Romosozumab Improves Tissue Thickness-Adjusted Trabecular Bone Score in Women With Osteoporosis and Diabetes
- PMID: 39854280
- PMCID: PMC12448627
- DOI: 10.1210/clinem/dgae862
Romosozumab Improves Tissue Thickness-Adjusted Trabecular Bone Score in Women With Osteoporosis and Diabetes
Abstract
Context: Trabecular bone score (TBS), a gray-level texture index derived from lumbar spine (LS) dual-energy x-ray absorptiometry (DXA) scans, is decreased in patients with diabetes and is associated with increased fracture risk, independent of areal bone mineral density (aBMD), but potentially influenced by abdominal fat tissue.
Objective: Evaluate effect of romosozumab (210 mg monthly) for 12 months followed by alendronate (70 mg weekly) for 24 months vs alendronate alone (70 mg weekly) for 36 months on LS aBMD and TBS in women with type 2 diabetes (T2D) enrolled in the ARCH study.
Methods: This post hoc analysis included women from ARCH who had T2D at baseline and LS DXA scans at baseline and ≥1 postbaseline visit (romosozumab-to-alendronate, n = 165; alendronate-to-alendronate, n = 195). aBMD and TBS (determined by an updated tissue thickness-adjusted TBS algorithm [TBSTT]) were assessed on LS DXA scans at baseline and ≥1 postbaseline visit (months 12, 24, and 36).
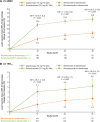
Results: Romosozumab led to significantly greater gains in LS aBMD and TBSTT at month 12 vs alendronate, and the greater gains with romosozumab were maintained after transition to alendronate and persisted significantly at months 24 and 36 vs alendronate alone. TBSTT percentage changes weakly correlated to LS aBMD percentage changes from baseline to month 36 (romosozumab-to-alendronate, R2 = 0.1493; alendronate-to-alendronate, R2 = 0.0429).
Conclusion: In postmenopausal women with osteoporosis and T2D, 12 months of romosozumab followed by 24 months of alendronate vs alendronate alone significantly improved LS aBMD and TBSTT (independently of abdominal fat) and to a greater extent. Hence, romosozumab may improve bone strength in patients with T2D.
Trial registration: ClinicalTrials.gov-NCT01631214.
Keywords: DXA; anabolic; bone mineral density; fracture risk; osteoporosis; type 2 diabetes (T2D).
© The Author(s) 2025. Published by Oxford University Press on behalf of the Endocrine Society.
Figures



References
-
- Bonds DE, Larson JC, Schwartz AV, et al. Risk of fracture in women with type 2 diabetes: the women’s health initiative observational study. J Clin Endocrinol Metab. 2006;91(9):3404‐3410. - PubMed
-
- Paccou J, Ward KA, Jameson KA, Dennison EM, Cooper C, Edwards MH. Bone microarchitecture in men and women with diabetes: the importance of cortical porosity. Calcif Tissue Int. 2016;98(5):465‐473. - PubMed
-
- Nilsson AG, Sundh D, Johansson L, et al. Type 2 diabetes mellitus is associated with better bone microarchitecture but lower bone material strength and poorer physical function in elderly women: a population-based study. J Bone Miner Res. 2017;32(5):1062‐1071. - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

