Mass Casualty Incident Training in Immersive Virtual Reality: Quasi-Experimental Evaluation of Multimethod Performance Indicators
- PMID: 39869892
- PMCID: PMC11811659
- DOI: 10.2196/63241
Mass Casualty Incident Training in Immersive Virtual Reality: Quasi-Experimental Evaluation of Multimethod Performance Indicators
Abstract
Background: Immersive virtual reality (iVR) has emerged as a training method to prepare medical first responders (MFRs) for mass casualty incidents (MCIs) and disasters in a resource-efficient, flexible, and safe manner. However, systematic evaluations and validations of potential performance indicators for virtual MCI training are still lacking.
Objective: This study aimed to investigate whether different performance indicators based on visual attention, triage performance, and information transmission can be effectively extended to MCI training in iVR by testing if they can discriminate between different levels of expertise. Furthermore, the study examined the extent to which such objective indicators correlate with subjective performance assessments.
Methods: A total of 76 participants (mean age 25.54, SD 6.01 y; 45/76, 59% male) with different medical expertise (MFRs: paramedics and emergency physicians; non-MFRs: medical students, in-hospital nurses, and other physicians) participated in 5 virtual MCI scenarios of varying complexity in a randomized order. Tasks involved assessing the situation, triaging virtual patients, and transmitting relevant information to a control center. Performance indicators included eye-tracking-based visual attention, triage accuracy, triage speed, information transmission efficiency, and self-assessment of performance. Expertise was determined based on the occupational group (39/76, 51% MFRs vs 37/76, 49% non-MFRs) and a knowledge test with patient vignettes.
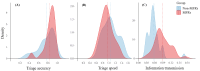
Results: Triage accuracy (d=0.48), triage speed (d=0.42), and information transmission efficiency (d=1.13) differentiated significantly between MFRs and non-MFRs. In addition, higher triage accuracy was significantly associated with higher triage knowledge test scores (Spearman ρ=0.40). Visual attention was not significantly associated with expertise. Furthermore, subjective performance was not correlated with any other performance indicator.
Conclusions: iVR-based MCI scenarios proved to be a valuable tool for assessing the performance of MFRs. The results suggest that iVR could be integrated into current MCI training curricula to provide frequent, objective, and potentially (partly) automated performance assessments in a controlled environment. In particular, performance indicators, such as triage accuracy, triage speed, and information transmission efficiency, capture multiple aspects of performance and are recommended for integration. While the examined visual attention indicators did not function as valid performance indicators in this study, future research could further explore visual attention in MCI training and examine other indicators, such as holistic gaze patterns. Overall, the results underscore the importance of integrating objective indicators to enhance trainers' feedback and provide trainees with guidance on evaluating and reflecting on their own performance.
Keywords: disaster medicine; emergency medicine; emergency simulation; eye tracking; mass casualty incident; medical education; prehospital decision-making; virtual reality.
©Anke Sabine Baetzner, Yannick Hill, Benjamin Roszipal, Solène Gerwann, Matthias Beutel, Tanja Birrenbach, Markus Karlseder, Stefan Mohr, Gabriel Alexander Salg, Helmut Schrom-Feiertag, Marie Ottilie Frenkel, Cornelia Wrzus. Originally published in the Journal of Medical Internet Research (https://www.jmir.org), 27.01.2025.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures


Similar articles
-
Exploring the role of virtual reality in preparing emergency responders for mass casualty incidents.Isr J Health Policy Res. 2025 Apr 9;14(1):22. doi: 10.1186/s13584-025-00681-9. Isr J Health Policy Res. 2025. PMID: 40205512 Free PMC article.
-
Exploring medical first responders' perceptions of mass casualty incident scenario training: a qualitative study on learning conditions and recommendations for improvement.BMJ Open. 2024 Jul 11;14(7):e084925. doi: 10.1136/bmjopen-2024-084925. BMJ Open. 2024. PMID: 38991686 Free PMC article.
-
The Use of Smartphone-Based Highly Realistic MCI Training as an Adjunct to Traditional Training Methods.Mil Med. 2024 Aug 19;189(Suppl 3):775-783. doi: 10.1093/milmed/usae274. Mil Med. 2024. PMID: 39160830
-
Extended reality training for mass casualty incidents: a systematic review on effectiveness and experience of medical first responders.Int J Emerg Med. 2024 Aug 23;17(1):99. doi: 10.1186/s12245-024-00685-3. Int J Emerg Med. 2024. PMID: 39179965 Free PMC article. Review.
-
A Qualitative Assessment of Studies Evaluating the Classification Accuracy of Personnel Using START in Disaster Triage: A Scoping Review.Front Public Health. 2022 Feb 24;10:676704. doi: 10.3389/fpubh.2022.676704. eCollection 2022. Front Public Health. 2022. PMID: 35284379 Free PMC article.
References
-
- Lomaglio L, Ansaloni L, Catena F, Sartelli M, Coccolini F. Mass casualty incident: definitions and current reality. In: Kluger Y, Coccolini F, Catena F, Ansaloni L, editors. WSES Handbook of Mass Casualties Incidents Management. Cham, Switzerland: Springer; 2020.
-
- Berndt H, Wessel D, Willer L, Herczeg M, Mentler T. Immersion and presence in virtual reality training for mass casualty incidents. Proceedings of the 15th ISCRAM Conference; ISCRAM 2015; May 20-23, 2018; Rochester, NY. 2018. - DOI
-
- Mills B, Dykstra P, Hansen S, Miles A, Rankin T, Hopper L, Brook L, Bartlett D. Virtual reality triage training can provide comparable simulation efficacy for paramedicine students compared to live simulation-based scenarios. Prehosp Emerg Care. 2020;24(4):525–36. doi: 10.1080/10903127.2019.1676345. - DOI - PubMed
-
- Baetzner AS, Wespi R, Hill Y, Gyllencreutz L, Sauter TC, Saveman BI, Mohr S, Regal G, Wrzus C, Frenkel MO. Preparing medical first responders for crises: a systematic literature review of disaster training programs and their effectiveness. Scand J Trauma Resusc Emerg Med. 2022;30(1):76. doi: 10.1186/s13049-022-01056-8. https://sjtrem.biomedcentral.com/articles/10.1186/s13049-022-01056-8 10.1186/s13049-022-01056-8 - DOI - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources

