Necrosis in Preoperative Cross-Sectional Imaging and Postoperative Histology Is a Diagnostic Marker for Malignancy of Adrenocortical Tumors
- PMID: 39851941
- PMCID: PMC11764034
- DOI: 10.3390/curroncol32010025
Necrosis in Preoperative Cross-Sectional Imaging and Postoperative Histology Is a Diagnostic Marker for Malignancy of Adrenocortical Tumors
Erratum in
-
Correction: Dukaczewska et al. Necrosis in Preoperative Cross-Sectional Imaging and Postoperative Histology Is a Diagnostic Marker for Malignancy of Adrenocortical Tumors. Curr. Oncol. 2025, 32, 25.Curr Oncol. 2025 Apr 2;32(4):210. doi: 10.3390/curroncol32040210. Curr Oncol. 2025. PMID: 40277799 Free PMC article.
Abstract
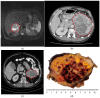
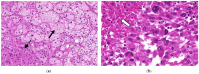
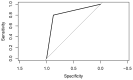
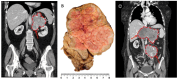
Necrosis in postoperative histology has been reported as being specific for adrenocortical carcinoma (ACC) compared to adenoma. We therefore retrospectively analyzed the diagnostic accuracy of the finding of necrosis in preoperative cross-sectional imaging and postoperative histology as a marker for ACC in our patient cohort. Among the 411 adrenalectomies in 396 patients performed between 2008 and April 2022, 30 cases of ACC (7.6%) were identified, with one tumor measuring less than 40 mm excluded. All 45 benign adrenocortical tumors of at least 40 mm in diameter, including Cushing, Conn, and hormonally inactive adenomas, served as controls. Preoperative imaging was available for 40 benign and 27 malignant adrenocortical tumors. In total, 10 of 40 (25%) benign adrenocortical tumors and 22 of 27 (81%) ACCs showed signs of possible necrosis in preoperative imaging. Pathologic examination confirmed necrosis in 1 of 40 (2.5%) benign tumors and in 26 out of 27 (96%) malignant tumors. The specificities of possible necrosis in preoperative imaging and necrosis in histology for diagnosing ACC were 75% and 97.5%, respectively, whereas the sensitivities were 81% and 96%, respectively. Signs of possible necrosis in radiologic imaging and tumor necrosis in histology proved to be very good predictive markers for the diagnosis of malignant adrenocortical tumors.
Keywords: adrenalectomy; adrenocortical adenoma; adrenocortical carcinoma; computed tomography; magnetic resonance imaging; tumor necrosis.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

References
-
- Gaujoux S., Mihai R., Joint Working Group of ESES and ENSAT European Society of Endocrine Surgeons (ESES) and European Network for the Study of Adrenal Tumours (ENSAT) recommendations for the surgical management of adrenocortical carcinoma. Br. J. Surg. 2017;104:358–376. doi: 10.1002/bjs.10414. - DOI - PubMed
-
- Fassnacht M., Arlt W., Bancos I., Dralle H., Newell-Price J., Sahdev A., Tabarin A., Terzolo M., Tsagarakis S., Dekkers O.M. Management of adrenal incidentalomas: European Society of Endocrinology Clinical Practice Guideline in collaboration with the European Network for the Study of Adrenal Tumors. Eur. J. Endocrinol. 2016;175:G1–G34. doi: 10.1530/EJE-16-0467. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous

