Association of preoperative body mass index with postoperative complications and survival for patients with gastric cancer: A systematic review and meta-analysis
- PMID: 39874306
- PMCID: PMC11774357
- DOI: 10.1371/journal.pone.0317985
Association of preoperative body mass index with postoperative complications and survival for patients with gastric cancer: A systematic review and meta-analysis
Abstract
Objective: The relationship among body mass index (BMI), postoperative complications, and clinical outcomes in patients undergoing gastrectomy for gastric cancer remains unclear. This study aimed to evaluate this association using a meta-analysis.
Method: We conducted a systematic search of the PubMed, Embase, and Cochrane Library databases up to February 25, 2024. Patients were classified into underweight (<18.5 kg/m2), normal weight (18.5-25.0 kg/m2), and overweight (≥25.0 kg/m2) groups based on BMI categories. Meta-analysis was performed using a random-effects model. Additionally, exploratory sensitivity and subgroup analyses were performed.
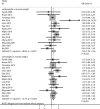
Results: Twenty-two studies involving 41,144 patients with gastric cancer were included for quantitative analysis. Preoperative underweight (odds ratio [OR]: 1.26; 95% confidence interval [CI]: 1.03-1.55; P = 0.024) and overweight (OR: 1.19; 95%CI: 1.09-1.30; P <0.001) were associated with an increased risk of postoperative complications. Furthermore, preoperative underweight was associated with poorer overall survival (hazard ratio [HR]: 1.40; 95%CI: 1.28-1.53; P <0.001), whereas preoperative overweight was associated with better over-survival (HR: 0.82; 95%CI: 0.73-0.91; P <0.001). Furthermore, preoperative underweight was not associated with disease-free survival (HR: 1.48; 95%CI: 0.97-2.26; P = 0.069), whereas preoperative overweight was associated with longer disease-free survival (HR: 0.80; 95%CI: 0.70-0.91; P = 0.001). In terms of specific postoperative complications, preoperative underweight was associated with an increased risk of septic shock (OR: 3.40; 95%CI: 1.26-9.17; P = 0.015) and a reduced risk of fever (OR: 0.39; 95%CI: 0.18-0.83; P = 0.014). Preoperative overweight was associated with an increased risk of wound infections (OR: 1.78; 95%CI: 1.08-2.93; P = 0.023), intestinal fistula (OR: 5.23; 95%CI: 1.93-14.21; P = 0.001), arrhythmia (OR: 6.38; 95%CI: 1.70-24.01; P = 0.006), and pancreatic fistula (OR: 3.37; 95%CI: 1.14-9.96; P = 0.028).
Conclusion: This study revealed that both preoperative underweight and overweight status were associated with an increased risk of postoperative complications. Moreover, the postoperative survival outcomes were significantly better in overweight compared to that of underweight patients.
Trial registration: Registration: INPLASY202480004.
Copyright: © 2025 Li et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Similar articles
-
The impact of preoperative skeletal muscle mass index-defined sarcopenia on postoperative complications and survival in gastric cancer: An updated meta-analysis.Eur J Surg Oncol. 2025 Mar;51(3):109569. doi: 10.1016/j.ejso.2024.109569. Epub 2024 Dec 28. Eur J Surg Oncol. 2025. PMID: 39794171
-
Muscle attenuation, not skeletal muscle index, is an independent prognostic factor for survival in gastric cancer patients with overweight and obesity.Nutrition. 2024 Jun;122:112391. doi: 10.1016/j.nut.2024.112391. Epub 2024 Feb 8. Nutrition. 2024. PMID: 38460446
-
The impact of body mass index on colorectal surgery: A short-term outcome and cost analysis in an Asian cohort of 3169 patients.Colorectal Dis. 2025 Aug;27(8):e70192. doi: 10.1111/codi.70192. Colorectal Dis. 2025. PMID: 40751348
-
Preoperative weight loss and postoperative pancreatic fistula risk affected by body mass index: a National Surgical Quality Improvement Program study.J Gastrointest Surg. 2025 Sep;29(9):102157. doi: 10.1016/j.gassur.2025.102157. Epub 2025 Jul 14. J Gastrointest Surg. 2025. PMID: 40669805
-
Overweight, obesity and gastric cancer risk: results from a meta-analysis of cohort studies.Eur J Cancer. 2009 Nov;45(16):2867-73. doi: 10.1016/j.ejca.2009.04.019. Epub 2009 May 6. Eur J Cancer. 2009. PMID: 19427197
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical