Normative values for lung, bronchial sizes, and bronchus-artery ratios in chest CT scans: from infancy into young adulthood
- PMID: 39891681
- PMCID: PMC12226683
- DOI: 10.1007/s00330-025-11367-w
Normative values for lung, bronchial sizes, and bronchus-artery ratios in chest CT scans: from infancy into young adulthood
Abstract
Objective: To estimate the developmental trends of quantitative parameters obtained from chest computed tomography (CT) and to provide normative values on dimensions of bronchi and arteries, as well as bronchus-artery (BA) ratios from preschool age to young adulthood.
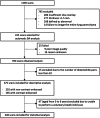
Materials and methods: Two independent radiologists screened a dataset of 1160 chest CT scans, initially reported as normal, from participants aged 0 to 24 years. Using an automated deep learning-based algorithm, we computed the following bronchus and artery parameters: bronchial outer diameter (Bout), bronchial inner diameter (Bin), adjacent pulmonary artery diameter (A), bronchial wall thickness (Bwt), bronchial wall area (BWA), and bronchial outer area (BOA). From these parameters, we computed the following ratios: Bout/A, Bin/A, Bwt/A, Bwt/Bout, and BWA/BOA. Furthermore, mean lung density, total lung volume, and the square root of wall area of bronchi with a 10-mm lumen perimeter (Pi10) were obtained. The effects on CT parameters of age, sex, and iodine contrast were investigated using mixed-effects or regression model analyses.
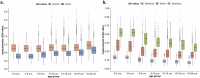
Results: 375 normal inspiratory chest CT scans (females / males = 156 / 219; mean age [SD] 12.7 [5.0] years) met the inclusion criteria. Bout and Bin progressively increased with age (all p < 0.05), but Bwt, Bout/A, Bin/A, Bwt/A, Bwt/Bout, or BWA/BOA did not. Total lung volume and mean lung density continuously increased with age (both p < 0.001), while Pi10 did not exhibit such a trend. Bout, total lung volume, and mean lung density were the only parameters that differed between males and females, all higher in males than females (all p < 0.03). The presence of iodinated contrast led to greater values for Bwt, Bwt/Bout, and BWA/BOA, but lower values for Bin, Bout/A, Bin/A, and Bwt/A (all p < 0.01).
Conclusion: Quantitative CT parameters of both lung parenchyma and bronchi exhibit growth-related changes, but from 6 to 24 years ratios between bronchus and artery dimensions remain constant. Contrast-enhanced CT scans affect the assessment of lung parenchyma and bronchial size. We propose age and technique-dependent normative values for bronchial dimensions and wall thickness.
Key points: Question What are the developmental trends of quantitative lung CT parameters in patients from childhood into young adulthood? Findings The ratio between bronchus and pulmonary artery dimensions demonstrates consistent values across age groups, indicating synchronized growth between bronchi and paired pulmonary arteries. Clinical relevance Our findings highlight the importance of standardized CT protocol and volume acquisition, and emphasize the need for ongoing collection of normal chest CT scans to refine the proposed reference values.
Keywords: Adolescents; Bronchi; Computer-assisted diagnosis; Reference values.
© 2025. The Author(s).
Conflict of interest statement
Compliance with ethical standards. Guarantor: The scientific guarantor of this publication is Dr. Pierluigi Ciet. Conflict of interest: The author of this manuscript, Harm Tiddens, declares relationships with the following companies: Insmed, TBIO, Thirona, Neupharma and Boehringer. The author of this manuscript, Jean-Paul Charbonnier, declares relationships with Thirona. Daan Caudri is director of the Erasmus MC-LungAnalysis laboratory. The author of this manuscript, Pierluigi Ciet, declares relationships with the following companies: Vertex Pharmaceutical, Chiesi Pharmaceuticals, and Siemens Healthineers. Wieying Kuo is affiliated with Voiant Clinical. The rest of the authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article. Statistics and biometry: One of the authors, Eleni-Rosalina Andrinopoulou, has significant statistical expertise. Informed consent: Written informed consent was not required for this study because this is a retrospective study. Ethical approval: Institutional Review Board approval was obtained. Study subjects or cohorts overlap: The cohort has been previously reported in Kuo et al [6]. In the previous study, the dataset consisted of 294 out of 1160 chest CT scans of children and adolescents were collected retrospectively by the international multicenter Normal Chest CT Study Group. The previous study aimed to define normative data on central airway dimensions, in particular trachea, right main bronchi, and left main bronchi, in chest CT of children. On these 294 inspiratory CT scans, central airways were semi-automatically analyzed using Myrian XP-Lung software (version 1.19.1, Intrasense). The intrathoracic tracheal length was measured from the carina to the thorax inlet manually. In the recent study, the dataset consisted of 375 out of 1160 chest CT scans of children and young adults. The primary aim of the current study is to establish normative data for the dimensions of peripheral airways extending down to the 6th bronchial generation, in chest CT of children. On these 375 inspiratory CT scans, bronchi and adjacent pulmonary arteries were automatically analyzed using LungQ (version 2.0.1, Thirona). Using this algorithm, we computed the following bronchus and artery parameters from segmental bronchi to the most peripheral detectable bronchi: bronchial outer diameter (Bout), bronchial inner diameter (Bin), adjacent pulmonary artery diameter (A), bronchial wall thickness (Bwt), bronchial wall area (BWA), and bronchial outer area (BOA). From these parameters, we computed the following ratios: Bout/A, Bin/A, Bwt/A, Bwt/Bout, and BWA/BOA. Furthermore, mean lung density, total lung volume, and the square root of wall area of bronchi with a 10-mm lumen perimeter (Pi10) were obtained by using another module from the same software package. Methodology: Retrospective Observational Multicenter study
Figures

References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

