Ethnic and racial differences in children and young people with respiratory and neurological post-acute sequelae of SARS-CoV-2: an electronic health record-based cohort study from the RECOVER Initiative
- PMID: 39850015
- PMCID: PMC11753962
- DOI: 10.1016/j.eclinm.2024.103042
Ethnic and racial differences in children and young people with respiratory and neurological post-acute sequelae of SARS-CoV-2: an electronic health record-based cohort study from the RECOVER Initiative
Abstract
Background: Children from racial and ethnic minority groups are at greater risk for severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection, but it is unclear whether they have increased risk for post-acute sequelae of SARS-CoV-2 (PASC). Our objectives were to assess whether the risk of respiratory and neurologic PASC differs by race/ethnicity and social drivers of health.
Methods: We conducted a retrospective cohort study of individuals <21 years seeking care at 24 health systems across the U.S, using electronic health record (EHR) data. Our cohort included those with a positive SARS-CoV-2 molecular, serology or antigen test, or with a COVID-19, multisystem inflammatory disease in children, or PASC diagnosis from February 29, 2020 to August 1, 2022. We identified children/youth with at least 2 codes associated with respiratory and neurologic PASC. We measured associations between sociodemographic and clinical characteristics and respiratory and neurologic PASC using odds ratios and 95% confidence intervals estimated from multivariable logistic regression models adjusted for other sociodemographic characteristics, social vulnerability index or area deprivation index, time period of cohort entry, presence and complexity of chronic respiratory (respectively, neurologic) condition and healthcare utilization.
Findings: Among 771,725 children in the cohort, 203,365 (26.3%) had SARS-CoV-2 infection. Among children with documented infection, 3217 children had respiratory PASC and 2009 children/youth had neurologic PASC. In logistic regression models, children <5 years (Odds Ratio [OR] 1.78, 95% CI 1.62-1.97), and of Hispanic White descent (OR 1.19, 95% CI 1.05-1.35) had higher odds of having respiratory PASC. Children/youth living in regions with higher area deprivation indices (OR 1.25, 95% CI 1.10-1.420 for 60-79th percentile) and with chronic complex respiratory conditions (OR 3.28, 95% CI 2.91-3.70) also had higher odds of respiratory PASC. In contrast, older (OR 1.57, 95% CI 1.40-1.77 for those aged 12-17 years), non-Hispanic White individuals and those with chronic pre-existing neurologic conditions (OR 2.04, 95% CI 1.78-2.35) were more likely to have a neurologic PASC diagnosis.
Interpretation: Racial and ethnic differences in healthcare utilization for neurologic and respiratory PASC may reflect social drivers of health and inequities in access to care.
Funding: National Institutes of Health.
Keywords: Chronic COVID-19 syndrome; Ethnicity; Late sequelae of COVID-19; Long COVID; Long-haul COVID; Long-term COVID-19; PCORnet; PEDSnet; Post-COVID condition; Post-COVID syndrome; Post-acute COVID-19; Post-acute sequelae of SARS-CoV-2 infection; Race; Social determinants of health.
© 2025 The Authors. Published by Elsevier Ltd.
Conflict of interest statement
Dr. Kleinman is Board Member for Dartnet Institute, and owns stocks with Glaxo, Amgen, Regeneron and Sanofi. Dr. Oliveira is on the Board of Directors for Eastern Society of Pediatric Research (ESPR) Executive Committee for American Academy of Pediatrics–Section on Epidemiology, Public Health, and Evidence (AAP-SOEPHE) Associate Editor for Journal of Pediatric Infectious Diseases Society. All other authors have no conflicts of interest to disclose.
Figures

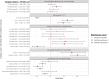
References
-
- Centers for Disease Control and Prevention Deaths by race and hispanic origin, ages 0-18 years. https://data.cdc.gov/NCHS/Deaths-by-Race-and-Hispanic-Origin-Ages-0-18-Y...
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

