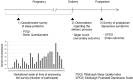
Association between sleep problems during pregnancy and postpartum depressive symptoms as well as condition of newborn at delivery
- PMID: 39865440
- PMCID: PMC11771626
- DOI: 10.1111/jog.16219
Association between sleep problems during pregnancy and postpartum depressive symptoms as well as condition of newborn at delivery
Abstract
Background: Pregnancy-related anatomic, physiologic, and hormonal factors can occur at different stages of pregnancy and affect sleep disturbances. The relationship between sleep problems during pregnancy and postpartum depressive symptoms as well as neonatal condition at delivery have not been well described. This study hypothesized that sleep problems are associated with postpartum depressive symptoms and adverse neonatal outcomes at delivery.
Methods: This study conducted a prospective study for perinatal women (n = 683, 30.54 ± 5.11 years old) to evaluate sleep problems during pregnancy using the Pittsburgh sleep quality index (PSQI) and Berlin questionnaire, postpartum depressive symptoms using Edinburgh postnatal depression scale (EPDS), and clinical signs of neonatal condition at delivery using the Apgar score.
Results: PSQI total score during pregnancy were significantly higher in those with postpartum depressive symptoms than those without 1 month after delivery. PSQI score in the third trimester was significantly associated with postpartum depressive symptoms even after adjustment for relevant confounding factors and self-reported lifetime depression (odds ratio = 1.19, 95% confidence interval = 1.03-1.36, p = 0.015). The Apgar score at 5 min after birth was significantly lower in those with obstructive sleep apnea (OSA) than those without OSA in the second and third trimesters, although mean scores were within the normal range.
Conclusion: This study revealed that sleep problems during pregnancy influence postpartum depression 1 month after delivery. OSA during pregnancy may lead to risks of delivery. Attention should be paid to sleep health during pregnancy to ensure the mental health of mothers and a safe delivery.
Keywords: Apgar score; postpartum depression; pregnancy; sleep apnea; sleep problem.
© 2025 The Author(s). Journal of Obstetrics and Gynaecology Research published by John Wiley & Sons Australia, Ltd on behalf of Japan Society of Obstetrics and Gynecology.
Conflict of interest statement
Yoko Komada received honorarium from Eisai co. Sho‐Ichi Kawakami received grants or lecture fees from Tsumura & Co., Kracie Holdings, Ltd., Bayer Yakuhin, Ltd., and Pfizer Japan Inc. outside the submitted work. Azusa Ikegami received grants or lecture fee from Esai Corp., MSD Corp., Takeda Pharmaceutical, Astrazeneca Corp., Teijin Healthcare Ltd., Novartis Pharma Corp., Towa Pharmaceutica, ResMed, Taisyo Pharma. Co., Idorsia Pharmaceuticals Japan Ltd., outside the submitted work. Satoko Furuie and Rena Mori declare no competing interests.
Figures
Similar articles
-
Antepartum sleep quality, mental status, and postpartum depressive symptoms: a mediation analysis.BMC Psychiatry. 2022 Aug 2;22(1):521. doi: 10.1186/s12888-022-04164-y. BMC Psychiatry. 2022. PMID: 35918689 Free PMC article.
-
Sleeping problems during pregnancy-a risk factor for postnatal depressiveness.Arch Womens Ment Health. 2019 Jun;22(3):327-337. doi: 10.1007/s00737-018-0903-5. Epub 2018 Aug 18. Arch Womens Ment Health. 2019. PMID: 30121844
-
Sleep habits and problems across gestational progress in Japanese women.J Obstet Gynaecol Res. 2023 Apr;49(4):1137-1143. doi: 10.1111/jog.15573. Epub 2023 Feb 6. J Obstet Gynaecol Res. 2023. PMID: 36746646
-
The intrapartum and perinatal risks of sleep-disordered breathing in pregnancy: a systematic review and metaanalysis.Am J Obstet Gynecol. 2018 Aug;219(2):147-161.e1. doi: 10.1016/j.ajog.2018.02.004. Epub 2018 Feb 15. Am J Obstet Gynecol. 2018. PMID: 29454869
-
Anxious and depressive components of Edinburgh Postnatal Depression Scale in maternal postpartum psychological problems.J Perinat Med. 2013 Jul;41(4):343-8. doi: 10.1515/jpm-2012-0258. J Perinat Med. 2013. PMID: 23426862 Review.
Cited by
-
Psychological Distress and Maternal Outcomes in Women With Pre-eclampsia: A Retrospective Case-Control Study.Health Sci Rep. 2025 Aug 6;8(8):e71133. doi: 10.1002/hsr2.71133. eCollection 2025 Aug. Health Sci Rep. 2025. PMID: 40772116 Free PMC article.
References
-
- Bloch M, Schmidt PJ, Danaceau M, Murphy J, Nieman L, Rubinow DR. Effects of gonadal steroids in women with a history of postpartum depression. Am J Psychiatry. 2000;157(6):924–930. - PubMed
-
- Wisner KL, Parry BL, Piontek CM. Clinical practice. Postpartum depression. N Engl J Med. 2002;347(3):194–199. - PubMed
-
- Stremler R, Sharkey KM. Postpartum period and early parenthood. In: Kryger MH, Roth T, Goldstein CA, editors. Principles and practice of sleep medicine. 7th ed. Philadelphia: Elsevier; 2022. p. 1773–1780.
-
- Ford DE, Kamerow DB. Epidemiologic study of sleep disturbances and psychiatric disorders. An opportunity for prevention? JAMA. 1989;262(11):1479–1484. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical