Persistent symptoms and clinical findings in adults with post-acute sequelae of COVID-19/post-COVID-19 syndrome in the second year after acute infection: A population-based, nested case-control study
- PMID: 39847575
- PMCID: PMC12005676
- DOI: 10.1371/journal.pmed.1004511
Persistent symptoms and clinical findings in adults with post-acute sequelae of COVID-19/post-COVID-19 syndrome in the second year after acute infection: A population-based, nested case-control study
Abstract
Background: Self-reported health problems following severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection are common and often include relatively non-specific complaints such as fatigue, exertional dyspnoea, concentration or memory disturbance and sleep problems. The long-term prognosis of such post-acute sequelae of COVID-19/post-COVID-19 syndrome (PCS) is unknown, and data finding and correlating organ dysfunction and pathology with self-reported symptoms in patients with non-recovery from PCS is scarce. We wanted to describe clinical characteristics and diagnostic findings among patients with PCS persisting for >1 year and assessed risk factors for PCS persistence versus improvement.
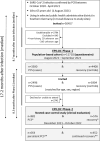
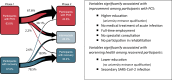
Methods and findings: This nested population-based case-control study included subjects with PCS aged 18-65 years with (n = 982) and age- and sex-matched control subjects without PCS (n = 576) according to an earlier population-based questionnaire study (6-12 months after acute infection, phase 1) consenting to provide follow-up information and to undergo comprehensive outpatient assessment, including neurocognitive, cardiopulmonary exercise, and laboratory testing in four university health centres in southwestern Germany (phase 2, another 8.5 months [median, range 3-14 months] after phase 1). The mean age of the participants was 48 years, and 65% were female. At phase 2, 67.6% of the patients with PCS at phase 1 developed persistent PCS, whereas 78.5% of the recovered participants remained free of health problems related to PCS. Improvement among patients with earlier PCS was associated with mild acute index infection, previous full-time employment, educational status, and no specialist consultation and not attending a rehabilitation programme. The development of new symptoms related to PCS among participants initially recovered was associated with an intercurrent secondary SARS-CoV-2 infection and educational status. Patients with persistent PCS were less frequently never smokers (61.2% versus 75.7%), more often obese (30.2% versus 12.4%) with higher mean values for body mass index (BMI) and body fat, and had lower educational status (university entrance qualification 38.7% versus 61.5%) than participants with continued recovery. Fatigue/exhaustion, neurocognitive disturbance, chest symptoms/breathlessness and anxiety/depression/sleep problems remained the predominant symptom clusters. Exercise intolerance with post-exertional malaise (PEM) for >14 h and symptoms compatible with myalgic encephalomyelitis/chronic fatigue syndrome were reported by 35.6% and 11.6% of participants with persistent PCS patients, respectively. In analyses adjusted for sex-age class combinations, study centre and university entrance qualification, significant differences between participants with persistent PCS versus those with continued recovery were observed for performance in three different neurocognitive tests, scores for perceived stress, subjective cognitive disturbances, dysautonomia, depression and anxiety, sleep quality, fatigue and quality of life. In persistent PCS, handgrip strength (40.2 [95% confidence interval (CI) [39.4, 41.1]] versus 42.5 [95% CI [41.5, 43.6]] kg), maximal oxygen consumption (27.9 [95% CI [27.3, 28.4]] versus 31.0 [95% CI [30.3, 31.6]] ml/min/kg body weight) and ventilatory efficiency (minute ventilation/carbon dioxide production slope, 28.8 [95% CI [28.3, 29.2]] versus 27.1 [95% CI [26.6, 27.7]]) were significantly reduced relative to the control group of participants with continued recovery after adjustment for sex-age class combinations, study centre, education, BMI, smoking status and use of beta blocking agents. There were no differences in measures of systolic and diastolic cardiac function at rest, in the level of N-terminal brain natriuretic peptide blood levels or other laboratory measurements (including complement activity, markers of Epstein-Barr virus [EBV] reactivation, inflammatory and coagulation markers, serum levels of cortisol, adrenocorticotropic hormone and dehydroepiandrosterone sulfate). Screening for viral persistence (PCR in stool samples and SARS-CoV-2 spike antigen levels in plasma) in a subgroup of the patients with persistent PCS was negative. Sensitivity analyses (pre-existing illness/comorbidity, obesity, medical care of the index acute infection) revealed similar findings. Patients with persistent PCS and PEM reported more pain symptoms and had worse results in almost all tests. A limitation was that we had no objective information on exercise capacity and cognition before acute infection. In addition, we did not include patients unable to attend the outpatient clinic for whatever reason including severe illness, immobility or social deprivation or exclusion.
Conclusions: In this study, we observed that the majority of working age patients with PCS did not recover in the second year of their illness. Patterns of reported symptoms remained essentially similar, non-specific and dominated by fatigue, exercise intolerance and cognitive complaints. Despite objective signs of cognitive deficits and reduced exercise capacity, there was no major pathology in laboratory investigations, and our findings do not support viral persistence, EBV reactivation, adrenal insufficiency or increased complement turnover as pathophysiologically relevant for persistent PCS. A history of PEM was associated with more severe symptoms and more objective signs of disease and might help stratify cases for disease severity.
Copyright: © 2025 Peter et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures


References
-
- WHO Coronavirus (COVID-19) Dashboard. [cited 18 Oct 2023]. Available from: https://covid19.who.int
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

