Predictive Value of NT-proBNP for Functional Outcome of Ischemic Stroke Without Cardiac Disease: A Prospective, Observational Study
- PMID: 39897711
- PMCID: PMC11784306
- DOI: 10.2147/NDT.S488574
Predictive Value of NT-proBNP for Functional Outcome of Ischemic Stroke Without Cardiac Disease: A Prospective, Observational Study
Erratum in
-
Erratum: Predictive Value of NT-proBNP for Functional Outcome of Ischemic Stroke Without Cardiac Disease: A Prospective, Observational Study [Corrigendum].Neuropsychiatr Dis Treat. 2025 Mar 10;21:539-540. doi: 10.2147/NDT.S526646. eCollection 2025. Neuropsychiatr Dis Treat. 2025. PMID: 40093026 Free PMC article.
Abstract
Purpose: Our study aimed to evaluate the prognostic value of NT-proBNP in predicting adverse outcomes among patients with anterior circulation infarction (ACI) and posterior circulation infarction (PCI), specifically in those without pre-existing cardiac comorbidities.
Patients and methods: This single-center, prospective observational study enrolled patients with acute ischemic stroke (AIS) within 7 days of symptom onset. We aimed to elucidate predictive role of NT-proBNP levels in determining adverse outcomes in AIS patients. Additionally, the study sought to explore the relationship between NT-proBNP levels and the risk of poor functional outcomes in both ACI and PCI patients without underlying cardiac comorbidities.
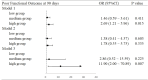
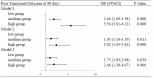
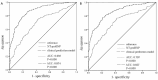
Results: A total of 821 patients were included in our study. Both univariate and multivariate logistic analyses indicated that higher NT-proBNP was an independent risk factor for adverse outcomes of ischemic stroke patients at 90 days. In noncardiogenic patients, the risks of adverse outcomes during follow-up were significantly elevated in the medium and high NT-proBNP groups (medium group: OR 1.75, 95% CI 1.03-2.98, P=0.039; high group: OR 2.46, 95% CI 1.30-4.67, P=0.006), with a dose-dependent trend. The association was similarly observed in patients with isolated ACI (medium group: OR 2.02, 95% CI 1.06-3.83, P=0.031; high group: OR 2.70, 95% CI 1.25-5.79, P=0.011). High NT-proBNP levels were independently associated with END in patients without underlying cardiac comorbidities (high group: OR 2.14, 95% CI 1.06-4.31, P=0.033) and this association was also observed in ACI patients (high group: OR 5.39, 95% CI 1.70-17.04, P=0.004). Moreover, when incorporated into the clinical prediction model, NT-proBNP exhibited excellent sensitivity and specificity for predicting stroke-related functional outcomes.
Conclusion: NT-proBNP demonstrates potential as a valuable biomarker in the clinical predictive model for functional outcomes specifically in ACI patients suggesting that elevated NT-proBNP levels in these patients should prompt closer monitoring and more comprehensive patient management.
Trial registration: https://www.chictr.org.cn/, ChiCTR2300067696.
Keywords: NT-proBNP; anterior circulation infarction; functional outcomes; posterior circulation infarction.
© 2025 Liu et al.
Conflict of interest statement
The authors report no conflicts of interest in this work.
Figures



Similar articles
-
Elevated NT-proBNP predicts unfavorable outcomes in patients with acute ischemic stroke after thrombolytic therapy.BMC Neurol. 2023 May 23;23(1):203. doi: 10.1186/s12883-023-03222-6. BMC Neurol. 2023. PMID: 37221489 Free PMC article.
-
Cardiac biomarkers are associated with increased risks of adverse clinical outcomes after ischemic stroke.J Neurol. 2024 Sep;271(9):6313-6324. doi: 10.1007/s00415-024-12536-5. Epub 2024 Aug 6. J Neurol. 2024. PMID: 39105893
-
Serum NT-proBNP level for predicting functional outcomes after acute ischemic stroke.Sci Rep. 2023 Aug 25;13(1):13903. doi: 10.1038/s41598-023-41233-y. Sci Rep. 2023. PMID: 37626208 Free PMC article.
-
Prognostic Value of NT-proBNP After Ischemic Stroke: A Systematic Review and Meta-analysis of Prospective Cohort Studies.J Stroke Cerebrovasc Dis. 2020 Apr;29(4):104659. doi: 10.1016/j.jstrokecerebrovasdis.2020.104659. Epub 2020 Feb 14. J Stroke Cerebrovasc Dis. 2020. PMID: 32067852
-
Association of Natriuretic Peptide With Adverse Outcomes and Disease Severity After Intracerebral Hemorrhage: A Systematic Review.Front Neurol. 2021 Nov 15;12:775085. doi: 10.3389/fneur.2021.775085. eCollection 2021. Front Neurol. 2021. PMID: 34867764 Free PMC article.
References
Publication types
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

