Severe Guillain-Barré syndrome with concurrent optic neuritis in a pediatric patient: a case report
- PMID: 39896802
- PMCID: PMC11781990
- DOI: 10.3389/fimmu.2024.1517943
Severe Guillain-Barré syndrome with concurrent optic neuritis in a pediatric patient: a case report
Abstract
Introduction: Guillain-Barré syndrome (GBS) is a rare, immune-mediated polyneuropathy primarily affecting the peripheral nervous system. Diagnosis is often supported by neuroconduction studies showing polyradiculoneuropathy and cerebrospinal fluid (CSF) analysis revealing albumin-cytological dissociation. However, these features may not appear in the early stages, leading to potential misdiagnosis. The central nervous system (CNS) is generally not affected due to differences in antigen expression, optic neuritis (ON), a demyelinating inflammation of the optic nerve, occasionally co-occurs with GBS as a rare variant. Although GBS can manifest with various neurological symptoms, the co-occurrence of optic neuritis (ON) is rare, especially in pediatric cases. This report documents the first known case in China of a child with severe GBS complicated by ON, which developed following an upper respiratory infection.
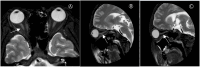
Case presentation: A 14-year-old male presented with acute progressive quadriparesis and visual impairment following a febrile illness. On admission, he displayed severe respiratory and autonomic instability requiring mechanical ventilation. Neurological examination revealed flaccid paralysis of all four limbs with absent reflexes, along with bilateral optic neuritis, confirmed by MRI showing inflammation of the optic nerve. Initial cerebrospinal fluid (CSF) analysis was normal, but subsequent testing revealed elevated protein levels typical of GBS. Neurophysiological studies indicated widespread demyelinating and axonal damage.
Interventions and outcomes: The patient received intravenous immunoglobulin (IVIG) therapy, high-dose corticosteroids, and, given the severe progression, rituximab. Despite initial worsening, gradual improvement in muscle strength and visual acuity was observed over several weeks. At three months, the patient was discharged with significantly restored function, with muscle strength nearing baseline and partial visual recovery.
Conclusion: This case highlights the clinical complexity of GBS with ON in pediatric patients, emphasizing the importance of timely immunomodulatory treatment. It also underscores the need for awareness of overlapping central and peripheral autoimmune neuropathies to improve diagnostic accuracy and patient outcomes.
Keywords: Guillain-Barré syndrome; case report; immunotherapy; optic neuritis; pediatric neurology; rituximab.
Copyright © 2025 Xue, Bao, Yu, Li, Liu and Li.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures

References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

