Sodium-glucose cotransporter 2 inhibitors in patients with type 2 diabetes and myocardial infarction undergoing percutaneous coronary intervention: A systematic review and meta-analysis
- PMID: 39867488
- PMCID: PMC11757226
- DOI: 10.1016/j.ajpc.2024.100927
Sodium-glucose cotransporter 2 inhibitors in patients with type 2 diabetes and myocardial infarction undergoing percutaneous coronary intervention: A systematic review and meta-analysis
Abstract
Background: Sodium-glucose cotransporter 2 inhibitors (SGLT2i) have shown benefits in improving cardiovascular (CV) outcomes in patients with heart failure (HF) and may mitigate symptom progression in myocardial infarction (MI). However, their effectiveness in patients with type 2 diabetes and MI undergoing percutaneous coronary intervention (PCI) is unclear.
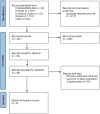
Methods: To identify eligible studies, a comprehensive search of electronic databases, PubMed, Cochrane Library, Scopus and Embase, was conducted from inception until May 2024. Results were presented as risk ratios (RR) and their corresponding 95 % confidence intervals (CIs).
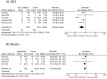
Results: Our analysis included 8 observational studies comprising 24,229 patients. The results indicated that SGLT2i with PCI was associated with a significantly reduced risk of all-cause death (RR=0.61; 95 % CI=0.54 to 0.68), CV death (RR=0.46; 95 % CI=0.22 to 0.94), major adverse cardiovascular events (RR=0.80;95 % CI: 0.66 to 0.96), HF-related hospitalizations (RR=0.63; 95 % CI=0.44 to 0.90), stroke (RR=0.77; 95 % CI: 0.62 to 0.96) and acute kidney injury (RR=0.46; 95 % CI: 0.25 to 0.84) compared to PCI without SGLT2i use. However, the risk of revascularization remained comparable between the groups.
Conclusion: Our study demonstrates that SGLT2i with PCI in patients with type 2 diabetes and MI are associated with improved CV outcomes compared to PCI without SGLT2i use. Randomized controlled trials are required to confirm the improvement in outcomes with SGLT2i therapy combined with PCI in patients with MI and diabetes.
Keywords: Myocardial infarction; Percutaneous coronary intervention; Sodium-glucose co-transporter 2 inhibitors; Type 2 diabetes.
© 2024 The Authors.
Conflict of interest statement
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Figures



References
-
- Reed G.W., Rossi J.E., Cannon C.P. Acute myocardial infarction. Lancet. 2017;389(10065):197–210. Jan 14. - PubMed
-
- Benjamin E.J., Virani S.S., Callaway C.W., Chamberlain A.M., Chang A.R., Cheng S., et al. Heart disease and stroke statistics-2018 update: a report from the american heart association. Circulation. 2018;137(12):e67–492. Mar 20. - PubMed
-
- Byrne R.A., Rossello X., Coughlan J.J., Barbato E., Berry C., Chieffo A., et al. 2023 ESC Guidelines for the management of acute coronary syndromes. Eur Heart J. 2023;44(38):3720–3826. Oct 12. - PubMed
-
- Tsai T.T., Patel U.D., Chang T.I., Kennedy K.F., Masoudi F.A., Matheny M.E., et al. Contemporary incidence, predictors, and outcomes of acute kidney injury in patients undergoing percutaneous coronary interventions: insights from the NCDR Cath-PCI registry. JACC Cardiovasc Interv. 2014;7(1):1–9. Jan. - PMC - PubMed
-
- Ritsinger V., Nyström T., Saleh N., Lagerqvist B., Norhammar A. Heart failure is a common complication after acute myocardial infarction in patients with diabetes: a nationwide study in the SWEDEHEART registry. Eur J Prev Cardiol. 2020;27(17):1890–1901. Nov. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

