2022-14.9-million-excess-deaths-were...
-
- Odd D, Stoianova S, Williams T, Thursby-Pelham A, Ladhani S, Oligbu G, et al. Deaths in children and young people in England following SARS-CoV-2 infection during the first two years of the pandemic: a national study using linked mandatory child death reporting data. Research Square. 2023. doi: 10.21203/rs.3.rs-3782971/v1 - DOI
-
- Flaxman S, Whittaker C, Semenova E, Rashid T, Parks RM, Blenkinsop A, et al. Assessment of COVID-19 as the underlying cause of death among children and young people aged 0 to 19 Years in the US. JAMA Netw Open. 2023;6(1):e2253590. Epub 2023 Jan 03. doi: 10.1001/jamanetworkopen.2022.53590 ; PMCID: PMC9887489 - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

