Inflammatory Biomarkers and Lipid Parameters May Predict an Increased Risk for Atrial Arrhythmias in Patients with Systemic Sclerosis
- PMID: 39857802
- PMCID: PMC11762971
- DOI: 10.3390/biomedicines13010220
Inflammatory Biomarkers and Lipid Parameters May Predict an Increased Risk for Atrial Arrhythmias in Patients with Systemic Sclerosis
Abstract
Background/objectives: Autoimmune inflammation enhances the electrical instability of the atrial myocardium in patients with systemic sclerosis (SSc); thus, atrial arrhythmia risk is increased, which might be predicted by evaluating the P wave interval and dispersion of a 12-lead surface electrocardiogram (ECG).
Methods: We examined 26 SSc patients and 36 healthy controls and measured the P wave interval and P wave dispersion of the 12-lead surface ECG in each patient. Furthermore, echocardiography and 24-h Holter ECG were performed and levels of inflammatory laboratory parameters, including serum progranulin (PGRN), sVCAM-1, sICAM-1, leptin and C-reactive protein (CRP), were determined. Lipid parameters, such as Apo A-I, LDL-cholesterol (LDL-C), oxidized LDL (oxLDL) and the LDL and HDL subfractions were also evaluated.
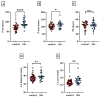
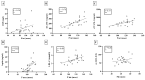
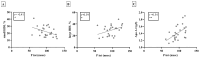
Results: The P wave interval showed a significant positive correlation with the levels of Apo A-I, LDL-C, CRP, sVCAM-1, sICAM-1 and leptin. The oxLDL level correlated positively with P wave dispersion. Of note, significant positive correlation was also found between the large HDL percentage and the P wave interval.
Conclusions: Our results suggest that PGRN, sVCAM-1, sICAM-1, leptin, CRP, LDL-C and oxLDL, along with LDL and HDL subfractions, might have a role in atrial arrhythmogenesis in patients with SSc.
Keywords: LDL and HDL subfractions; atrial arrhythmias; electrocardiography; inflammation; leptin; oxLDL; systemic sclerosis.
Conflict of interest statement
The authors declare no conflicts of interest. The funders had no role in the design of the study; in the collection, analyses or interpretation of data; in the writing of the manuscript; or in the decision to publish the results.
Figures
Similar articles
-
Progranulin, sICAM-1, and sVCAM-1 May Predict an Increased Risk for Ventricular Arrhythmias in Patients with Systemic Sclerosis.Int J Mol Sci. 2024 Jul 5;25(13):7380. doi: 10.3390/ijms25137380. Int J Mol Sci. 2024. PMID: 39000486 Free PMC article.
-
Determination of Serum Progranulin in Patients with Untreated Familial Hypercholesterolemia.Biomedicines. 2022 Mar 25;10(4):771. doi: 10.3390/biomedicines10040771. Biomedicines. 2022. PMID: 35453521 Free PMC article.
-
Weight loss achieved by bariatric surgery modifies high-density lipoprotein subfractions and low-density lipoprotein oxidation towards atheroprotection.Clin Biochem. 2019 Jan;63:46-53. doi: 10.1016/j.clinbiochem.2018.10.007. Epub 2018 Oct 17. Clin Biochem. 2019. PMID: 30342017 Clinical Trial.
-
Effects of Pitavastatin on Lipoprotein Subfractions and Oxidized Low-density Lipoprotein in Patients with Atherosclerosis.Curr Med Sci. 2020 Oct;40(5):879-884. doi: 10.1007/s11596-020-2263-4. Epub 2020 Oct 29. Curr Med Sci. 2020. PMID: 33123903
-
High-sensitivity C-reactive protein and atherosclerotic disease: from improved risk prediction to risk-guided therapy.Int J Cardiol. 2013 Oct 15;168(6):5126-34. doi: 10.1016/j.ijcard.2013.07.113. Epub 2013 Aug 24. Int J Cardiol. 2013. PMID: 23978367 Review.
References
-
- Tzelepis G.E., Kelekis N.L., Plastiras S.C., Mitseas P., Economopoulos N., Kampolis C., Gialafos E.J., Moyssakis I., Moutsopoulos H.M. Pattern and distribution of myocardial fibrosis in systemic sclerosis: A delayed enhanced magnetic resonance imaging study. Arthritis Rheum. 2007;56:3827–3836. doi: 10.1002/art.22971. - DOI - PubMed
-
- Bruni C., Buch M.H., Furst D.E., De Luca G., Djokovic A., Dumitru R.B., Giollo A., Polovina M., Steelandt A., Bratis K., et al. Primary systemic sclerosis heart involvement: A systematic literature review and preliminary data-driven, consensus-based WSF/HFA definition. J. Scleroderma Relat. Disord. 2022;7:24–32. doi: 10.1177/23971983211053246. - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

